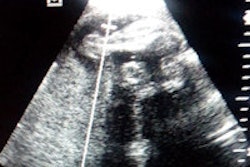
A recent study has shown that providing pregnant women in rural Uganda with access to ultrasound screenings resulted in overall improved quality of maternal and newborn care.
The study showed increases in the number of women attending prenatal visits and in husbands taking a more active role in health choices surrounding pregnancy. It also showed a near-doubling of newborns delivered by skilled healthcare workers (PLOS One, October 30, 2013).
The research was sponsored by Imaging the World and funded in part by Philips Healthcare's parent company, Royal Philips Electronics.
Imaging the World, in collaboration with Royal Philips, began a program in 2010 to provide access to basic prenatal ultrasound at Nawanyago Health Centre III in Uganda. Under this program, midwives were trained in the Imaging the World ultrasound screening protocol, and the resulting increase in prenatal care visits allowed for opportunities to educate women on safe birthing and home-care practices.
Since the program began, midwives have diagnosed previously undiagnosed complications such as placenta previa, breech presentation, multiples, molar pregnancy, and low fluid levels, and patients requiring hospital care were referred to district and regional hospitals.
Dr. Andrew Ross, of the University of Vermont College of Medicine, and colleagues analyzed the number of prenatal visits and deliveries during the 42 months prior and 23 months after the introduction of ultrasound at Nawanyago Health Centre III, comparing the center's outcomes to a clinical control site. Following the introduction of ultrasound, the number of deliveries at the clinic increased by 60% and the average number of prenatal visits increased by 73%, Ross' group found.
"One difficulty the clinic has faced is getting women to return for all four recommended antenatal visits," said Dr. Kristen DeStigter, co-founder of Imaging the World, in a statement released by Philips. "After the ultrasound program was introduced, the number of women coming back for the full four visits recommended by the World Health Organization nearly quadrupled. That represents a tremendous increase in the number of women getting appropriate care during pregnancy, especially during the latter stages."










![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)





