Virtual simulations of interventional and surgical procedures using open-source computer-aided detection (CAD) software is improving the accuracy of preoperative planning in corrective jaw surgery, German researchers have found.
Official German statistics for 2015 show that 43% of all medical errors happened in surgical departments, explained Johannes Haubold and colleagues from the Department of Diagnostic and Interventional Radiology and Neuroradiology at University Hospital Essen in Germany. Furthermore, preoperative planning continues to be mainly based on 2D datasets, which ignores the angle and the resulting distortion of the measured distances, and some procedures are planned on projection radiographic images, showing a significant distraction of the real anatomy.
"Simultaneously, CAD software in machine engineering is capable of precisely planning the assemblage of goods digitally in 3D with an extremely low discrepancy," they noted in an e-poster presentation at ECR 2017. "Some projects using CAD software for preoperative planning, mainly in orthognathic (corrective jaw) surgery, have already been realized, showing an enhancement in precision and effectiveness."
CAD and computer-aided manufacturing (CAM) have made it possible to adapt implants to the patient's anatomy, thereby improving the structural matching, Haubold continued, adding that preoperative planning with CAD/CAM is only possible with specialist software that works with a short range of anatomical structures and implants, such as for hip replacements. As a result, CAD-based preoperative planning is not yet integrated into day-to-day surgical practice.
Novel use of dual-energy CT
To make CAD-based preoperative planning more accessible, the team developed an open-source method using 3D datasets of preoperative CT scans for a virtual simulation of an implantation. They wanted to show that CAD-based planning could be done with every implant using dual-energy CT.
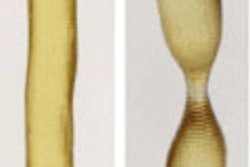
The researchers acquired 3D models of osteosynthesis materials using high-resolution dual-energy CT scans on a Somatom Definition Flash and Force (Siemens Healthineers) machines with a space resolution of 0.125 mm and a layer thickness of 1.5 mm. They were keen to make full use of dual-energy CT to improve the image quality of 3D models of patients' anatomy rendered using the preoperative CT scans.
"In most cases, lowering the layer thickness of day-to-day business CT scans resulted in an accelerated image noise, lowering the quality of the 3D models," Haubold and colleagues observed.
To increase the range of possible implants and the accessibility, they adapted existing open-source methods of 3D model acquisition. They used 3D Slicer, an open source multiplatform software package for visualization and 3D rendering of CT and MRI datasets. It is open for commercial use and third-party developers under a Berkeley Software Distribution (BSD)-style license.
The group cropped the target volume using the crop volume tool within the 3D Slicer, and then labeled the target structure by marking the voxels with a specified Hounsfield unit (HU), e.g. 300-1,500 HU for bones using the editor of the package.
Open-source CAD software
To simulate an implantation, they imported those 3D models into open-source CAD software called FreeCAD. FreeCAD is published under the GNU Lesser General Public License (LGPL), and is open to third-party developers and free of charge for commercial use. They imported the stereolithography files of the patients' anatomy into a new project, after which they added different osteosynthesis materials and virtually implanted them into the patients' anatomy.
"Three-dimensional models of patients' anatomy and osteosynthesis materials could be rendered and exported as stereolithography files using open source 3D-rendering software. Using the stereolithography files, precise computer-aided preoperative planning in 3D could be done using open source CAD software," they wrote.
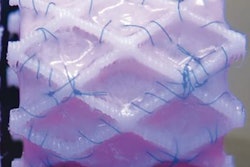
In addition, the stereolithography files were printed with a 3D printer for a physical simulation of operative procedures. If preoperative planning in 3D with CAD software can lower the perioperative morbidity and mortality, the full details must be shown, Haubold and colleagues noted.
Looking to the future, they anticipate that open-source virtual 3D fusion will make CAD planning more widely available.
To view their clinical cases presented at ECR 2017, click here.










![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)





