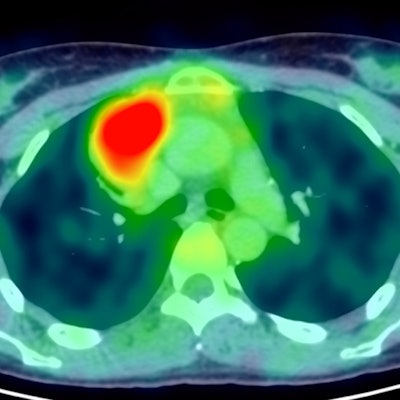
FDG-PET can help determine which younger patients with newly diagnosed early-stage unfavorable Hodgkin's lymphoma don't need treatment with radiation therapy, German researchers have reported at the virtual European Hematology Association (EHA) congress, held between 11 and 21 June.
In the treatment of early-stage Hodgkin's lymphoma in patients who have risk factors indicating an unfavorable prognosis, physicians have used four cycles of chemotherapy and radiotherapy. However, using radiotherapy in younger patients (median age of around 30 at disease onset) raises concerns about adverse events such as cardiovascular disease and secondary malignancies.
Results from the HD17 trial were unveiled at the EHR congress, and they demonstrated that omission of radiotherapy in the treatment of certain early-stage Hodgkin's lymphoma patients does not result in a loss of tumor control in patients responding well to a standard chemotherapy regimen. The researchers also found that most patients respond well to chemotherapy and benefit from this strategy.
A research team led by Dr. Peter Borchmann from University Hospital of Cologne sought to determine if radiotherapy could be omitted for patients that respond well to chemotherapy. They used FDG-PET to make that determination in 1,100 patients who were prospectively enrolled in the randomized trial.
At five years follow-up, only two out of 1,100 patients died from Hodgkin's lymphoma and only one died from treatment-related adverse events. The mortality of patients with early-stage unfavorable Hodgkin's lymphoma in the HD17 study did not differ from the normal German population, according to the researchers.







![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)






