It has been more than four years since Dr. Christiane Kuhl and colleagues published a landmark paper in The Lancet that advocated the use of MRI as a distinct method to detect breast cancer in its earliest stage, instead of as an adjunct to mammography. Yet during a pre-congress symposium at ECR 2011, fewer than 10% of her colleagues raised their hands in response to her question: "How many of you are using MRI?"
 Dr. Christiane Kuhl, from Aachen, has been a keen advocate of breast MRI for the past 16 years.
Dr. Christiane Kuhl, from Aachen, has been a keen advocate of breast MRI for the past 16 years.
"Okay, some of you are doing it at least," she said.
Following the session, Kuhl explained she has been preaching the same message for the past 16 years, since 1995.
"I can only urge people that MRI is the most potent breast imaging tool," she said. "People are constantly developing new tools like tomosynthesis and elastography, but every time the diagnostic accuracy of such a technique is investigated, they compare it to MRI. This is an implicit acknowledgement of the fact MRI is considered the gold standard, the reference standard for breast cancer diagnosis. Which is why I would ask, why not use MRI rightaway, in the first place?"
Kuhl, head of the department of diagnostic and interventional at Aachen in Germany, advocated the greater use of MRI in breast cancer diagnosis during three sessions at ECR 2011. She provided an update on the MRI BI-RADS system from the American College of Radiology (ACR), where she serves as one of the faculty members, and argued for "Breast Cancer Screening with MR Imaging and Nothing Else," in a forward-looking panel discussion about Breast Imaging in 2025.
Yet, it was the day before ECR 2011 officially opened, during the annual meeting for the European Society of Breast Imaging (EUSOBI), that Kuhl presented her most powerful arguments. High-grade ductal carcinoma in situ (DCIS) is a non-obligate but direct precursor of high grade invasive cancer -- a cancer that may kill, she told her fellow breast specialists.
Her studies show that the disease is identified by mammography in only 52% of cases compared to 98% for MRI. The implications of these finding are clear: A large-scale multicenter breast-screening trial with MRI in the general population is essential. The prevention of high-grade invasive cancer, through diagnosis and treatment of high grade DCIS, is critical to the survival of patients, she said.
"My message is that one should keep MRI really simple," she said. "Instead of making people afraid of this technique by propagating multiparametric imaging, CAD systems, color codings, and multi-compartment modeling. I recommend to just use your mammographic commonsense, some easy-to-learn principles, and to get some personal experience with MRI before you start."
Kuhl demonstrated this point at the end of her presentation on the MRI BIRADS criteria in the ECR symposium, leading breast specialists through a series of case studies. Like a professor at medical school, she showed image after image, challenging colleagues to distinguish lesions from non-malignant structures. Like a well-trained class, the radiologists chanted in unison their responses, for the most part correct.
"It is difficult to understand why people make such a fuss around interpreting MRI; it is easy!" she said. "My first recommendation is: Use a pulse sequence that is 'conservative,' that does not exaggerate enhancement. Take, for example, the pulse sequence that we've used for 16 years. Do not get fooled by people who want to convince you to use 'advanced' technology such as active fat suppression, isotropic imaging, parallel image acquisition, high field MRI, fancy k-space read out technologies, and the like. Then, my second recommendation is: Stay relaxed. If you start doing breast MRI, only call something suspicious if it really looks like cancer."
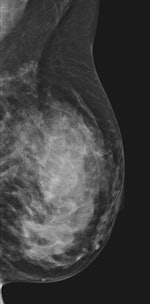 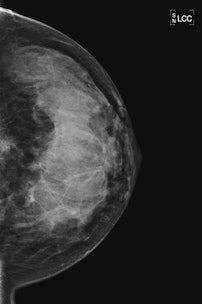 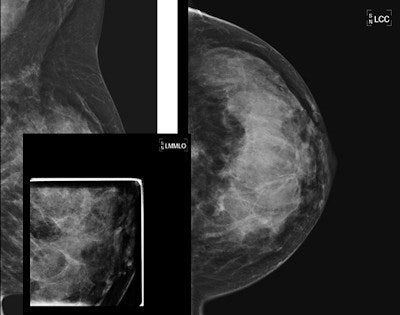 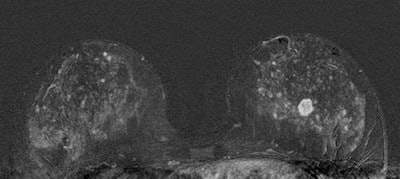 |
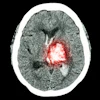
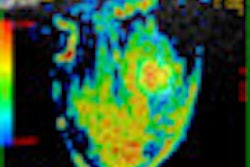
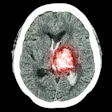
| 45-year-old asyptomatic woman with family history of breast cancer underwent mammography and MRI for screening. Full field digital mammogram is normal. Coned down view was done after MRI. MRI depicts a well circumscribed tumor with fast and early enhancement, strong wash out, and peripheral (rim) enhancement. This is high grade invasive cancer (basal-like) without calcifications; even coned down view is unremarkable. All images courtesy of Dr. Christiane Kuhl |