
A study using dual-energy x-ray absorptiometry scans to image obese patients suggests that increases in visceral body fat may be associated with an individual's quality of sleep, particularly duration, researchers from a top London facility have reported.
An international group led by Dr. Panagiotis Giannos of Imperial College London found that visceral fat mass was negatively associated with sleep duration in a group of 5,151 adults, with a plateau effect at eight hours of sleep per day. The finding sheds new light on potential links between obesity and sleep deprivation, the authors suggest.
"Our study adds further evidence to the notion that chronic sleep restriction may be a potential contributor for visceral fat mass adiposity," the group wrote. The study was published on 15 March online in Sleep Medicine.
Increasing rates of obesity and habitual declines in sleep duration are public health concerns worldwide. Emerging evidence suggests a link between weight gain and reduced sleep, yet few studies have investigated the potential association between sleep duration with regional body fat mass in U.S. adults, according to the researchers.
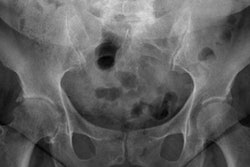
To address the knowledge gap, the researchers culled data from 5,151 participants from two U.S. Department of Health and Human Services surveys; the team estimated sleep duration via home interview questionnaires. All study participants underwent dual energy x-ray absorptiometry (DEXA) scans, which the researchers used to calculate regional body fat percentages.
The study cohort's food intake was within the recommended ranges and alcohol intake was low. Participants had high body mass indexes (BMI); the majority reported no trouble sleeping and were mainly free of any sleep disorders, the authors reported.
The investigators found a significant overall negative association between sleep duration and visceral fat mass: specifically, a difference of one hour less in daily sleep duration that corresponded to an increase of 12.1 grams in visceral fat mass. They also found that this association plateaued at eight hours of sleep per day and appeared stronger in men.
"Sleep duration is negatively associated with visceral fat mass accumulation during adulthood with possibly no benefits beyond eight hours of sleep per day," the study authors explained.
The results may be clinically significant, as visceral adiposity is associated with metabolic disorders such as insulin resistance and type 2 diabetes, which increase the risk of endothelial and cardiometabolic dysfunctions, according to the authors. Nonetheless, they did note that this is the first study to comprehensively explore the association between sleep duration and regional body fat mass.
"Mechanistic and prospective studies are required to confirm the effect of sleep duration on visceral adiposity and determine its causes," they concluded.








![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)








