
In French telemedicine, two key domains of application concern imaging: telestroke and emergency. Telemedicine is developing fast due to skill shortages in certain areas, and this has resulted in constant growth of the sector. In this article, we intend to address the topical issues in neuroradiology, notably telestroke and thrombectomy.
Telemedicine and neuroradiology also involve expertise and interpretation of scheduled exams, with requests for centralized second readings in the screening of progressive multifocal leucoencephalopathy during the follow-up of patients on natalizumab, and in the diagnosis and follow-up of cerebral tumors.
 Dr. Nadya Pyatigorskaya is from the Pitié Salpêtrière University Hospital in Paris.
Dr. Nadya Pyatigorskaya is from the Pitié Salpêtrière University Hospital in Paris.Teleradiology is a great asset in the management of patients, whether it is practiced intrainstitutionally or as part of a regional or national solution. The practice of teleradiology in France is governed by the Charter of Teleradiology, which was created by the Professional Council of Radiology (Conseil Professionnel de Radiologie, G4) together with the French National Medical Council (Conseil National de l'Ordre des Médecins, CNOM). This charter reminds practitioners of the duties and ethical principles of physical and moral parties involved in the teleradiology network, and specify the rules of medical ethics and professional good practice applicable to this activity.
The place of teleradiology in neuroimaging has become particularly important with the development of management networks for acute stroke and the increase in indications for thrombectomy. Indeed, recent studies underlining the efficacy of thrombectomy in the management of acute stroke point to the necessity of a thorough reorganization of management networks for acute vascular patients, within which neuroimaging should be central to both diagnosis and therapy. Let us not forget that speedy management of stroke is a top priority in public health and is part of two top national priorities in the area of telemedicine and emergency care.
This recourse to teleimaging is also based on European experiments that have shown the efficacy of teleimaging in the management of acute stroke. But what is the goal? Allowing a better selection of patients presenting with indications for thrombectomy and requiring transfer to a specialist interventional neuroradiology center.
This selection is based on clinical and radiological criteria. The patient managed in an emergency department with an imaging facility can benefit immediately from an assessment without any time wasted. In a neurovascular unit without an on-call interventional radiology team, teleradiology can be used for image transfer and thus for selecting patients for potential thrombectomy.
Which examination to use?
From an imaging point of view, MRI remains the key exam for positive diagnosis of ischemia. Time elapsed since stroke onset is estimated due to combined diffusion/fluid-attenuated inversion recovery (FLAIR) analysis, exclusion of intracranial bleeding, and localization of arterial occlusion, an important element in the decision for an eventual thrombectomy. The time-optimized protocol includes diffusion sequences T2*, time of flight, and FLAIR.
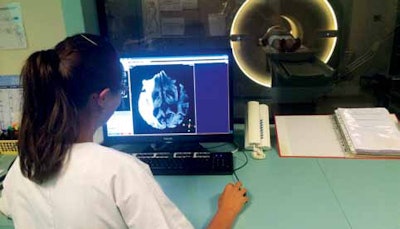 MRI acquisition in a university hospital with a stroke unit, sending data to a teleimaging center for expert discussion of thrombectomy. Image courtesy of JFR.
MRI acquisition in a university hospital with a stroke unit, sending data to a teleimaging center for expert discussion of thrombectomy. Image courtesy of JFR.Imaging can also be undertaken with CT, if MRI is not available, with a study of the intracranial parenchyma (cerebral CT without injection), combined with a vascular study through an angio CT of the polygon of Willis (to look for level of arterial occlusion).
Thanks to teleradiology, if the network and the technical protocols that are put into place work correctly, the exam can be interpreted quickly by a referring neuroradiologist capable of selecting patients requiring urgent transfer for thrombectomy. Other specialists such as the vascular neurologist can equally intervene through teleconsultation, thus forming with the teleradiologist a multidisciplinary telemedicine network.
This interpretation can be made in the frame of telediagnostics through a protocoled study and interpreted distantly if no radiologist is present at the exam site or in the frame of telexpertise if the radiologist present needs a second opinion. The same principle can be applied for the other actors in the clinical management of the patient. It is clear that, to be effective, teleradiology in the management of acute stroke must be optimal, in order for precious time to be saved when making therapeutic decisions. "Time is brain" prevails and therein lies the challenge!
Optimizing patient care
How can we optimize care when adding in a stage without costing the patient time? This requires organizing in advance a specific network defined by a flowchart, linking the different requiring centers to specialist interventional neuroradiology centers working with teleinterpretation and teleexpertise. It is also fundamental that close and constant contact is maintained between the imaging centers where the patient is managed and those where the imaging is interpreted.
Finding an effective image transfer technique between these centers, and a prior optimization of protocols by the radiologist and technician, is also important. Regular communication between the medical radiology team and the technicians undertaking the exams is fundamental for establishing protocols and for subsequent follow-up.
On the technical front, it is necessary to have a secure network allowing rapid and secure transmission without loss of data (benefit of bandwidth outside hospitals and centers with a neurovascular unit), allowing an optimizing of time, and of the quality of images transferred. Systematic quality control is important and is a part of the teleradiology charter.
Beyond all technical considerations that facilitate smooth functioning, the increase in practice for the referral organization as well as for the personnel involved in this activity should be acknowledged. These challenges should be anticipated and evaluated to ensure the sustainability of the teleradiology project.
These are the issues of the teleradiology tool, already widely established in parts of France demonstrating its efficacy when well used. At the moment the French Society of Neuroradiology (Société Française de Neuroradiologie, SFNR) is working on the creation of a charter, the goal of which is to help establish and support teleimaging networks involved in acute stroke management across France.
Dr. Nadya Pyatigorskaya is a fellow of the neuroradiology department at Pitié Salpêtrière University Hospital in Paris. Assisting with this article were Dr. Myriam Edjlali-Goujon, Diagnostic Neuroradiology, Sainte-Anne Hospital, Paris, and Dr. François Cotton, Radiology, Lyon-Sud Hospital, Pierre-Bénite.
Editor's note: This is an edited translation of an article published in French on 16 October 2015 by le Quotidien des JFR (Journées Françaises de Radiologie Diagnostique et Interventionnelle), the daily newspaper of the French national congress of radiology. Translation by Frances Rylands-Monk.










![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)






