A shear-wave ultrasound elastography method can be used to evaluate the stability of carotid plaques, helping to identify those that are most vulnerable to rupturing and causing a stroke, according to a study published in the June issue of the Journal of Ultrasound in Medicine.
Researchers from the First Affiliated Hospital of China Medical University in Shenyang, China, used shear-wave elastography to calculate the Young's modulus -- a measure of stiffness -- of carotid plaques in more than 60 patients. After retrospectively evaluating patient outcomes after six months, they found that patients who went on to have a stroke or transient ischemic attack within that time period had a lower mean Young's modulus score, indicating a more vulnerable plaque. In addition, the group found that the combination of the Young's modulus with the plaque's stenosis rate yielded the best diagnostic performance for identifying the plaques that became symptomatic.
"The [shear-wave elastography] technique is a noninvasive, vascular elastography technique that can provide information regarding carotid plaque vulnerability, and could be of clinical benefit to help identify symptomatic carotid plaques more comprehensively and to predict cardiovascular risk," wrote the team led by Dr. Zhe Lou.
Carotid plaque stability
The presence of carotid atherosclerotic plaques is a strong predictor of cerebrovascular events, and investigators are searching for noninvasive imaging and biochemical parameters that can accurately identify vulnerable plaques to prevent stroke. While the rigidity of a plaque can be calculated on shear-wave elastography via the Young's modulus stiffness measure, few studies have assessed its use for evaluating the stability of carotid atherosclerotic plaque. As a result, the researchers set out to evaluate the feasibility and clinical value of the technique in assessing the rigidity and vulnerability of carotid plaque (J Ultrasound Med, June 2017, Vol. 36:6, pp. 1213-1223).
Lou and colleagues retrospectively studied a total of 61 subjects with carotid plaques who had received carotid ultrasound from January to November 2015. Patients were excluded from the study if they showed disabilities caused by stroke, bilateral focal neurological symptoms, atrial fibrillation, vascular lesions, recent myocardial infarction, or severe congestive heart failure that could be the cardioembolic cause of cerebrovascular stroke.
To ensure that culprit plaques originated from the external cranial carotid artery, the researchers also excluded patients with moderate to severe stenosis of the intracranial artery, or with moderate to severe stenosis before the initial part of the carotid. Patients with radiation injury-associated stenosis, restenosis after endarterectomy, Takayasu arteritis, carotid artery dissection, or total carotid occlusion were also left out of the study.
The patients -- 45 men and 16 women -- were separated into two groups depending on whether they showed unilateral focal neurological symptoms within six months or if they were asymptomatic over that time frame. Of the 61 patients, 31 were in the symptomatic group; 16 had a nondisabling stroke and 15 had a transient ischemic attack. The remaining 30 were asymptomatic.
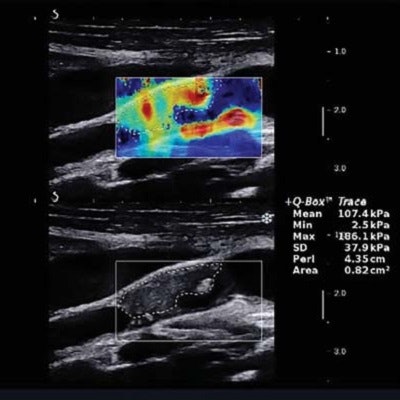
All patients received a clinical carotid ultrasound examination in conjunction with shear-wave elastography using an Aixplorer (SuperSonic Imagine) ultrasound scanner with a L10-2 MHz linear array transducer. Shear-wave elastography analysis was successfully carried out in 271 (92%) of the 295 plaques evaluated in the study, and the scanner's built-in Q-Box-Trace software tool was used to quantify the maximum, mean, and minimum Young's modulus values.
Finding vulnerable plaques
When confounding factors such as gender and smoking history were controlled, the researchers found a significant correlation between Gray-Weale plaque classification and mean Young's modulus (r = 50.728, p < 0.01). In addition, the mean Young's modulus of representative plaques in the symptomatic group was 81 kPa, compared with 115 kPa in the asymptomatic group. The difference was statistically significant (p < 0.01).
The researchers noted that the vulnerability of the whole plaque can be determined by calculating its Young's modulus measure on shear-wave elastography.
"The lower mean Young's modulus indicates a greater proportion of lipid cores, which could imply greater vulnerability than plaques with a higher fibrous content," they wrote.
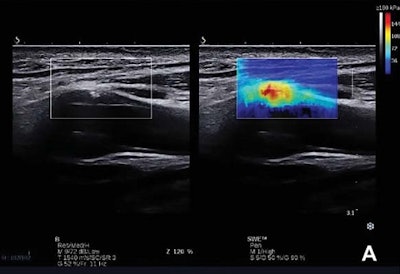 (A, above) Carotid plaque classified as Gray-Weale Type II shown with a B-mode and shear-wave elastography image. (B, below) The Young's modulus value of the plaque located in the anterior of the internal carotid artery was obtained using the Q-Box-Trace software tool. All images courtesy of the Journal of Ultrasound in Medicine.
(A, above) Carotid plaque classified as Gray-Weale Type II shown with a B-mode and shear-wave elastography image. (B, below) The Young's modulus value of the plaque located in the anterior of the internal carotid artery was obtained using the Q-Box-Trace software tool. All images courtesy of the Journal of Ultrasound in Medicine.What's more, logistic regression and receiver operating characteristic (ROC) analysis suggested that the combination of the mean Young's modulus with stenosis rate could yield increased sensitivity and specificity for identifying symptomatic carotid plaques, according to the researchers.
| Diagnostic efficacy of ultrasound parameters for differentiating carotid plaque | |
| Area under the curve | |
| Gray-Weale plaque classification | 0.760 |
| Mean Young's modulus | 0.871 |
| Stenosis rate | 0.880 |
| Gray-Weale classification and mean Young's modulus | 0.872 |
| Gray-Weale classification and stenosis rate | 0.901 |
| Stenosis rate and mean Young's modulus | 0.933 |
"Further studies are required to prove our initial findings and to extend the study to the assessment of the different Young's modulus values against other noninvasive imaging techniques and pathological staining, which could further confirm the clinical potential and value of the carotid plaque evaluation via [shear-wave elastography]," the authors wrote.










![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)




