PET imaging has revealed a connection in the brain between the opioid system and food craving triggered by external appetite stimuli, according to a recent study.
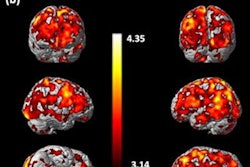
In a retrospective PET study, researchers from Finland analyzed imaging of central mu-opioid receptors (MORs) in 92 healthy subjects and cannabinoid CB1 receptors (CB1Rs) in 35 subjects. These receptors regulate energy balance in the brain via multiple neural pathways and promote food intake and reward.
Because obesity and eating disorders have been associated with alterations in the brain's opioid and endocannabinoid signaling, variations in MOR and CB1Rs system function could potentially underlie distinct eating behavior phenotypes, the researchers hypothesized.
They found that lower cerebral MOR availability was associated with increased external eating -- individuals with low MORs reported being more likely to eat in response to palatable food cues. CB1R availability was also associated with multiple eating behavior traits.
Although MORs and CB1Rs overlap anatomically in brain regions regulating food reward, they have distinct roles in mediating individual feeding patterns, the authors stated. The MOR system might provide a pharmacological target for reducing excessive cue-reactive eating behavior, the researchers concluded.
Low cerebral MOR availability is associated with increased externally triggered eating behavior, and the modern obesogenic environment may promote food consumption via engaging the opioidergic link of the reward circuit whose tone is linked with cue-reactive eating, they wrote.
"Our study suggests that for individuals with aberrant external eating, MOR system might provide a feasible pharmacological target to combat weight gain," the authors concluded. "Central CB1Rs are in turn associated with multiple eating behavioral traits measured with DEBQ, consistent with endocannabinoid system’s role as a major homeostatic regulatory system at the intersection of feeding, emotion and behavior."
The study was published on 27 August in Translational Psychiatry.









![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)






