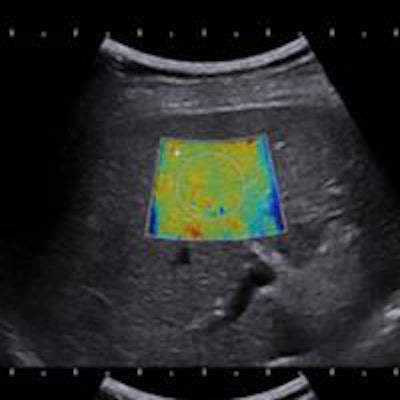
When assessing the current state of ultrasound elastography, Peter R. Hoskins, PhD, and Dr. William E. Svensson called 2012 the "early days" of shear-wave elastography (SWE), but reasoned that the technique's unique ability to quantify "true elastic modulus means that in time it will probably become the industry standard and henceforth the clinical standard."1 How has that prediction fared?
The answer is that SWE, a technology that can yield quantified measurements of tissue stiffness noninvasively, should have become the clinical standard already. Considering the continued characterization of SWE as an emerging technique, however, we may conclude this is not yet the case.2
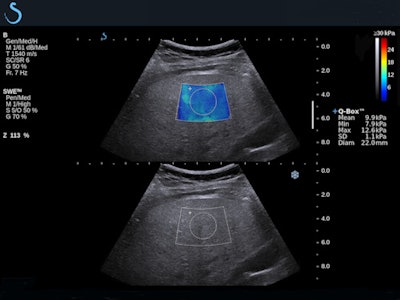 Fatty liver with shear-wave elastography shows stage F3 liver fibrosis.
Fatty liver with shear-wave elastography shows stage F3 liver fibrosis.Broader clinical acceptance typically follows after an application makes diagnosis indisputably easier for clinicians. An example of this trend in radiology is color Doppler, which was widely adopted only after it became clear that, for deep vein thrombosis, it afforded physicians greater diagnostic confidence.
The breakthrough for greater adoption of SWE is likely to come through investigation of liver fibrosis.
On the brink of change
Liver disease is a substantial health concern globally; in 2013, the WHO found the total deaths worldwide from cirrhosis and liver cancer rose by 50 million per year over two decades.3
To classify and stage diffuse liver diseases, including chronic hepatitis and cirrhosis,4 a noninvasive method would be preferred to the accepted gold standard: liver biopsy. There are two equally powerful reasons for this preference: first, liver biopsies suffer from sampling limitations that do not affect SWE, as biopsies only sample a very small portion of the liver; as the American Association for the Study of Liver Diseases notes, "in nearly all liver diseases, parenchymal abnormalities are irregularly distributed, and sampling variability is almost inevitable."5 Second, liver biopsies are painful, require in-patient hospital stays of up to three days, and carry a small risk of serious complications. SWE, on the other hand, saves patients time and anxiety, as the scan can be performed quickly and without any risk or discomfort for the patient.
Both of these reasons have financial aspects to consider as well. In the U.K., the National Health Service Technology Adoption Centre (NTAC) found that ultrasound elastography using the shear-wave technique is safer than the traditional liver biopsy. Opposed to biopsy, SWE's ease of use, quick exam time, reduced complications, and less patient pain would carry with it a savings of $20 million, NTAC found, if it were applied to all patients diagnosed with liver disease in England and Wales.6
Evaluating liver stiffness
Over the past decade, several studies have demonstrated the benefits of SWE for assessing liver stiffness quantitatively, noninvasively, and accurately.7 SWE has been shown to yield accurate diagnostic measurement of liver fibrosis in a range of patients, from hepatitis C patients to cirrhosis, including those with ascites.8
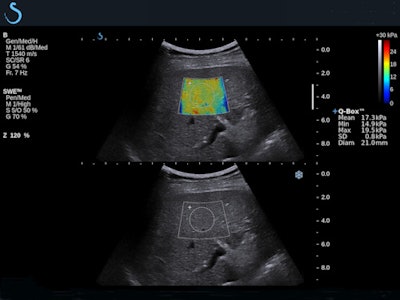 Shear-wave elastography demonstrates stage F4 liver fibrosis.
Shear-wave elastography demonstrates stage F4 liver fibrosis.One of the more recent studies found the moving images obtained this way accurately measured incidentally discovered liver lesions in patients with no history of liver disease; another found that SWE aided the detection of portal hypertension, a dangerous complication of cirrhosis.9 Two-dimensional images obtained noninvasively were especially important for monitoring the progression of liver disease in vulnerable patient populations such as those suffering from chronic viral hepatitis.
