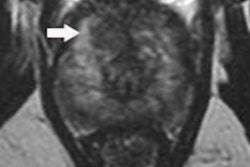
Abstinence from ejaculation prior to a prostate MR examination significantly increases the volume of seminal vesicles (SVs), and thereby may well improve evaluation of SV invasion on multiparametric MRI, especially in older men, according to new research from Turkey and the U.S.
The study involving 238 patients sought to establish the impact of preimaging abstinence on the diagnostic accuracy of MRI. The results showed that abstinence improved image interpretability, particularly in men older than 60 years of age, raising important questions about what recommendations should be made to patients ahead of MRI prostate exams.
 Abstinence from ejaculation is not a "must" for men younger than 60 undergoing prostate MRI, Dr. Ismail Kabakus said.
Abstinence from ejaculation is not a "must" for men younger than 60 undergoing prostate MRI, Dr. Ismail Kabakus said.The authors of the article, published online by American Journal of Roentgenology on 26 September and scheduled for inclusion in the December 2016 edition, highlighted how early detection and staging of prostate cancer is crucial to patient management and this includes assessing SV invasion. This study into the impact of abstinence on the diagnostic value of multiparametric prostate MRI is an important milestone in prostate cancer imaging, but larger-scale studies are needed to understand the impact of age, race and ethnicity, prostate-specific antigen (PSA) levels, and medications, they explained.
In Turkey, there is growing awareness of prostate cancer among Turkish men, and prostate imaging, especially by MRI, tends to be well accepted, noted lead author Dr. Ismail Kabakus, a radiologist at Hacettepe University Hospital in Ankara. However, he pointed out the need to abstain from ejaculation can cause extra stress to patients.
"Although abstinence from ejaculation is included in preimaging protocols for prostate MRI for better evaluation of seminal vesicles, our results showed that it is not a must, especially for patients under 60," he said. "This makes the preimaging protocol easier and more comfortable for patients who are already anxious because of their upcoming prostate examination."
He believes that three-day abstinence from ejaculation is more likely to remain a suggestion rather than a requirement.
"Seminal vesicles shrink with age," he added. "Our study showed that for patients over 60, refraining from ejaculation prior to prostate MRI examination is strongly recommended in order to have enough distension for evaluation."
The retrospective U.S. National Institutes of Health study involved 238 patients who underwent 3-tesla MRI of the prostate between June and September 2015. Patients were asked to complete a questionnaire to estimate the number of days since their last ejaculation (< 3 days versus ≥ 3 days) and were divided into two groups accordingly.
For men older than 60, abstinence for three or more days before undergoing MRI resulted in larger SV volumes and lower rates of nondiagnostic evaluation. This was observed to a lesser extent in men younger than 60. The key findings are shown below. Percentages are rounded, according to Kabakus and colleagues. Two-figure ranges were provided by two radiologist readers.
| Abstinence less than 3 days (g1 = 42) | Abstinence 3 days or more (g2 = 42) | |
| SV vol | 6 mL | 8.8 mL |
| Mean interpretability | 2.0 | 2.5 |
| Nondiagnostic (N/d) scores | 10-13 (23.8% to 31%) | 2-5 (4.7% to 11.9%) |
| N/d for men over 60 | 9-11 of 25 (36% to 44%) | 2-5 of 26 (7.6% to 19.2%) |
| N/d for men 60 & under | 1-2 of 17 (5.8% to 11.7%) | 0 of 16 (0%) |
Specifically, 42 patients (mean patient age, 62.0 years, mean [± standard deviation] PSA level, 10.1 ± 2.1 ng/mL) indicated it had been less than three days since their last ejaculation and were designated as group 1, whereas the remainder indicated an interval of three days or more since their last ejaculation. Because age impacts SV volume, a group of 42 age-matched subjects (mean patient age, 62.1 years, mean PSA level, 7.0 ± 0.6 ng/mL) were randomly selected from the remaining 196 patients and were designated as group 2.
SV volumes were measured manually. To clarify if the statistically significant volume differences had a meaningful effect on diagnostic interpretability, two readers were asked to judge the interpretability of the SVs. Two radiologists who were blinded to group assignment and patient characteristics scored the right and left SVs separately to determine diagnostic interpretability, using a three-point scale: A score of 1 denoted the SVs were not dilated and the score was nondiagnostic; a score of 2 indicated the SVs were not dilated but the score was diagnostic; and a score of 3 denoted the SVs were dilated and the score was diagnostic.
Interobserver agreement was analyzed using the Cohen kappa statistic and found to be good (0.7). A separate analysis was performed to evaluate differences in diagnostic interpretability for patients 60 years and younger versus patients older than 60.
Results
The right, left, and total SV volumes for group 1 were 3.1 mL, 2.9 mL, and 6.0 mL, respectively, whereas those for group 2 were 4.7 mL, 4.1 mL, and 8.8 mL, respectively (p = 0.011). The mean interpretability scores for group 1 and group 2 were 2.0 and 2.5, respectively. For group 1, reader 1 and reader 2 assigned a nondiagnostic score for 10 and 13 patients (23.8% to 31%), respectively, whereas for group 2, they assigned a nondiagnostic score for two and five patients (4.75% to 11.9%), respectively (p = 0.01, for reader 1; and p = 0.03, for reader 2).
Failure to abstain from ejaculation for three days or more increased the risk of nondiagnostic scan results for the SVs, and this was higher in men older than 60 who did not refrain from ejaculation for three days or more, increasing 2.4-fold to 4.7-fold: For men in group 1 who were older than 60, reader 1 and reader 2 gave a nondiagnostic score for nine and 11 patients (36% to 44%) of 25, respectively; whereas for men in group 2 who were older than 60, the readers gave a nondiagnostic score for two and five patients (7.6% to 19.2%) of 26, respectively (p = 0.01, for reader 1; and p = 0.05, for reader 2).
For men 60 years and younger, reader 1 and reader 2 assigned a nondiagnostic score for respectively one and two of 17 patients in group 1 (5.8% to 11.7%); both readers assigned a nondiagnostic score of 0 for 16 patients in group 2 (p = 0.325, for reader 1; and p = 0.157, for reader 2).
Version 2 of the Prostate Imaging and Reporting Data System, the most recent recommendations for prostate MRI, confirms many radiologists have adopted the practice of urging abstinence prior to MRI, but the system does not fully endorse the practice, the authors stated. The findings may trigger further debate about whether a three-day abstinence should be recommended more firmly -- and widely -- in instructions given ahead of MRI prostate exams to patients older than 60, and whether this recommendation should be downplayed in younger patients.
"Because there is no cost, and because men receive similar instructions before samples are acquired for PSA tests, abstinence is an easily implemented patient preparation procedure which may improve the diagnostic value of multiparametric MRI, especially in men older than 60 years," Kabakus and colleagues concluded.