A new study from Germany involving more than 17,000 refugees has shown mass tuberculosis (TB) screening by chest x-ray (CXR) is inefficient due to the high number required to detect active pulmonary TB. In a migrant population in which TB prevalence is low, a more targeted approach to screening may be useful.
The study, published online in European Radiology on 3 January 2017, aimed to show the prevalence of TB, the number needed to screen, and the diagnostic accuracy of CXR screening to detect active pulmonary TB during the 2015 European refugee crisis. This involved the evaluation of data from all refugees who underwent CXR screening in the Hamburg metropolitan area in 2015, and comparison with all definite TB cases registered at the Department of Public Health.
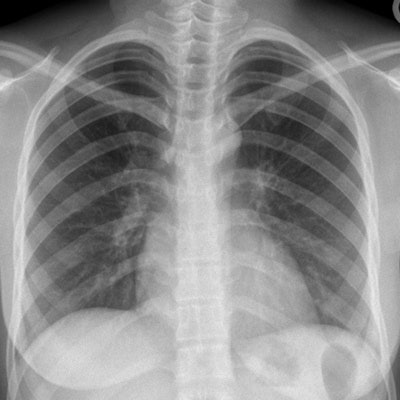
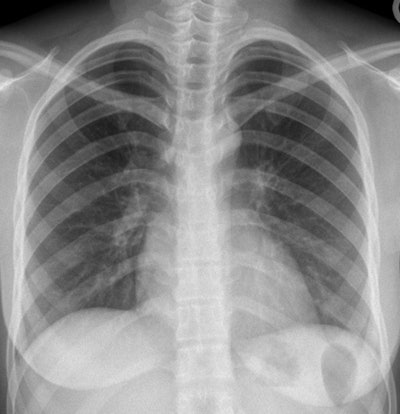 This CXR of a 26-year-old female Afghani refugee was normal at screening, but she was later diagnosed with pulmonary TB. Image courtesy of Dr. Julius Weinrich.
This CXR of a 26-year-old female Afghani refugee was normal at screening, but she was later diagnosed with pulmonary TB. Image courtesy of Dr. Julius Weinrich.TB is a leading cause of death worldwide, and migrants are generally considered to be a high-risk group for carrying it. By law in Germany, all nonpregnant female and all male immigrants older than 15 and to be admitted to shared accommodation sites are obliged to undergo TB screening by CXR.
Yet this study's comparatively high number needed to screen and low sensitivity has thrown into doubt the usefulness of general TB screening by CXR. According to the authors, a recent meta-analysis of screening programs for different risk groups established the overall median number needed to screen using CXR as a primary screening algorithm at 156 (range 66-320), tenfold lower than the number needed to screen in this study, calculated at 1,749.
This indicated that nontargeted CXR screening for TB had low yield during the 2015 crisis, and has highlighted the need to predefine risk groups for screening programs, the authors noted.
A total of 17,487 immigrants (13,465 males; 4,022 females) with an average age of 29.6 ± 11.8 years underwent single-center CXR screening between 1 January and 31 December 2015 in Hamburg. All CXR-screened refugees were included in the study.
The key findings are summarized in the chart below.
| No. of refugees CXR screened for active TB = 17,487 | |
| Prevalence of active pulmonary TB | 0.1% |
| CXR sensitivity | 55.6% |
| CXR specificity | 98.3% |
| No. needed to be screened | 1,749 |
| PPV | 3.3% |
| NPV | 100% |
| No. of cases of confirmed active pulmonary TB | 18/17,487 (0.1%) |
| Active pulmonary TB diagnosed by CXR | 10/18 (55.6%) |
| All (pulmonary & extrathoracic) TB missed by CXR | 16/17,487 (0.9%) |
| Pulmonary TB missed by CXR | 8/17,487 (0.5%), overall 8/18 (44.4%) in pulmonary TB cases |
Overall, the prevalence of definite active pulmonary TB in the screened population of 17,487 refugees was 0.103% (18 cases). The number needed to screen for detecting one case of active pulmonary TB was 1,749. CXR screening sensitivity was 55.6% (CI 30.8-78.5%), specificity was 98.3% (CI 98.1-98.5%), positive predictive value (PPV) was 3.3% (CI 1.6-5.9%), and negative predictive value (NPV) was 100% (CI 99.9-100%).