With the recent advent of highly effective antiviral therapy in patients with chronic hepatitis C, SWE can be used to monitor treatment response.
New guidelines available
One last factor, this one from within the medical-scientific community, should also help speed widespread use of SWE: the increasing circulation of the Guidelines and Recommendations on the Clinical Use of Ultrasound Elastography, compiled and published by the European Federation of Societies for Ultrasound in Medicine and Biology (EFSUMB) in 2013.
These guidelines distill the existing research on the various forms of ultrasound elastography and offer introductions to the fundamental principles of each technology. More importantly for clinicians, perhaps, the document includes concrete tips for performing scans with these technologies. The authors of each section share their experience working with specific technologies as well as providing a literature review of the studies pertaining to each ultrasound platform.
To explain the lag in adoption between the establishment of a modality's efficacy and its widespread use, clinicians tend to blame the glut of new medical technologies and their vast differences of quality and utility. They critique the studies supporting these tools, often rightly, as focused on too small a cohort or on a nonrepresentative sample.
In the case of SWE, these objections have been addressed by a diverse body of studies, focusing on the liver but also including SWE for evaluating the prostate, kidney, and breast.11,12 While those last areas may legitimately still be considered emerging applications for the technology, it is time for radiologists to make SWE a standard modality for assessing the liver.
Disclosures
Dr. Cosgrove is a member of the Scientific Board of SuperSonic Imagine.
Dr. David Cosgrove is a professor of clinical ultrasound at Imperial and King's Colleges in London.
The comments and observations expressed herein do not necessarily reflect the opinions of AuntMinnieEurope.com, nor should they be construed as an endorsement or admonishment of any particular vendor, analyst, industry consultant, or consulting group.
References
- Hoskins PR, Svensson W. Current State of Ultrasound elastography. Ultrasound, 2012;20(1):3-4.
- This 2015 study, for instance, refers to "newly emerging shear wave elastography techniques": Comb-Push Ultrasound Shear Elastography of Breast Masses: Initial Results Show Promise. PLoS One. 2015;10(3):e0119398.
- Tucker, Miriam E. Global Burden of Liver Disease Substantial. Medscape Multispecialty, Nov. 4, 2013. http://www.medscape.com/viewarticle/813788.
- Beland MD, Brown SF, Machan JT, Taliano RJ, Promrat K, Cronan JJ. A pilot study estimating liver fibrosis with ultrasound shear-wave elastography: Does the cause of liver disease or location of measurement affect performance? AJR Am J Roentgenol.2014;203(3):W267-73.
- Rockey, Don et al. Liver Biopsy, An Association for American Study of Liver Diseases Position Paper. Hepatology. 2009;49(3):1017-1044.
- http://www.healthcare-in-europe.com/en/article/11627-liver-fibrosis-emerges-as-a-breakthrough-for-elastography.html British pounds converted to U.S. dollars using: http://www.exchange-rates.org/converter/GBP/USD/.
- Ferraioli G1, Tinelli C, Dal Bello B, et al. Accuracy of real-time shear wave elastography for assessing liver fibrosis in chronic hepatitis C: A pilot study. Hepatology. 2012;56(6):2125-2133.
- Cosgrove, D. et al. EFSUMB Guidelines and Recommendations on the Clinical Use of Ultrasound Elastography. Part 2: Clinical Applications.
- Maxime Ronot, Sara Di Renzo, Bettina Gregoli, et al. Characterization of fortuitously discovered focal liver lesions: additional information provided by shearwave elastography. Eur Radiol. 2015;25(2):346-358.
- Quantitative Elastography of Liver Fibrosis and Spleen Stiffness in Chronic Hepatitis B Carriers: Comparison of Shear-Wave Elastography and Transient Elastography with Liver Biopsy Correlation. Radiology. 2013;269:910-918.
- Berg WA et al. Shear wave Elastography improves the specificity of breast US; the BE1 multinational study of 939 masses. Radiology, 2012:262(2):435-449.
Barr, R. et al. Shear Wave Ultrasound Elastography of the Prostate: Initial Results. Ultrasound Quarterly. 2012;28(1):13-20.



















