
New analysis from Germany supports a dramatic change in the management of patients with ongoing chest pain and psychological problems after angiographic exclusion of heart disease. Its results call into question repeat or further investigative procedures that might not diagnose a somatic cause for chest pain.
The study examined the incidence of mental symptoms in patients with angiographic exclusion of coronary heart disease. Around 20% of patients with chest pain have normal coronary angiograms, according to lead author Dr. Marian Christoph, from the Heart Centre University Hospital at the University Hospital of Dresden.
The pain may be a psychosomatic symptom related to mental health, and this may not always be considered adequately by healthcare professionals. Moreover, because surplus investigations burden both the patient and the health system, this study could prove a useful tool for reducing costs while optimizing the care of such patients through the initiation of early psychosomatic therapy.
Fast and easy-to-implement psychosomatic screening could prove crucial to the care of patients with noncardiac chest pain, the study claims. Although the authors stop short of suggesting that such screening should replace repeat imaging and other investigative techniques, they believe that its wider and earlier implementation in patients with normal angiograms would be beneficial (Open Heart, 3 November 2014).
"It is probably possible to prevent redundant somatic diagnostics and treatment and to improve the quality of life of these patients significantly," they wrote. "As a psychosomatic screening tool, the use of the standardized and validated questionnaires was very practicable, even for cardiologists without psychosomatic training."
The study took place over a year and involved 253 patients who had to be 18 years of age or older and native German speakers. Medical eligibility criteria included exclusion of relevant coronary artery disease in coronary angiography; preserved left and right ventricular systolic function; exclusion of valvular heart disease in echocardiography; and presence of at least one of the three following cardiac symptoms: chest pain, dyspnoea, and/or palpitations.
Reasons for exclusion were relevant coronary artery disease, hemodynamic relevant valvular heart disease, decreased ventricular ejection fraction, and documented cardiac arrhythmia.
The type and intensity of their symptoms were evaluated before and after coronary angiography.
The incidence of psychopathological symptoms was quantified by standardized questionnaires such as general anxiety and depression (Hospital Anxiety and Depression Scale, HADS), heart-focused anxiety (Cardiac Anxiety Questionnaire, CAQ), hypochondria (Whitely Index), somatoform disorder (Screening for Somatoform Disorders, SOMS), and quality of life (12-item Short Form Health Survey, SF-12). The incidence of psychological symptoms in these patients was compared with incidence in the normal population.
All identified patients who had an angiographic exclusion of coronary heart disease within the previous year (from January to December) received the questionnaires by mail the following June, six to 18 months after the coronary angiography. From the cohort, 70% continued to suffer cardiac symptoms.
General anxiety increased by 37% in women and by 22% in men compared with the normal population. Heart-focused anxiety was raised by 27%, and somatoform disorders appeared 120% more often in patients after cardiac catheterization in comparison with the normal population. Furthermore, increased psychological symptoms were mirrored in perception of a significantly lower quality of life in patients with inconspicuous coronary angiography.
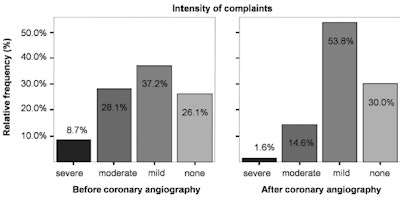 Relative frequency of complaint intensity (%). Source: Open Heart, 3 November 2014.
Relative frequency of complaint intensity (%). Source: Open Heart, 3 November 2014.Overall, the study suggests that patients with cardiac symptoms and normal coronary arteries more often suffer from mental symptoms compared with the healthy population. According to the authors, these results support the opinion that patients with noncardiac chest pain should receive a psychological or psychiatric examination in order to initiate appropriate psychosomatic therapy early, if necessary.
Entire psychosomatic screening consists of 98 questions. The complete filling out of all items requires about 120 minutes per patient, a time frame "acceptable" for inpatients as well as for outpatients, the authors state.
"The analysis of these questionnaires takes about 15 minutes and can also be performed by nurses. Taken together, the time required for this diagnosis is justified," they noted.
Study limitations
Christoph et al point to some of the study's shortcomings. The results are based on subjective ratings from questionnaires, which limit interpretability, and some questions cannot be answered adequately; i.e., it is not clear whether the psychopathological symptoms cause the cardiac symptoms or if the cardiac symptoms provoke the psychopathological disorders.
Another unresolved fact is whether or not psychosomatic therapy can improve the outcome and the quality of life in these patients. However, the authors cite recent works that show the prognosis of patients with heart-focused anxiety can be improved with the help of cognitive-behavioral therapies, though whether these therapies additionally decrease the overuse of the healthcare system remains unclear.
The authors see a real potential role for early psychosomatic therapy initiation for a significant number of chest pain patients.
"Patients with angiographic exclusion of a coronary artery disease have a significantly increased incidence of mental symptoms compared to the healthy population. Therefore, a psychosomatic diagnostic should be performed early in these patients," they concluded. "These diagnostic tools may prevent repeated utilization of the healthcare system and this could help to reduce costs."







![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)






