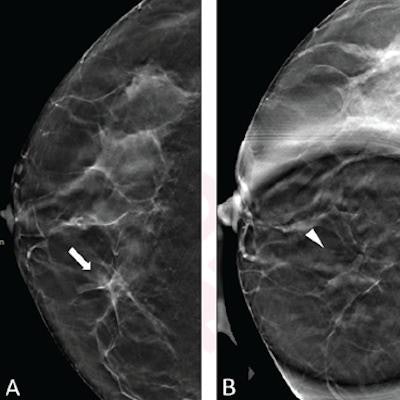
Digital breast tomosynthesis (DBT) combined with synthesized mammography can detect more invasive breast cancers than digital mammography alone, according to a German study of nearly 100,000 women.
A team led by Prof. Dr. Walter Heindel from the University of Münster found that the detection rate from the combined approach was about 48% higher compared with full-field digital mammography used in routine screening.
"The findings ... might help to close an important knowledge gap and to develop advanced strategies for an improved systematic early breast cancer detection in population-based settings," Heindel and colleagues wrote in an article published on 12 April in Lancet Oncology.
Digital mammography may be the standard when it comes to breast cancer screening, but DBT's popularity continues to grow among breast radiologists. The researchers believe DBT reduces the likelihood of overlapping breast tissues that can hide features indicating malignancy.
Previous research suggests that combining digital mammography with DBT can detect more cancers. However, this means patients are exposed to more radiation than usual. Synthesized 2D mammography could help with this issue since images are constructed from an already-acquired DBT exam, the study authors wrote.
The team wanted to test this out by creating the Tomosynthesis plus Synthesized Mammography Study (TOSYMA). A total of 99,689 women who were screened between July 2018 and December 2020 were included. The women were between the ages of 50 and 69 and were screened in 17 units in two federal states of Germany.
The women were randomly placed into one of two groups, one that used DBT plus synthesized mammography (49,762 women) and one that used digital mammography (49,796 women).
The combined approach detected 354 invasive breast cancers in its respective group, with a detection rate of 7.1 cases per 1,000 women screened. Conventional digital mammography, meanwhile, detected 240 invasive cancers in its respective group, with a detection rate of 4.8 cases per 1,000 women screened (p < 0.0001).
The researchers also found that the median glandular dose for radiation absorbed by the breast was 1.86 mGy for the group that got DBT plus synthesized mammography and 1.36 mGy for the group that received conventional digital mammography. The national diagnostic reference level in Germany is 2 mGy.
The team also reported that the median reading time for the DBT plus synthesized mammography group was twice as high as the digital mammography group, at 109 seconds compared with 54 seconds.
No statistically significant differences were found for recall rates for either group, and adverse events and device deficiencies were rare, with researchers reporting no serious adverse events.
While this study analyzed one screening round, researchers noted that the British "Prospects" study, which also has an enrollment of about 100,000 participants, will compare the cost-effectiveness and interval cancer rates of breast cancer screening with DBT plus digital mammography versus standard digital mammography.
With these results, the study authors touted DBT's potential long-term screening benefits with its higher detection rates over conventional mammography.
"An absolute increase in the detection rate of invasive breast cancer for early tumor stages in the screening phase of TOSYMA, presumably indicating diagnostic improvements, might be expected to reduce the incidence of advanced breast cancers in screened populations and thus, potentially exert positive effects on breast cancer mortality," they wrote.









![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)








