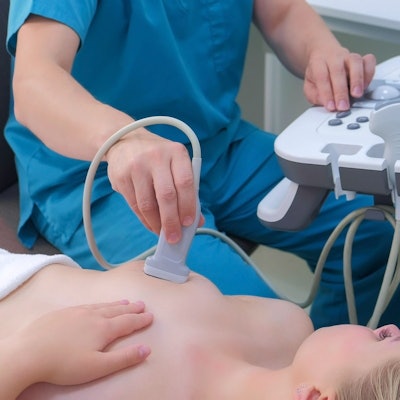
Diagnostic ultrasound outperformed other imaging methods when it came to assessing margins of cancers being excised during breast-conserving surgery, according to research published on 4 January in Academic Radiology.
A team led by Dr. Irina Manhoobi from Aarhus University Hospital in Denmark found that ultrasound had the highest pooled sensitivity, specificity, and area under the curve (AUC) for margin assessment compared to radiography, digital breast tomosynthesis (DBT), and micro-CT.
"Achieving adequate resection margins in breast conserving surgery is challenging and often demands more than one surgical procedure," Manhoobi and colleagues said.
Breast-conserving surgery and whole-breast irradiation are the standard treatments for early-stage breast cancer. One challenge facing surgeons, however, is that breast-conserving surgery involves removing the tumor with a sufficient margin while also preserving the physical appearance of the breast.
The researchers said that not much is known when it comes to the pooled diagnostic performance of imaging methods during surgery for assessment of tumor margins, as well as their impact on repeat surgery.
Manhoobi et al wanted to look at the sensitivity and specificity of conventional and emerging imaging methods for margin assessment during breast-conserving surgery. They also wanted to find out if these methods contribute to a reduced repeat surgery rate.
They looked at 22 research articles from the U.S., Europe, and Asia with 29 radiological imaging methods for meta-analysis, with the articles using either ultrasound, radiography, DBT, or micro-CT. The team found that ultrasound achieved the highest marks, despite only one study showing its use in assessing margins during surgery. The rest of the included studies showed that ultrasound was used for preoperatively marking the breast tumor.
| Performance of imaging modalities for breast‑conserving surgery | ||||
| Radiography | DBT | Micro-CT | Ultrasound | |
| Sensitivity | 52% | 67% | 68% | 72% |
| Specificity | 77% | 76% | 69% | 78% |
| AUC | 60% | 76% | 72% | 80% |
Despite ultrasound's high marks, the researchers said it is "not realistic" that ultrasound of specimens will be implemented in surgical workflows.
"It is too resource demanding for a breast radiologist to attend the operating theater and perform the intraoperative ultrasound of the specimen, and it takes time for a breast surgeon to achieve the same level of experience with ultrasound as a breast radiologist," the authors wrote.
Manhoobi et al said ultrasound's higher level of performance could be linked to operator dependability. Experienced breast radiologists performed ultrasound scans in half of the included studies. The team also wrote that ultrasound is limited by difficulties of detecting ductal carcinoma in situ (DCIS), and its use risks flattening the specimen when the transducer meets the specimen's surface, leading to false-positive findings.
"The radiological methods for margin assessment need further improvement to provide reliable guidance in the clinical workflow and to prevent repeat surgeries for early-stage breast cancer patients," the researchers said.







![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)