Pulmonary TB was present in 30 of the 40 (75%) immigrants with definite TB and in 18 of 26 (69%) of CXR-screened refugees.
Evidence of active or prior pulmonary TB was found in 306 CXR examinations (306:17,487; 1.75%) Active TB was confirmed in 10:306 (3.3%) with findings suggestive of TB, and all individuals having symptoms such as cough or fever at the time of screening. The remaining 296 refugees were considered false positives. This resulted in a number needed to screen of 1,749 (10:17,487) to detect one case of active TB.
Missed diagnoses
Twenty-six of the 40 refugees (65%) with bacteriologically confirmed TB participated in the screening, eight of whom (30.8%) had extrathoracic TB (extrathoracic lymph nodes six; brain one; spine one); the remaining 18 (69.2%) had pulmonary TB. CXR correctly identified 10 of the 18 cases (55.6%) and missed eight (44.4%). Mean time (± SD) between false-negative CXR and positive diagnosis was 188 (± 115) days.
In total, TB in 16/17,487 (0.09%) refugees was missed by CXR. Eight of these were diagnosed with extrathoracic TB that could not have been detected by CXR. The remaining eight (8/17,487; 0.05%) were diagnosed with active pulmonary TB.
 CXR might be better used as an add-on to symptom-based TB screening, according to Dr. Julius Weinrich.
CXR might be better used as an add-on to symptom-based TB screening, according to Dr. Julius Weinrich.Speaking to AuntMinnieEurope.com, lead author Dr. Julius Weinrich, a radiologist in the Department of Diagnostic and Interventional Radiology and Nuclear Medicine at University Medical Center Hamburg-Eppendorf, pointed to the low yield of CXR screening for TB in the study, due to the low prevalence of TB in the sample population, and the high number needed to screen, strongly suggesting a need for improved, adapted screening algorithms.
Although he believes the low prevalence of active pulmonary TB in the population studied should be confirmed by further data from different refugee centers throughout the country, this particular study suggests that most refugees arrived healthy.
He added that only eight missed cases of pulmonary TB were seen in the study, and because the mean time between screening and diagnosis was long, it was likely these individuals were not diseased at the time of screening.
Moreover, epidemiological data suggest there is a rising number of extrathoracic TB in immigrants, which are not detectable by CXR screening. One-third of all definite TB cases in the study had extrathoracic TB.
Future strategy
It remained vital, therefore, to use thorough clinical examination with the aid of translators and questionnaires to detect individuals in whom there was a suspicion of TB. As a second step, measurements such as sputum sample or CXR should be used to increase screening accuracy in a predefined TB risk group, according to Weinrich. In patients with inconclusive CXR findings, CT is useful as an additional imaging method to detect pulmonary TB, he added.
"TB prevention should be based on medical attention in refugee camps and awareness amongst refugees about the symptoms of TB. Instead of generally screening each person with CXR, it might be better used as an add-on to symptom-based TB screening," Weinrich said.
He believes the study provides evidence that those who were identified with TB already had clinical symptoms, supporting the view that CXR screening should only be performed in cases where there is a suspicion of active pulmonary TB.
He admits there are challenges to changing screening strategy; not all centers have enough staff and equipment to deal with overwhelming numbers of refugees. In addition, clinical examinations and history-taking could be more time-consuming and difficult than generalized CXR screening due to a lack of translators. Moreover, this approach might not be feasible in the scenario of one million refugees arriving in the course of a year.
"Unfortunately, we did not obtain all personal data, such as the country of origin. Thus, we were not able stratify for risk groups. Future studies should evaluate if risk stratification before CXR might improve sensitivity," he concluded.