
Logistical problems and personal beliefs play a key role in skipping breast cancer screening. That is the key finding of Italian researchers, who investigated why more than 30% of women miss their appointments in the northeastern region of Friuli Venezia Giulia.
The team aimed to uncover reasons behind the nonattendance of public screening via a qualitative telephone survey. In the region, 300,000 women are targeted per round for cervical screening, more than 150,000 women for breast cancer screening, and more than 300,000 men and women for colorectal cancer screening.
Friuli Venezia Giulia is the second best performing region of Italy for mammography screening, the third for colon cancer screening, and the first for cervical cancer screening in Italy, according to national figures. Nevertheless, participation levels can still be improved, the authors wrote in an article posted online in the journal Public Health on 17 January.
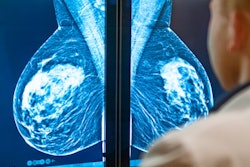
 Participation in screening could be improved, says Dr. Francesca Valent, PhD.
Participation in screening could be improved, says Dr. Francesca Valent, PhD.The survey helped the team understand that a gender gap exists in access to these programs, according to lead author Dr. Francesca Valent, PhD, director of the hygiene and clinical epidemiology unit of the University Hospital of Udine.
"Reported causes of nonattendance among women are fragility of position at work, being in charge of children and/or people with a disability or elderly relatives, and house duties," she told AuntMinnieEurope.com. "Regional public health authorities need to address this matter."
The study also revealed that people who take up screening outside the regional public health system are keen to continue privately, Valent noted. To counter this, the region has now planned a project specifically to support initial participation in the three public screening programs.
The researchers called a random selection of 4,456 individuals from the 2017 program -- 1,475 women from the mammography screening program, 1,483 women from the cervical Pap smear screening program, and 1,498 men and women from the fecal occult blood test screening program -- who, after invitation by letter to the screening, had failed to attend.
Answers from the single-question survey were transcribed with no personal identifiers, and these answers were then classified into exclusive macrocategories and subcategories. The main reasons provided for nonattendance are shown in the table below.
| Reasons provided for nonattendance as a percentage of responses for nonparticipation | |||
| Category of motivations reported for nonparticipation | Breast cancer screening (%) | Cervical cancer screening (%) | Colorectal cancer screening (%) |
| Personal factors -- beliefs | 18.4 | 11.7 | 26.3 |
| Personal factors -- practical issues | 34.4 | 45.7 | 54.6 |
| Physician-related factors | 0.1 | 0.0 | 0.0 |
| Exam-related factors | 7.6 | 1.6 | 1.1 |
| Screening program-related factors | 9.2 | 21.4 | 11.7 |
| No particular reason | 30.2 | 19.3 | 6.3 |
Clear results
Practical issues such as a language barrier, death in the family, sickness on the day of screening, disability, lack of time due to work, or looking after family members, including children, were the most common type of barrier reported in all three screening programs. This was followed by personal beliefs such as fatalism, fear of cancer, fear of examination, shame, mistrust of doctors, and a belief that screening is harmful, according to the authors.
Program-related issues such as accessibility, time taken to get to the screening center, transport problems, comfort of the environment, difficulties in contacting the center to reschedule, or no delivery of the invitation letter were more common in cervical cancer screening than in the others.
Just over 30% of those surveyed for nonattendance of public breast cancer screening did not provide a reason. Respectively, just over 19% and just over 6% of those failing to attend cervical and colon cancer screening did not provide a specific reason.
Almost half of the women not participating in the public breast cancer screening and 40% of those not adhering to the public cervical cancer screening had mammography or a Pap test privately.
The proportion of persons participating in private screening was high among those providing certain reasons for not attending the regional program. In the case of breast cancer screening, 100% of women who did not attend the public program because ultrasound was not offered in addition to mammography attended private screening.
Overall, 46% of respondents underwent private screening for breast cancer, 39% underwent private cervical cancer screening, and 12% had private colorectal cancer screening.
Scope for improvement
There are lessons to be learned for public screening organizers in terms of reaching target populations, according to Valent.
Public screening in this region has very high quality standards that may not be replicated by private clinics, she noted. These programs also manage individuals from initial screening tests through to treatment and follow-up, while this type of complete care is not offered in the private sector.
"The region must find a way to communicate that not only do the public programs ensure quality but also the advantages of a well-organized path in case a patient has a positive first-level test," she said.
Furthermore, she urged practitioners to engage in a discussion of personal beliefs, as well as to be prepared for questions about screening recommendations and the balance of benefits and harms. In addition, surveys of nonparticipants in other geographic areas could be helpful to local policymakers as they work to overcome practical barriers, Valent concluded.








![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)






