
The recent development of MRI scanners integrated with linear accelerators (linacs) represents a milestone in radiation treatment of abdominal tumors. MRI can produce diagnostic-quality images during radiation delivery, enabling visualization of tumors when surrounded by soft tissue. To exploit this improved in-room image quality and improve the accuracy when delivering increased doses and/or reducing margins, new MRI-based strategies for radiotherapy of moving targets are needed.
Integrated MR-linac systems are currently being evaluated as preclinical prototypes. An MR-linac comprising a 7 MV accelerator from Elekta rotating on a ring gantry around a modified 1.5-tesla MRI scanner from Philips Healthcare was initially developed and installed at UMC Utrecht. In 2012, the MR-linac Consortium was established -- whose members include Elekta, Philips, and seven academic hospitals in the Netherlands, U.K., Canada, and the U.S.
The Netherlands Cancer Institute (NKI) in Amsterdam is the third site in the world to install the integrated MR-linac. Researchers in its Department of Radiation Oncology have developed and validated an MRI-based midventilation (midV) approach for radiotherapy of the liver. MidV, defined as the anatomy of a patient closest to the time-weighted mean position of the tumor, offers two treatment advantages. It provides a motion-artifact-free representation of the anatomy, and minimizes systematic errors compared with any other breathing phase. This results in a significantly smaller planning target volume (PTV) compared with the internal target volume (ITV) method, for example (Radiotherapy and Oncology, November 2016, Vol. 121:2, pp. 276-280).
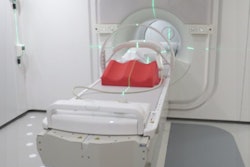
 Installation of the integrated MR-linac at the Netherlands Cancer Institute in Amsterdam.
Installation of the integrated MR-linac at the Netherlands Cancer Institute in Amsterdam.The method developed by the NKI team is an MRI-based midventilation approach for treatment planning and image guidance. The researchers obtained a high-quality MR image in midV and quantified respiratory-induced motion in 3D from additionally acquired time-resolved 2D MRI scans. To compensate for the fact the velocity of the liver is high in midventilation and images are most susceptible to motion artifacts, the researchers interleaved two navigator-triggered imaging sequences. They included a fast but low-resolution image in midV to minimize motion artifacts and facilitate an accurate midV position, and a high-resolution image acquired in exhale to exploit the prolonged time spent in this position. The exhale image was mapped to the midV anatomy using deformable registration to generate a high-quality image in midV. Sagittal and coronal cine-MRI scans were acquired. From these scans, respiratory motion was quantified in three directions for inclusion in the safety margins.
Tessa van de Lindt, a doctoral student in the group of Jan-Jakob Sonke, and colleagues, first conducted experiments using an MR-compatible motion phantom. They used six waveforms, acquiring an interleaved midV/exhale scan and two orthogonal cine-scans in the tumor compartment. These were used to vary different aspects of the respiratory pattern, specifically amplitude, period, and shape.
 Tessa van de Lindt is a doctoral student in the group of Jan-Jakob Sonke at the NKI's Department of Radiation Oncology.
Tessa van de Lindt is a doctoral student in the group of Jan-Jakob Sonke at the NKI's Department of Radiation Oncology.The researchers compared the midV position of the tumor compartment in the triggered scan with the mean position in the cine-MRI to determine the accuracy of the triggered midV position. The cine-quantified motion amplitude was compared with the real phantom motion.
Images were also acquired from 10 healthy volunteers and one patient with liver metastasis for validation. The total examination time took 15 to 22 minutes, with the acquisition of the interleaved midV/exhale scans taking three to five minutes. The total scan duration depended upon on each individual's respiratory pattern. The researchers validated deformable registration accuracy using the SIFT algorithm.
The authors reported that the accuracy of the midV-position was 0.5 ± 0.5 mm for phantom motion and 0.9 ± 1.2 mm for the volunteers; mean residuals after deformable registration were 0.2 ± 1.8 mm. The accuracy and reproducibility of the method used for all studies are within proven inter- and intrafraction liver position variability. Image sharpness was quantified by evaluation of intensity profiles of veins in the liver, and image quality was assessed by visual inspection of small structures in the liver. The deformed exhale-to-midV images had better in-plane image quality, in terms of the visibility and sharpness of small structures in the liver, compared with the midV images.
Van de Lindt explained that the phantom study demonstrated the algorithm was implemented correctly and was robust to variations in waveforms, while the volunteer study demonstrated the method is accurate in humans who have more irregular motion than the phantom. Imaging a patient with liver metastasis demonstrated adequate tumor visualization.
Clinical applications
According to the authors, the MRI-based midV method could be incorporated into a conventional liver radiotherapy workflow for better registration with the midV planning CT, as well as a midV-based online MR-linac workflow. Van de Lindt told medicalphysicsweb that at NKI, a midV CT is currently being used for treatment planning, and additional MRI scans are acquired in exhale to provide optimal image quality.
However, the exhale MRI scans are often difficult to register with the midV planning CT. Van de Lindt believes use of the midV method would improve the MRI-to-CT image registration accuracy. She noted the method could be validated on more patients and that the research software needs to be released for clinical use, anticipated in 2017.
Another clinical application Van de Lindt foresees is the use of midV triggering on the MR-linac for accurate tumor targeting, not only in liver cancer patients but also other disease sites. "Such clinical application requires the clinical release of the MR-linac system and the integration of the midventilation triggering with this system," she said. "We expect this integration to be completed in 2018. However, implementation on other hospital's radiation oncology departments depends on the plans of commercial vendors."
© IOP Publishing Limited. Republished with permission from medicalphysicsweb, a community website covering fundamental research and emerging technologies in medical imaging and radiation therapy.

















![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)