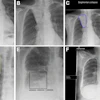
Leading European contrast media specialists have released new recommendations on how to manage and prevent the "underreported" problem of extravasation. The 11-page document released on 17 February covers pathophysiology, diagnosis, risk factors, treatments, and protocols.
"In an increasingly litigious healthcare environment, then the advice is to better document extravasation," Dr. Giles Roditi, consultant cardiovascular radiologist at NHS Greater Glasgow & Clyde, U.K., told AuntMinnieEurope.com. "After all, while the patient is at the CT or MRI scanner, it is quite easy to produce some images to inform as to whether the extravasate is only in a superficial compartment or in deeper tissues and this informs immediate management."
A protocol on how to deal with extravasation should exist in every radiology department, according to fellow author Prof. Olivier Clément, a radiologist at Hospital Pompidou APHP Paris. Risk of extravasation is dependent on scanning technique and patient risk factors, and diagnosis is mostly clinical and outcomes are mostly favourable. Referral to surgery should be based on clinical severity rather than extravasated volume, he said.
 Dr. Giles Roditi from Glasgow Royal Infirmary, U.K.
Dr. Giles Roditi from Glasgow Royal Infirmary, U.K.Contrast media extravasation involves leakage of intravenously administered contrast agents (either iodine or gadolinium-based) into the surrounding soft tissues, joint first authors Roditi and Dr. Nadir Khan and colleagues noted in European Radiology. It varies in severity and is one of the most frequent adverse events in radiology, but it is much less studied than other issues, such as contrast-associated acute kidney injury.
"Whilst contrast media extravasation does not usually lead to significant morbidity, the rare, serious complications of compartment syndrome, skin ulceration and tissue necrosis are important to recognise. Furthermore, even what may be clinically regarded as minor contrast media extravasation will be perceived as important by the patient and contribute to feelings of dissatisfaction at a stressful time since "something has gone wrong" with their care," the authors explained.
A recent study of over 142,000 patients undergoing CT scans showed contrast media extravasation incidence of 0.23%, while other researchers have found rates of 0.2%. Rates of serious contrast media extravasation seem much lower, but there is probably an element of underreporting, they added.
How do complications occur?
With contrast media extravasation, contrast escapes and infiltrates the interstitium during injection. This is mostly a clinical diagnosis and routine use of imaging is not indicated for its detection, according to the authors.
Technologists, radiographers, and healthcare support workers are usually the first responders, so Roditi and Khan recommend imaging departments follow a protocol that allows identification of at-risk patients, easy detection of extravasation, awareness of monitoring needs, and effective management of extravasation by a wide range of staff.
Outpatients with extravasation should be kept under observation in the department until a physician is satisfied that signs and symptoms are resolving such that intervention will not be needed and the patient allowed home. At the patient level, good documentation allows early recognition of deterioration, they emphasized.
The following are the three main ways of detecting contrast media extravasation:
- Direct patient observation. A technologist/radiographer located in the room or video monitoring observes and monitors scans for expected contrast arrival and completed scans for enhancement. Self-reporting by the patient is also an option.
- Pressure monitoring. Power injectors for contrast media administration have pressure monitoring systems with graphic displays and flow-profile previews that can automatically or semi-automatically stop the injection if increased resistance or faults within the system are encountered. One of the promoted benefits of this technology is extravasation prevention/minimization, but no published studies have specifically explored their impact to date.
- Extravasation detection accessories. Some vendors have developed sensors to detect extravasation amongst other capabilities.
The new advice is an update to pre-existing guidance rather than anything completely new, and in time it will be incorporated into the full, overarching ESUR contrast media guidelines, which are de facto seen as the profession’s guidance within Europe, noted Roditi, who is an honorary professor in the Institute of Cardiovascular and Medical Sciences at the University of Glasgow.
The guidelines apply across anatomic/clinical sub-specializations, including neuro and gynecologic radiology, and they must be viewed differently from those originating within special interest societies that only pertain to more focused issues (e.g. how often to follow up intracranial aneurysms), he added.
Work still to do
More work is needed here, particularly around the issue of patient perception of contrast media extravasation. "This is likely one of the commonest adverse events in radiology, but we did not have a good handle on exactly how common it is," Roditi added.
Clément thinks there is a need for a further systematic study to look at different risk factors, such as catheter type, type of contrast, temperature of injection, flow rate, volume injected, and injection site.