
Research conducted in Dublin finds the breast MRI recall rate is 10.8%, which compares well with other published data but is above U.K. national breast screening guidelines' minimum standard of less than 10% and an expected standard of less than 7%. Is that achievable? Maybe.
Breast MRI is a screening tool used for surveillance in patients at high risk of developing breast cancer. Its benefits include high sensitivity and the absence of radiation, which is of particular relevance in young women who require lifelong or long-term surveillance, said Dr. Nuala Healy, a specialist registrar in radiology from St. James's Hospital in Dublin, at last month's ECR 2015.
The study cohort included women with a known gene mutation such as BRCA1 or BRCA2, women with a known first-degree relative with a gene mutation but who themselves were untested, women with a history of chest wall radiation, and women with a high lifetime risk of developing breast cancer as determined by the breast clinic. Surveillance MRIs are beneficial for these women, but they also inevitably lead to detection of lesions that are incompletely characterized on MRI, Healy explained.
"This leads to recall with further imaging with ultrasound or mammogram, and may lead to biopsy," she said. "High recall rates are associated with increased patient anxiety. In addition, there are also negative implications for the breast radiologist department in terms of increased workload and healthcare costs."
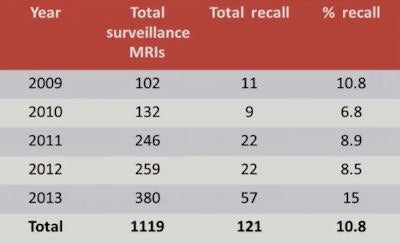 Recall rates over the five-year period. Image courtesy of Dr. Nuala Healy.
Recall rates over the five-year period. Image courtesy of Dr. Nuala Healy.Healy and colleagues reviewed all surveillance breast MRIs performed at St. James's between January 2009 and December 2014 to determine their recall rate and compare it with the current standards. A secondary objective was to determine the cancer detection rates.
Of the 1,119 surveillance breast MRIs performed over the five-year period, 121 patients were recalled for further imaging, for a rate of 10.8%. Also, 74 patients, or 61% of recalls, were in the prevalent round of screening. In other words, this was their first surveillance breast MRI.
"There is no general consensus on recall rates in breast MRI," Healy said. "Various papers describe multiple recall rates. An example of this is the Ontario breast screening program, which received a 15.1% recall rate in their prevalent round of screening. Our cancer detection rates [1.7%] appear quite low, but they are actually similar to those reported by other groups."
Regarding study specifics, all breast MRIs were performed according to a standard departmental protocol on a 1.5-tesla MRI system using a dedicated breast coil. They were reported by a single breast radiologist. All MRIs were given a BI-RADS score. For patients with a BI-RADS score of 0, 3, 4, or 5, additional imaging, modality of biopsy, and histology were recorded.
The researchers found their total surveillance breast MRI rate increased over the five-year period.
In 2013, the percentage recall rate was slightly higher, which the researchers think can be attributed to higher levels in the prevalent round of screening in that year.
In terms of biopsies, 71 biopsies were performed at the recall rate -- the majority of which were ultrasound-guided (92%), followed by MRI-guided (7%), and stereotactic-guided (1%). In the recall group, 19 cancers were detected in the recall group, for a malignancy detection rate of 1.7%. Reviewing the histology of the biopsies revealed the majority of malignancies were invasive ductal carcinoma (12 patients), followed by ductal carcinoma in situ (five patients) and invasive lobular carcinoma (two patients).
Given all this, how may recall rates be reduced? First of all, breast MRIs should be read by breast radiologists with experience with reporting on the modality, Healy said. Second, double reading would help, as would the use of automated software as an adjunct. There should also be a careful review of prior imaging and determination if prior imaging was performed at an external institution to limit recall rates.








![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)








