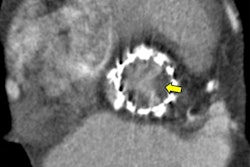
Intracoronary imaging -- such as intravascular ultrasound and optical coherence tomography -- can yield more precise diagnoses of heart attacks and be used to individualize patient treatment, according to an expert consensus paper published on 21 May in the European Heart Journal and presented this week at the EuroPCR meeting in Paris.
The paper, which was authored by a panel organized by the European Association of Percutaneous Cardiovascular Interventions (EAPCI), specifically promotes the use of intracoronary imaging in acute coronary syndromes -- including heart attack -- and when diagnostic information from coronary angiography is unclear. It includes criteria for assessment of the arteries, image interpretation, treatment decisions, and guidance of percutaneous coronary intervention (PCI).
The researchers, led by senior author Dr. Giulio Guagliumi of the Ospedale Papa Giovanni XXIII in Bergamo, Italy, noted that intracoronary imaging has identified plaque erosion and eruptive calcified nodules as other causes of acute coronary syndromes that may benefit from different treatment. Unlike angiography, intracoronary imaging can also clearly show thrombus, according to the researchers.
What's more, angiography is often ambiguous during heart attacks that lack an identifiable culprit lesion or have multiple culprit lesions. Intracoronary imaging, however, provides clarity both before and during PCI, according to the researchers.
"[Intracoronary] imaging is more accurate, helps guide decisions and facilitates tailored therapy, especially in younger heart attack patients who more frequently have plaque erosion or nonatherosclerotic coronary artery disease," Guagliumi said in a statement from the European Society of Cardiology.
Imaging is also particularly useful in complex patient and lesion scenarios, an important benefit as patients referred for PCI increasingly have comorbidities and complex coronary artery disease, according to Guagliumi.
"The role of intravascular imaging to diagnose acute coronary syndromes, select treatment, and guide PCI will continue to grow," said Guagliumi in a statement. "With it we expect to achieve superior long-term outcomes."
Although imaging companies have focused mainly on improving image quality, Guagliumi said that they should devote more attention to making imaging systems more user-friendly, such as incorporating automated analysis and classification.
"There is more to gain clinically through developments in these areas," he said.










![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)




