A new initiative that leverages radiation dose-monitoring software can achieve crucial results, including optimization of CT protocols and sharp decreases in mean effective dose to patients, according to recent research from Basel University Hospital in Switzerland.
Making use of data from radiation dose-monitoring software to guide its dose-reduction efforts, the institution was able to cut mean effective dose from CT scans by 32% over a three-year period, even in the midst of a 20% increase in scan volume.
"A comprehensive program with important tools such as radiation dose-tracking software can provide a substantial support for obtaining the big picture of actual practice at an institution, and is instrumental in depicting the room for optimization and standardization of protocols with improved statistical certainty since they are based on larger values and numbers," said lead author Dr. Anushri Parakh. "[This enables] increased patient safety by performing dose tracking, dose benchmarking, application of dose alerts, and helping in decisions such as investing in dose-efficient technology."
She shared the findings during a scientific session at the recent ECR 2016 in Vienna.
More CT scans
The number of CT scans performed continues to rise each year, caused in part by the increase in installed base of CT scanners, Parakh said.
"In Switzerland alone, there has been an increase by 54% in the number of CT scanners installed between 2004 and 2013," she said.
Another important contributing factor to the growth of CT has been the evolution in CT technology.
"This had led to faster temporal resolution and improved spatial resolution, furthering its foray into functional imaging [and] leading to an improved clinical outcome and also having important medicolegal implications," she said.
Not surprisingly, these factors have led to CT generating the highest radiation burden for patients compared with other imaging modalities that generate ionizing radiation, she said. Up to now, the role of the medical community has been to optimize radiation dose from CT scans by using referral guidelines, proper patient positioning, and contrast optimization by technologists, protocol optimization, and various innovations by vendors.
"All of this has been done basically to personalize scans to avoid a one-size and one-scan-fits-all approach," Parakh said. "What has been widely neglected up to now is the quantification of doses."
Tracking dose
With that in mind, the researchers set out to utilize dose-monitoring software to track and analyze the radiation dose of different CT protocols performed between January 2012 and December 2014 at their institution. Over the study period, a multidisciplinary team consisting of a radiologist, technologist, medical physicist, and IT specialist teamed up on a CT dose optimization program. This initiative involved systematic optimization of protocols, identification of dose outliers, training of technologists, and investment in dose-efficient scanners, Parakh said.
In 2012 and 2013, testing encompassed four CT scanners from Siemens Healthcare: an Emotion 16-slice scanner, a Sensation 64-slice scanner, a Definition AS+ 128-slice scanner, and a Definition Flash 128-slice CT scanner. Both Definition models were equipped with the vendor's sonogram-affirmed iterative reconstruction (SAFIRE) iterative reconstruction software.
In 2014, the institution replaced one of the systems to add another scanner capable of performing iterative reconstruction, she said. CT dose metrics -- CT dose index volume (CTDIvol), size-specific dose estimates (SSDE), dose length product (DLP), and effective dose -- were tracked using the Radimetrics radiation tracking software (Bayer HealthCare).
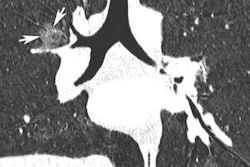
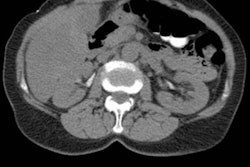
The team focused on five indication-based single-phase CT protocols: head for cerebral hemorrhage; thorax for pulmonary nodules/pneumonia; abdomen-pelvis for acute abdomen; low-dose pulmonary angiogram for pulmonary embolism; and low-dose renal colic for urolithiasis.
| CT radiation dose reduction by year | ||
| Total number of CT scans | Mean effective dose | |
| 2012 | 18,794 | 7.6 mSv |
| 2013 | 21,210 | 5.8 mSv |
| 2014 | 22,558 | 5.1 mSv |
While CT volume grew 20% over the three-year period, mean effective radiation dose decreased by 32%, with different protocols seeing varying levels of reduction.
Change in mean effective dose by protocol from 2012-2014
- Routine CT thorax: -64%
- Low-dose CT pulmonary angiogram: -48%
- Low-dose CT for urolithiasis: -48%
- Routine CT head: -34%
- Routine CT abdomen-pelvis: -31%
Alerts for outliers
The institution also sought to track dose outliers by setting up alerts in the dose monitoring software. Due to the lack of guidelines, the team arbitrarily set up thresholds that would trigger alerts. For example, the threshold for a dose alert on abdominal CT scans was a CTDIvol of 20 mGy, 5 mGy above the national diagnostic reference level. Over the study period, there was a significant reduction in the number of exams that were above the dose threshold, Parakh said.
The group also performed benchmarking of their scanners -- two of which had iterative reconstruction software -- and found a four-fold difference in doses among the systems; the highest dose was a dose-length product (DLP) of 8 mSV, while the lowest was 2 mSv.
"With this information, we tried to have the younger, radiosensitive patients being scanned on the iterative-reconstructed machines," she said. "We also invested in a new scanner in 2014, such that there was a more harmonious distribution of our doses."
Now, the three scanners vary in dose, from a median DLP of 1.3 mSv to 1.7 mSv, she said.
In addition to a decrease in median DLP, there was also a narrowing in the dose ranges.
| Resolution in CT thorax dose | |||
| Median dose-length product | Dose-length product: 25th percentile | Dose-length product: 75th percentile | |
| 2012 | 245 mGy/cm | 132 mGy/cm | 401 mGy/cm |
| 2013 | 133 mGy/cm | 90 mGy/cm | 218 mGy/cm |
| 2014 | 81 mGy/cm | 65 mGy/cm | 103 mGy/cm |
"What this means is that there was a reduction in variation in doses, or rather simply put, a standardization of practice was achieved in our institution," Parakh said.