A study conducted in Africa found that breast ultrasound can be used successfully by trained nurses and clinicians to detect lesions in areas where radiologists are scarce. The research was published on 20 June in the Journal of the American College of Radiology.
A team led by Dr. Lydia Pace from Brigham and Women's Hospital in Boston found that nonradiologist clinicians at a hospital in rural Rwanda could evaluate lesions that proved to be cancer with high sensitivity and "acceptable" positive predictive value (PPV) and that "very few" lesions believed to be low risk were diagnosed as cancer.
"These data can be used to guide clinical protocols, including thresholds for biopsy of sonographically benign-appearing lesions in limited-resource settings," Pace et al wrote. "Where barriers to patient follow-up are high, lower thresholds for biopsy may be indicated, though these must be balanced with the costs and harms of unnecessary biopsies."
Previous research suggests that two out of three breast cancer deaths occur in middle- and low-income countries. In these countries, screening mammography is not used as often and cancers are often diagnosed at a later stage.
The study authors noted that breast ultrasound is considered to be safe and relatively inexpensive while being able to detect and characterize palpable lesions. They wrote that ultrasound can play a role in evaluating and triaging breast abnormalities, as well as determining whether biopsy is needed.
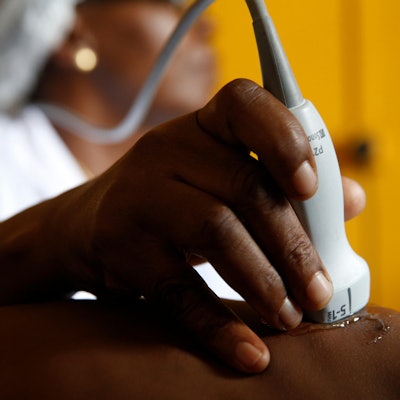
 Ultrasound is proving an increasingly valuable tool that can expand access at health facilities in low-income countries. Photo taken at Brazzaville Hospital, Republic of the Congo. Courtesy of GODONG / BSIP and Alamy Stock Photo.
Ultrasound is proving an increasingly valuable tool that can expand access at health facilities in low-income countries. Photo taken at Brazzaville Hospital, Republic of the Congo. Courtesy of GODONG / BSIP and Alamy Stock Photo.But radiologists are not widely available in rural areas in low-income countries, creating a barrier to access. Pace led a team that from 2015 to 2017 started a healthcare provider training program for early breast cancer detection in a rural part of Rwanda, the Burera District. The team's goal was to inform clinical protocols and build capacity in diagnostic breast ultrasound in Rwanda and other settings with limited resources.
The researchers trained nonradiologist doctors and nurses at the Butaro Cancer Center of Excellence, including seven weeks of intensive in-person training in January and February 2016, followed by e-mail remote supervision. Compared with trainer assessments, the sensitivity of trainee assessments for identifying a solid mass at medium or high suspicion of being cancerous was 95%, the authors wrote in a previous study at the center.
Pace and colleagues looked at data from 299 palpable breast findings from 199 patients, with 104 lesions initially biopsied. Out of the biopsied lesions, 38 were deemed to be malignant and three were deemed malignant on repeat biopsy.
A total of 34 patients were diagnosed with breast cancer and received initial recommendations for either biopsy or aspiration by trainees.
The team found that the positive predictive value of trainee biopsy recommendation was 34.8%, while their sensitivity for identifying malignant lesions was 92.7%. Of the 46 patients who did not receive biopsy and were told to return for clinical or imaging follow-up, 37% did not return.
The study authors wrote that none of the patients had subsequent diagnoses of cancer after being discharged or told to return for clinical or radiologic follow-up only. They added that all patients who were diagnosed with breast cancer received initial trainee recommendations for biopsy or aspiration.
Pace et al concluded that breast ultrasound is a "valuable" tool that is feasible and can expand access at health facilities in low-income countries.
"The World Health Organization's Global Breast Cancer Initiative is establishing recommendations for implementing breast cancer control, including rapid diagnosis, in resource-limited settings," they wrote. "Breast ultrasound performed by non-radiologists with adequate training and ongoing mentorship could play an important role in efficient evaluation of palpable masses."



















