Researchers from a top London facility have implemented a novel protocol to remove radiologist vetting of acute head CT exams in adults. This led to a marked and sustained reduction in the number of phone interruptions to the on-call radiologist, without increasing scanning numbers, they noted.
Are phone calls giving you a headache? That was the question asked by Dr. Sara ffrench-Constant and colleagues from the department of radiology at London's Imperial College Healthcare National Health Service (NHS) Trust. Their main goal was to reduce unnecessary interruptions during on-call radiology reporting.
"The U.K. has the second smallest radiology workforce in Europe, yet the number of CT scans being performed has more than doubled over the last five years," they stated in a poster presentation at the recent UK Imaging & Oncology Congress in Liverpool. "Rising workload is being compounded by increasing frequency of interruptions, the majority of which are phone calls. This reduces efficiency and can lead to reduced diagnostic accuracy."
Radiologists should be readily accessible, but unnecessary interruptions must be minimized for maximal clinical effectiveness, they explained.
Identifying the problem
The investigators conducted a prospective observational study across a large multisite hospital group. They recorded the quantity and reasons for phone calls by the on-call radiology registrars (junior doctors) over a three-week period before and a three-week period after implementation of a new protocol informed by their initial results. On-call shifts included evenings (5 p.m. to 9 p.m.), nights (9 p.m. to 9 a.m.), and weekends (9 a.m. to 9 p.m.).
The researchers aimed to identify common and potentially avoidable reasons for phone call interruptions to the on-call radiologist. They decided to conduct a reaudit following an intervention with the objective of reducing the frequency of phone call interruptions during radiology reporting.
At the Imperial, all acute CT and MRI requests require vetting by a radiologist prior to scan acquisition. Consequently, initial audit results demonstrated that calls to request the vetting of a study accounted for 230 (54.2%) of the 424 phone calls made to the on-call radiologist. Of these, 110 (22.3% of total) were requests for vetting of noncontrast CT head exams.
An unenhanced CT head exam is a low-dose study with high yield, meaning requests are rarely declined by the on-call radiologist. This means the current pathway of contacting the on-call radiologist to vet the scan is costly and futile in many cases, the authors explained. To improve efficiency, managers at Imperial introduced a protocol to remove radiologist vetting from the pathway, and all adult, unenhanced CT head requests fulfilling specific acute criteria went ahead.
Following protocol implementation, the number of phone calls about head CT exams fell by 81%, and there was a 21% reduction in the number of calls per shift to the on-call radiologist. Calls requesting vetting of head CT exams decreased from representing 26% of all calls to only 4%.
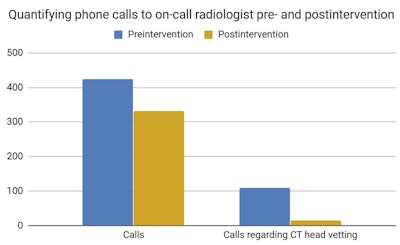 Source: ffrench-Constant et al.
Source: ffrench-Constant et al.Overall, the number of acute head CT exams performed out of hours remained largely unchanged, at 1.21 per hour after the intervention, compared with 1.33 exams per hour before the intervention. This supports the rationale behind the intervention, according to the group.