
The U.K. National Health Service (NHS) has appointed its first biomedical 3D technician, Heather Goodrum, to design and print maxillofacial guides, models, and inserts for use in surgery. The move shows how 3D printing of surgical prostheses is becoming a reality in routine practice, and hospital managers are keen to complement medical teams with digital design experts.
Until now, prosthetists and surgeons have been learning digital 3D design on the job, but the time has come for trained technicians to be involved in the screenwork, explained her colleague Peter Llewelyn Evans, a reconstructive scientist and Maxillofacial Laboratory Services Manager, at Morriston Hospital, part of Swansea NHS Trust.
 Heather Goodrum is the first biomedical 3D technician to be appointed to the U.K. NHS. Images courtesy of Abertawe Bro Morgannwg University Health Board and 3Dprintingindustry.com.
Heather Goodrum is the first biomedical 3D technician to be appointed to the U.K. NHS. Images courtesy of Abertawe Bro Morgannwg University Health Board and 3Dprintingindustry.com."Like many prosthetists, my role is patient-centered and my natural skills are in carving. These new digital skills constitute a hole in training," Evans said, adding that Goodrum has a master's degree in forensic reconstruction, is experienced in the same 3D modeling software used by the prosthetics department, and that other institutions are also searching for staff with skills in 3D design.
Evans noted that since the post was created, other big maxillofacial trauma units such as that at Queen Elizabeth Hospital in Birmingham, which receives army casualties and has its own 3D printer, and Leicester University Hospital, have also contacted Morriston Hospital with a view to creating similar positions on their own prosthetics teams.
Manipulating CT data
Goodrum's work entails taking the data from CT scans and manipulating the data using Belgian medical software Mimics, created by the Leuven-based company, Materialise. The software allows her to visualize the relevant cranial or facial structure in 3D and change the onscreen thresholds to pick out areas of interest on the CT scan such as soft or bony tissue. For the type of surgery undertaken in the unit, which usually involves bone reconstruction or bone-like inserts, MRI data is usually too fuzzy.
"We are reliant on radiologists to get the CT scan protocols right. Without accurate data from the CT, we couldn't create the CAD (computer-aided design) images that serve as the models for printing," Evans noted, adding that after the CT scan, the design work was solely the remit of the prosthetics team.
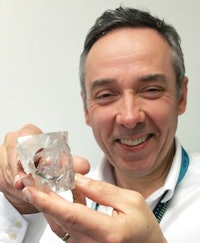 Without accurate data from CT, it would be impossible to create CAD models for 3D-printed inserts, said Peter Llewelyn Evans, shown here holding a 3D printed implant for an eye socket.
Without accurate data from CT, it would be impossible to create CAD models for 3D-printed inserts, said Peter Llewelyn Evans, shown here holding a 3D printed implant for an eye socket.The data are transferred from Mimics to Freeform, another type of software that allows 3D design modifications, before being transferred back to the Mimics program where designers can check in axial, coronal, and sagittal planes that the insert will fit perfectly in the area concerned. The model is then sent to another company, Renishaw, for 3D printing, usually in titanium, but also in polyether ether ketone (PEEK) or silicone, depending on the type of prosthesis.
Evans, who is also a founding member and secretary for the Centre for Applied Reconstructive Technologies in Surgery (CARTIS), pointed to one of the most common 3D-printed inserts for his patients: titanium orbital floors. In the case of a fractured orbital floor, a CT scan will be taken of the other "good" orbital floor, mirrored in CAD software, then manipulated to create a new orbital floor contour for the affected side, and printed.
Printed prosthetics also can be used in pediatric cases of microtia. For instance, a child who is missing an ear from birth can receive a 3D-printed artificial ear. This procedure involves scanning the existing ear so that a 3D silicone copy can be printed, which then clips onto a small implant placed into the existing earbone. The alternative would be surgical reconstruction, a difficult procedure due to the shortage of experts worldwide and the number of operations required.
When there is no intact or healthy side to a part, a scan from another similar patient will be used for creating the CAD images needed for 3D printing, he explained.
Advanced CAD methods
Design for cranial surgery is a large part of Goodrum's work. When part of the skull has been damaged or removed due to trauma or tumor surgery, the cranial contour can be directly replaced with a printed cranioplasty plate in PEEK or titanium. Furthermore, the Swansea team is branching into design and printing of prostheses for breast, hand, and finger -- and occasionally foot -- reconstruction. It also creates facial burns splints for occupational therapy patients.
The trend is in line with other moves toward 3D printing across Europe. In Germany, for example, Freiburg University Hospital's maxillofacial unit has gained a reputation as a key vanguard of advanced CAD for 3D-printed prostheses and inserts.
"We are a long way from the type of bioprinting envisaged 20 years ago, when scientists believed that doctors would take cells, and grow them into a body part to be inserted into the patient during surgery," Evans noted. "With the type of printing we are doing, although the bone will grow against the insert, the device will always remain a foreign part in biocompatible metal or plastic. It will be exciting when bioprinting becomes possible, but we need a huge jump in biomedical research and development."
While the evolutionary "great leap forward" in bioprinting has yet to occur, the era of prosthetic 3D printing is slowly advancing and gaining more territory in how it can be used in surgery. Designers can now directly print parts with complex structuring that mirror the anatomy of the patient. He believes the next step could be the seeding of these structures with stem cells to be implanted in patients, leading to unique tailored solutions for those with cancer, congenital abnormalities, and trauma patients.


















