
Radiologists will lament the day if they lose ultrasound as a valuable diagnostic tool, and there will be no going back afterwards, warned world expert Prof. Paul Sidhu in London on 22 September.
 Prof. Paul Sidhu.
Prof. Paul Sidhu.Many radiologists don't want to perform ultrasound because it is "seen as a chore," Sidhu told attendees at the British Institute of Radiology (BIR) Annual Congress. But they would come to regret abandoning the field altogether to other trained practitioners who are enthusiastically gaining skills and developing their use of a highly effective tool, he added.
"If radiology abandons ultrasound, it will adversely affect the comprehensive framework of imaging methods available for patient care provided by the radiological community." said Sidhu, who is professor of imaging sciences at King's College London and consultant radiologist at King's College Hospital.
He said it was possible that in 10 to 20 years' time, radiologists won't be performing ultrasound. It would be a mistake for radiologists, who have a broad understanding of all the different imaging techniques and how they interact, to leave the field of ultrasound to others completely, noted Sidhu, who is a past president of the European Federation of Societies for Ultrasound in Medicine and Biology (EFSUMB) and the British Medical Ultrasound Society (BMUS), and currently editor-in-chief of Ultrasound in Medicine and Biology.
Evolving modality
Ultrasound capabilities were "ever-evolving," with many different techniques combining to achieve a patient diagnosis, so-called "multiparametric" ultrasound, he continued. Moreover, this was accomplished at lower cost and patient morbidity than any other imaging modality.
He said ultrasound's appeal would only grow, with the hand-held scanners changing practice and making it more popular as a bedside tool.
"This is how good ultrasound is, how patient-friendly it is, and why you shouldn't be losing it to everyone else," Sidhu told BIR delegates.
He described the benefits and growing capabilities of ultrasound, including contrast-enhanced techniques and "exciting" developments in hepatic care, for measuring the quantity of fat and stiffness in patients' livers.
He said practitioners outside of radiology were "embracing all aspects of new ultrasound technology because they don't have immediate access to MRI and CT." Because many of them were not medically trained, there was a danger they would become purely technicians -- without a full understanding of the diseases they were looking at.
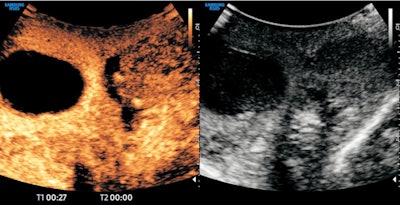 Contrast-enhanced ultrasound demonstrates testicular infarction in a case of spermatic cord torsion. Image courtesy of Prof. Paul Sidhu.
Contrast-enhanced ultrasound demonstrates testicular infarction in a case of spermatic cord torsion. Image courtesy of Prof. Paul Sidhu.In some countries, such as China and Russia, the trend was for ultrasound practitioners "only to do ultrasound, nothing else."
In the U.K., around 90% of ultrasound is performed by sonographers, whereas in European countries ultrasound is still predominantly physician-led, according to Sidhu.
The U.K. has a longstanding shortage of consultant radiologists and unlike many other European countries, only a small amount of diagnostic ultrasound is undertaken by clinicians. He said a hybrid model potentially offered the "best" way forward -- an ultrasound department run by radiologists but used by other practitioners of ultrasound and staffed by doctors and sonographers, as was happening in Germany, for example.
"The most important thing is to be with, and next to, a patient. Radiologists need to be fully aware of what they're doing -- there's no going back if there's a loss of ultrasound," noted Sidhu, who was awarded the Gold Medal of the Royal College of Radiologists in June 2022.









![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)





