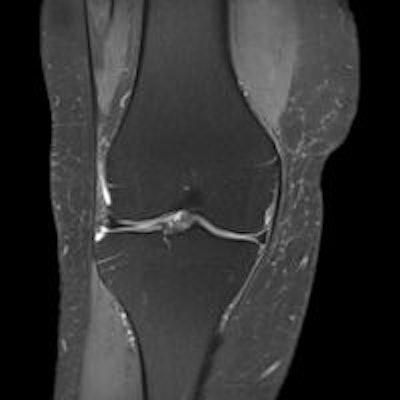
Prize-winning researchers from Pamplona, Spain, have devised a practical system for reading knee MRI scans that can help to improve efficiency, both in terms of speed and accuracy of detection of knee pathology. It may prove particularly beneficial for newcomers to the field.
In an e-poster that received one of the three winners' awards presented at the annual meeting of the European Society of Musculoskeletal Radiology (ESSR) held at the end of June in Riga, Latvia, the group proposed a systematic reading of knee MRI examinations. They suggested using the following order: meniscus, bone, ligaments, tendons, articular space and soft tissue, and second look.
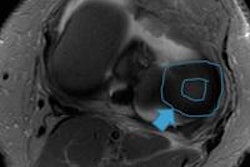
The meniscus should be the first step when evaluating knee MRI studies because of the importance and prevalence of meniscal pathology, according to lead author Dr. José María Bondía Gracia, a musculoskeletal radiologist at Clínica Universidad de Navarra in Pamplona. Its morphology requires great concentration for an appropriate assessment, and at the beginning of the study, the radiologist is less tired, making concentration easier.
"Meniscus' pathology is highly prevalent and can be treated effectively in most cases. Therefore, proper evaluation is really profitable. That is one of the main reasons why the systematic reading of the knee is usually started with the evaluation of meniscus," he noted.
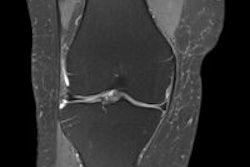
Gracia added that the sagittal plane is the most suitable projection for distinguishing meniscal tears and the axial plane is the worst for assessing the meniscus because it is affected by partial-volume effect, though it can be important in radial tears and bucket handle displacement. The development of 3D MRI sequences can be a great tool for this projection.
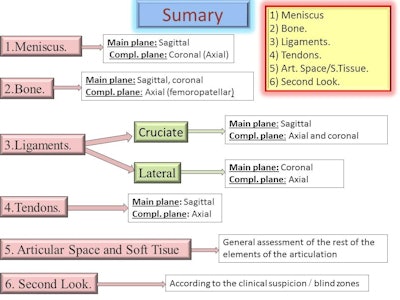 Workflow for knee MRI examinations proposed by Dr. José María Bondía Gracia. Source: ESSR 2014, e-poster P-0027, MRI of the Knee: A Proposal for a Systematic Reading.
Workflow for knee MRI examinations proposed by Dr. José María Bondía Gracia. Source: ESSR 2014, e-poster P-0027, MRI of the Knee: A Proposal for a Systematic Reading.The knee is composed of multiple structures, each with its own directional and spatial features; the reading of knee MRI exams is more effective when these structures are analyzed individually and following a particular order than when analyzed as a whole. A systematic reading that considers anatomical elements is more useful than going through the different images and sequences, the authors explained.
As for nonspecific clinical presentation of the knee, similar symptoms may correspond to different pathologies, and it requires a complete visualization of all structures of the knee, or at least the most important ones, in order not to miss what's pathological, according to the researchers.
For a proper assessment, it takes at least two planes in each structure: a start-up, where you see the structure more fully, and a complementary plane, or planes, in another space/direction. For oblique structures, three planes are required, as with cruciate ligaments, they added.
Also, it is important to assess the articular cartilage, and when predicting how the meniscus will be repaired in surgery, it is useful to know whether there is an impairment of the underlying cartilage. The existence of subchondral bone edema is a sign that could indicate chondral injury, and the presence of edema may help to diagnose a meniscal tear.
"It (the coronal plane) helps to check what we've seen in the sagittal plane. You can see small tears (especially vertical) not visible or difficult to see in the sagittal plane. It complements the criteria of contact of intrameniscal signal with superior or inferior surface of the meniscus in two slices," the authors stated. "At this level, we can evaluate meniscal insertions that are not typically seen in sagittal."
Evaluation of bone edema is the second step in knee MRI because the focus contusive pattern helps in the assessment of possible associated injuries. Furthermore, bone edema is an indirect sign of other diseases such as cartilage pathology or insertional pathology. They recommend caution, however, because the red bone marrow can simulate edema, and the key point is it is never in the epiphysis; the bone marrow, even very prominent, does not affect the epiphysis, they added.
When an anterior cruciate ligament (ACL) injury has been diagnosed, a second look is essential to check for meniscal tears (vertical tears of the medial meniscus, rupture of the posterior horn of the lateral meniscus), and injuries to the posterolateral corner. In addition to the relative frequency associated with an ACL injury, a radiologist often misses the findings, which are important in the prognosis and from a therapeutic point of view, concluded the authors.