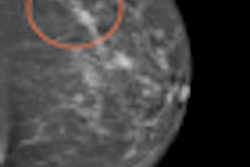
VIENNA - A low recall rate in combination with the introduction of digital mammography affects the balance between recall rate and detection rate, which can influence breast cancer care and the associated costs, according to a European Congress of Radiology (ECR) session on Friday afternoon.
Many countries have already switched to digital mammography for their breast cancer screening program, but for those who have not, a study out of the Netherlands demonstrates how recall rates may spike before eventually leveling out.
The Netherlands has a low recall rate (1.5%) compared to other European population-based breast cancer screening programs, while maintaining similar breast cancer detection and low breast cancer mortality rates. Once digital mammography was introduced in 2007, the recall rate increased, according to a presentation by Janine Timmers, a doctoral student student and scientific researcher at the National Expert and Training Centre for Breast Cancer Screening in Nijmegen, the Netherlands.
Close to 1,000 women (988) from Nijmegen were included in the study from the years 2000 to 2007. All of them received analogue mammography and 75% received digital. The average recall rate increased from 15 to 34 per 1,000 women screened with the introduction of digital, the researchers found. Also, the number of breast cancers detected increased from 5.5 to 7.8 per 1,000 screens, whereas the positive predictive value fell from 37% to 23%.
"Digital mammography improved detection: We found approximately an additional 1,500 breast cancers per year," Timmers said.
The researchers also found an increase in diagnostic workup procedures and total diagnostic costs. However, costs of a single workup slightly decreased as fewer surgical biopsies were performed.
This study has important implications for other countries making the switch to digital mammography as they may experience similar results, the session's moderator said.
The recall rate in the Netherlands is now comparable to that of other countries, Timmers said.