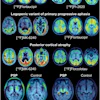
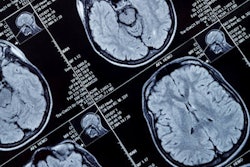
A brain study of long COVID conducted at a leading U.K. facility has highlighted gray-matter changes linked to inflammation in anosmia patients and microstructure properties possibly linked to iron homeostasis in patients recovering from COVID-19.
The research underlines the benefits of using advanced quantitative MRI to study the brains of patients recovering from the disease.
"COVID-19 has now been associated with neurological symptoms, but the pathogenesis of such symptoms is unknown. Advanced quantitative MRI can provide information on alterations of brain tissue properties beyond clinically identifiable lesions," noted Prof. Claudia Wheeler-Kingshott, professor of MR physics at the University College of London (UCL) Queen Square Institute of Neurology, and colleagues from Italy, the Netherlands, and Spain.
The group developed a novel comprehensive scanning protocol and highly automated analysis pipeline to compare brain structure and function in people who were exposed to SARS-COV-2 infection against individuals who were not.
 Researchers from the UCL Queen Square Institute of Neurology led the pan-European study of long COVID. Courtesy of Lankowsky / Alamy Stock Photo.
Researchers from the UCL Queen Square Institute of Neurology led the pan-European study of long COVID. Courtesy of Lankowsky / Alamy Stock Photo.Central nervous system (CNS) diseases, particularly vascular disorders and altered mental status, have been reported in symptomatic hospitalized patients. Plasma biomarkers of CNS injury are elevated in patients with moderate-to-severe COVID-19. Postmortem data have confirmed the presence of the SARS-COV-2 ribonucleic acid and protein in distinct regions of the brain.
"It is increasingly alarming that even people who experienced relatively mild COVID-19 report persistent symptoms, including fatigue, brain fog, anosmia, and autonomic dysfunction such as orthostatic hypotension. These persistent symptoms in otherwise healthy subjects are associated with what has now been defined as long-COVID syndrome," said Wheeler-Kingshott, who specializes in neuroinflammation and is head of quantitative MRI development on the 3-tesla scanner for multiple sclerosis research.
Also involved in the study were researchers from the Open University of Catalonia and Vall d'Hebron Institute of Oncology, both in Barcelona, Spain; the University of Pavia, Italy; and the VU Medical Centre in Amsterdam.
The need for evidence
The evolving landscape of COVID-19 neurological manifestations requires detailed population-level studies to understand the extent of direct and indirect effects of SARS-CoV-2 on the brain. Current studies are assessing possible consequences of associations between dementia genetic risk factors (apolipoprotein E gene) and COVID-19, the authors explained in a poster presented at the recent International Society for Magnetic Resonance in Medicine annual meeting.
Initially they recruited 40 people, of whom seven were not infected with SARS-COV-2 and were considered control subjects (two women, mean age 41 years, range 35-47). The remaining 33 subjects had polymerase chain reaction (PCR)-confirmed COVID-19 but had not been hospitalized or had positive IgM/IgG antibodies to SARS-COV-2 (30 female; mean age 42; range, 24-65) and were assigned to the COVID-19 group.
In an update received by AuntMinnieEurope.com on 30 May 2021, Wheeler-Kingshott noted that the UCL group has now completed the full study, which comprised 18 control subjects and 46 subjects who were infected with SARS-COV-2 several weeks prior to scanning.
"Nobody was hospitalised," she said. "Once correcting for age and gender, the white matter changes disappeared, but we detected grey matter changes linked to inflammation (in anosmia subjects) and microstructure properties possibly linked to iron homeostasis in the COVID group overall."
The study logistics
A Philips Ingenia CX 3T scanner with a 32-channel head coil was used. The MRI protocol combines cutting-edge methods for speed (simultaneous multislice echo planar imaging [EPI], compressed sensing, and image denoising) with advanced biophysical modeling of MR tissue properties, according to the researchers.
The acquisition protocol was developed in such a way that all EPI-based acquisitions have identical EPI readout. The protocol included clinical 3D fluid-attenuated inversion recovery (FLAIR) sequence for detecting brain abnormalities, 3D T1-weighted acquisition for brain volume measurements, quantitative proton density for macromolecular total volume calculations sensitive to the solid fraction, quantitative T2* for susceptibility-weighted imaging and quantitative susceptibility mapping for microbleeds and tissue composition, multi-shell diffusion-weighted imaging for microstructure assessment, resting-state functional MRI for brain functional connectivity, quantitative magnetization transfer and bound pool fraction for myelin integrity, MR spectroscopy from a voxel positioned in the brainstem for metabolic profiling, and arterial spin labeling for blood perfusion. The total scan time was one hour.
"For image analysis, data were automatically transferred from the scanner to a local XNAT server. 3D FLAIR images were assessed for hyperintensities by an experienced neuroradiologist," noted Wheeler-Kingshott and colleagues. "3D T1-weighted scans were first processed with the NicMSLesion software to detect abnormalities."
From the FLAIR radiological assessment, two subjects presented with incidental findings. Other white-matter hyperintensities were consistent with small vessel ischemia, each considered within the normal range (Fazekas scores < 3). Comparison of white matter, cortical grey matter, and deep grey-matter volumes between the control and COVID groups showed a smaller white-matter volume in COVID subjects (p < 0.001). Similarly, there was lower normal-appearing white matter (NAWM) fractional anisotropy (FA) (p < 0.01) and lower brainstem total choline (tCh) (p < 0.02) in COVID patients. No other statistical comparison was performed.
Sample size calculations (confidence interval, 95%; 80% power; equal group size) from these data support groups of 13 subjects each detected differences in NAWM FA in those with COVID. Power calculations indicated groups of 30 subjects, considering white-matter volume changes.
"Our fast multi-contrast protocol allowed us to acquire a uniquely rich dataset. Together with the decreased tCh in the brainstem, these results potentially indicate tissue damage in subjects who suffered from mild forms of COVID-19," the authors stated.
The UCL team is now preparing a full paper focusing on the grey-matter changes linked to inflammation in anosmia patients and microstructure properties possibly linked to iron homeostasis in the COVID-19 group overall.