Bone metastases are common in patients with advanced cancer, causing severe pain and rapid degradation in quality of life. Such metastases are usually treated using radiation therapy, but this isn't suitable, or successful, for all patients. Now, an international research team has shown that there may be another option: MR-guided focused ultrasound (MRgFUS).
Focused ultrasound is a noninvasive tissue ablation technique that uses acoustic energy to heat lesions to ablative temperatures of more than 65° C. Adding MR guidance confers additional advantages, including high-resolution imaging of the targeted tumor and surrounding anatomy, real-time MR thermometry during treatment to ensure adequate ablation temperatures while respecting normal tissue tolerances, and immediate post-treatment validation of the extent of ablation.
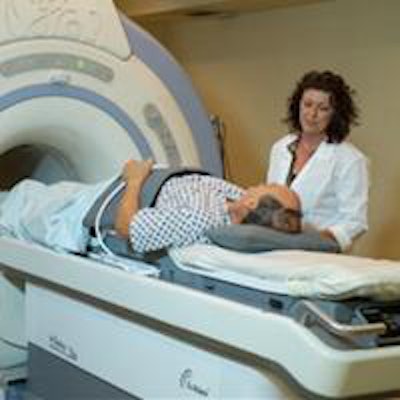
 The ExAblate MR-guided focused ultrasound system, from Israeli firm InSightec, is used for pain palliation of bone metastases.
The ExAblate MR-guided focused ultrasound system, from Israeli firm InSightec, is used for pain palliation of bone metastases.MRgFUS has previously been used to treat thousands of women with uterine fibroids, with excellent safety and efficacy profiles. This latest work represents the first completed phase III study to use the technology for cancer treatment, said principal investigator Dr. Mark Hurwitz from Thomas Jefferson University in Philadelphia. Hurwitz and colleagues performed the randomized controlled trial to evaluate the safety and efficacy of MRgFUS for palliation of pain due to bone metastases (Journal of the National Cancer Institute, 23 April 2014, Vol. 106:5, pii: dju082).
Blinded trial
The phase III study included 147 patients from 17 centers in the U.S., Canada, Israel, Italy, and Russia. Participants had bone metastases that were painful despite previous radiotherapy, or were not candidates for or declined radiotherapy. The patients were randomly assigned to receive MRgFUS (112 subjects) or placebo treatments (35 subjects).
The researchers created treatment plans for each patient, to precisely target ultrasound to their bone tumors while avoiding damage to nontargeted tissue. After verifying correct positioning using low-energy sonications, they used the ExAblate MRgFUS system from InSightec to heat lesions to ablative temperatures of between 65 and 85° C. Patients randomized to placebo underwent the same procedure but without ultrasound energy deposition.
The study's primary endpoint was improvement in self-reported pain score, without an increase in pain medication, three months after treatment. Specifically, a patient whose highest numerical rating scale (NRS) for pain decreased by at least two points and whose morphine equivalent daily dose did not increase by more than 25% was considered a responder; otherwise, they were considered a nonresponder.
 Principal investigator Dr. Mark Hurwitz from Thomas Jefferson University.
Principal investigator Dr. Mark Hurwitz from Thomas Jefferson University.
The study met its primary endpoint, with 64.3% of patients in the MRgFUS arm designated as responders, compared with 20.0% in the placebo arm. In the MRgFUS group, 23.2% of participants had a complete response (worst NRS of zero by trial end), while 5.7% in the placebo arm had a complete response. Response to MRgFUS was typically rapid, with about two-thirds of patients experiencing pain relief within days of treatment.
The researchers also observed a statistically significant difference in change from baseline in the worst NRS, with a mean reduction of 3.6 ± 3.1 points in the MRgFUS group and 0.7 ± 2.4 points in the placebo group. Additionally, 47% of patients treated by MRgFUS reduced (21%) or completely stopped (26%) their pain medication.
The most common treatment-related adverse event was sonication pain, which occurred in 32.1% of sonicated patients. In addition, two patients had pathological fractures, one had third-degree skin burn, and one suffered from neuropathy. Overall, 60.3% of all adverse events resolved on the treatment day, with an additional 14.3% resolving within one week.
The authors concluded that their study results support previous findings, with MRgFUS providing durable pain relief and improved function in patients who had failed, or were not candidates for, radiation therapy. They note that MRgFUS should be considered a viable treatment option for painful bone metastases, and that further studies are required to assess its role as a first-line therapy.
© IOP Publishing Limited. Republished with permission from medicalphysicsweb, a community website covering fundamental research and emerging technologies in medical imaging and radiation therapy.