
Having more information about the biological sex and gender of patients enables radiologists to improve their care and communication and become patient-oriented physicians, according to new international research posted in the European Journal of Radiology (EJR).
How well do radiology hardware and software support trans patients, such as by providing a third option for patients to list their gender? The answer is important as radiology seeks to be an inclusive and supportive discipline, noted the authors of a study published on 16 April in the EJR.A team led by Dr. Simon Matoori from the University of Montreal wrote that having a third gender option available on radiology hardware and software allows radiologists to accurately document patient gender in the medical record and help with inclusivity.
"In general, we are trying to improve awareness on the complexity of questions around biological sex and gender in radiology," wrote Matoori and his co-authors, who included respected radiologists Dr. Rosemarie Forstner from the University of Salzburg, Austria, and Prof. Andreas Gutzeit from Lucerne, Switzerland.
Previous research suggests that people who identify as transgender make up between 0.3% and 0.6% of the U.S. population. The researchers wrote that trans individuals have higher rates of diseases related to anxiety, substance abuse, HIV infections, and cancer. There are also medical conditions that are unique to trans individuals, such as the effects of testosterone substitution in trans men causing ovary changes similar to polycystic ovary syndrome.
"With a prevalence of 0.3% of transgender patients, a large hospital with a reported number of 116,525 imaging sessions per year will have 350 imaging sessions associated with a transgender patient per year," the researchers noted.
Trans patients also face discrimination in healthcare, which has reportedly prevented many from seeking medical attention. The study authors wrote that communication errors due to missing information on patient biological sex can also hinder optimal care and inclusivity. However, radiologists can help with this.
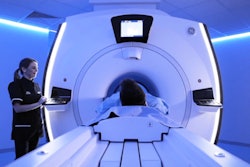
Matoori et al wanted to see if radiological technology is inclusive of gender diversity. They surveyed major hardware and software vendors of CT and MRI scanners, as well as providers of RIS and PACS software.
"From a radiological perspective, a more accurate record of each patient's sex/gender classification would be desirable," they wrote.
Six hardware and six software vendors responded to the survey. All but one of the 12 vendors reported having a third gender option in addition to male or female.
Software systems used terms defined by the Digital Imaging and Communication in Medicine (DICOM) standard, which allows for gender registration as "male," "female," or "other." For "other," RIS software can be coded to give additional information on gender status.
The authors wrote that they believe it's important for radiologists to have information about the biological sex and gender of patients for care and communication. This can help radiologists be patient-oriented physicians and understand the ins and outs of direct patient care.
"Trust being fundamental in positive patient experience, staff training on inclusive communication and transgender reality could facilitate the collection of gender-related information and potentially improve medical outcomes," they added.
The researchers also called for more studies regarding contrast agent dosing, radiation safety and protection, and image quality and interpretation. However, they also noted that gender assignment treatments are important medical information as well since trans patients may be at higher risk for certain diseases.
"Thus, noting a diverse or 'other' gender and additionally defining the biological sex could facilitate imaging interpretation when provided with the correct clinical context," they wrote.


![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=100&q=70&w=100)




![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)









