A misplaced MRI scan in the U.K. led to delays in treatment for an 8-year-old boy with brain cancer, according to a report published on 30 January in the Daily Mail.
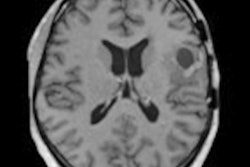
Rhonda Josephs' son Alexander began having seizures in September 2020, and an MRI scan at the Queen Elizabeth Hospital, Woolwich, showed a brain tumor, but a clerical error resulted in the scan being misplaced for three months.
The consultant pediatrician apologized to the mother of two, allegedly admitting to the clerical error that resulted in the scans not being flagged. "He said to me 'we're really sorry but for some reason, the MRI wasn't flagged in the system as him having a tumour, so it has just been sitting there,' " Rhonda told the Daily Mail.
To make matters worse, once the exam results were found and the tumor was identified in December, the COVID-19 pandemic further delayed treatment at a London hospital, the Daily Mail reported.
The patient's family sought to schedule surgery to remove the tumor, but in January 2021, staff at another hospital, King's College Hospital NHS Foundation Trust, London, told the family that cancer surgeries were being postponed because its intensive care unit was being used for COVID-19 patients.
However, after a February scan showed that the tumor had grown, Alexander had surgery in March at London's Royal Marsden Hospital. The tumor grew again, and he underwent a second surgery and began chemotherapy, according to the Daily Mail.
"Although the Royal Marsden is hopeful about Alexander's outcome, there is still only a 20% chance he will survive but the family are hopeful that their fundraising efforts could help them access more pioneering treatments in the future," the report concluded.








![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)






