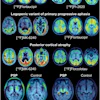
Through weight changes and tumor shrinkage, patients undergoing radiotherapy for head and neck cancer are particularly prone to variations in anatomy over a treatment course. Combined with uncertainties in treatment setup and steep dose gradients used to cover the tumor and spare sensitive structures, the changes can result in dose distributions that deviate significantly from the original treatment plan.
A European collaboration has retrospectively quantified the dosimetric impact of the uncertainties on intensity-modulated x-ray (IMXT) and proton therapy (IMPT) plans, using megavoltage images acquired over the treatment courses of five patients. The study is one of a small number to use treatment images to assess the effects on IMPT plans. Significant deviations from the planned treatments were observed, particularly for protons, demonstrating the importance of image guidance.
 First author Birgit Müller from Technical University Munich (TUM).
First author Birgit Müller from Technical University Munich (TUM)."We would like to create awareness of the dosimetric consequences of anatomical changes and misalignments in every staff member who is involved in treatment plan creation or actual irradiation," said first author Birgit Müller, of Technical University Munich (TUM), who worked on the study with colleagues at TUM and collaborators at the Institute of Cancer Research and Royal Marsden Hospital in London and Johannes Kepler University in Linz, Austria.
The patients had already received postoperative tomotherapy at the TUM Rechts der Isar Hospital. Seven-field IMXT and three-field IMPT plans were prepared for each, calculated using megavoltage CT scans acquired immediately before irradiation at the first fraction. Each plan was optimized using the same constraints and recalculated for the anatomy and setup observed in weekly megavoltage CT scans acquired over the 25-fraction treatment courses. Photon plans were evaluated in terms of absorbed dose. Proton absorbed doses were weighted with a relative biological effectiveness of 1.1 (Physica Medica, May 2015, Vol. 31:3, pp. 266-272).
Patient-to-patient variation
The nature and extent to which dose fluctuated varied significantly between patients and plan recalculations, the researchers found. For some individuals and recalculations, changes in dose over the treatment course were much larger than in others.
Contrary to the researcher's expectations, dose distributions did not show a universal, progressive deterioration over the course of treatment. In some instances, improvements were observed as treatment progressed.
Further investigation did not reveal any conclusive explanation of the variability, in part due to the small cohort size. For example, the patient with the most stable weight did not have the most stable dosimetry.
Examining dose coverage of the planning target volume (PTV), the researchers found deteriorations in both photon and proton treatments upon recalculation. However, IMPT plans tended to have greater dose inhomogeneity and a higher risk of underdosage. The range in minimum PTV dose over each treatment course, averaged over all patients, was 0.90 ± 0.31 to 1.46 ± 0.13 Gy (plan dose: 1.68 ± 0.03 Gy) in the IMPT plans. In the IMXT plans, it was 1.08 ± 0.44 Gy to 1.54 ± 0.09 Gy (plan dose: 1.57 ± 0.05 Gy).
In almost all cases, doses received by the parotid glands and spinal cord were several times lower in the IMPT plan than the IMXT plans, due to the steep drop-off in dose provided the Bragg peak. However, for the same reason, IMPT plans also tended to exhibit greater variations in OAR doses over the course of treatment as treatment geometry changed.
Importance of image guidance
The study provides further evidence of the need for accurate and frequent treatment imaging, particularly in proton therapy. Though time-consuming, plan recalculation using treatment images is also a valuable, objective tool in predicting deterioration in tumor coverage and OAR sparing, according to Müller. Currently, many facilities rely on visual assessment of treatment images by clinicians. "Dose changes are often not predictable just by looking at the CT and volumetric changes [in anatomy]," she told medicalphysicsweb.
Plan adaptation could reduce the impact of anatomical changes. However, due to the complexity of the problem, anatomical criteria that determine when adaptation is necessary have not yet been identified and further research is needed, Müller said. "There are many different interactions and patient dependencies that contribute to the dosimetric changes."
© IOP Publishing Limited. Republished with permission from medicalphysicsweb, a community website covering fundamental research and emerging technologies in medical imaging and radiation therapy.