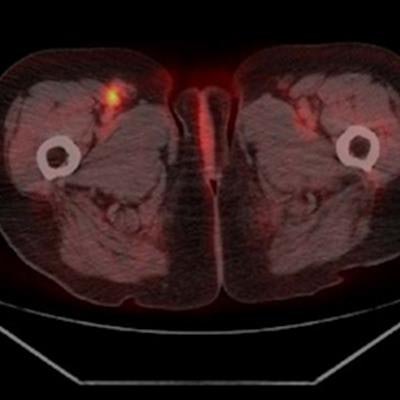
F-18 FDG-PET/CT imaging is a better choice than ultrasound for detecting both lymph node and abdominal metastases in patients with malignant melanoma, Swiss investigators have found.
Due to F-18 FDG-PET/CT's higher sensitivity and because it detected additional metastatic lesions throughout the body, the modality has an edge over ultrasound, which is typically used to identify metastases in this type of cancer, a team led by Dr. Philipp Weber wrote. "F-18 FDG PET/CT is preferable to ultrasound for detecting both lymph node and abdominal metastases."
Malignant melanoma has steadily increased in Switzerland. The incidence among men has grown by 83.3% since the late 1980s and among women by 63.5%, according to the researchers. Determining which imaging modality offers the highest sensitivity and specificity for primary staging and restaging is crucial, they noted.
In this study, Weber and colleagues included 308 patients who underwent one or more F-18 FDG-PET/CT scan and/or one or more ultrasound exams for primary staging or restaging of suspected or confirmed metastatic melanoma between September 1998 and August 2014 for primary staging or restaging of suspected or confirmed metastatic melanoma. The results were published on 21 October in Medicine.
Overall, F-18 FDG-PET/CT identified 824 cancer lesions and ultrasound identified 726. On a per-exam basis, an analysis revealed significant differences for the sensitivity of F-18 FDG PET/CT (80%) compared to whole ultrasound (63%) and peripheral lymph node ultrasound (61%). PET/CT's specificity was slightly lower compared with ultrasound, however, at 96% versus 98% for whole ultrasound and 99% for abdominal ultrasound, the researchers reported.
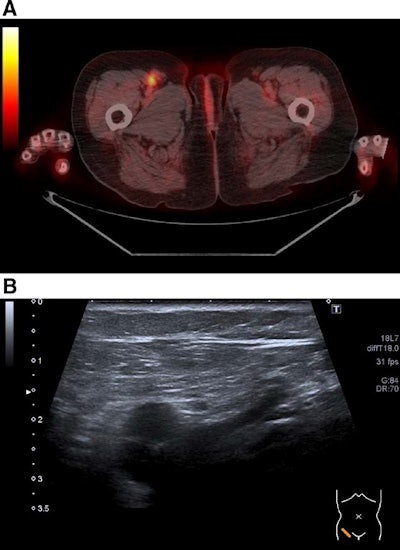 Lymph node metastasis inguinal right. (A) Detected as true positive by F-18 FDG-PET/CT. (B) Not evaluated as lymph node by ultrasound (false negative). Image courtesy of Medicine.
Lymph node metastasis inguinal right. (A) Detected as true positive by F-18 FDG-PET/CT. (B) Not evaluated as lymph node by ultrasound (false negative). Image courtesy of Medicine.Weber and colleagues noted that at their clinic in Basel, patients with malignant melanoma have undergone a combined examination with both modalities for several years. But in addition to being more accurate, using F-18 FDG-PET/CT alone may save costs, and they plan to use the study results to inform their practice, they wrote.
"Based on the available data from this study, the use of [abdomen ultrasound] cannot be justified, neither as a sole application, nor in combination with F-18 FDG-PET/CT," the group concluded.












![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)




