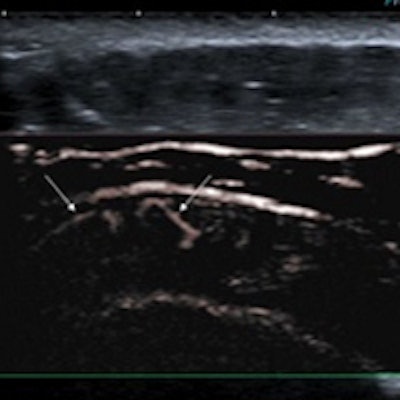
A new Doppler ultrasound technique can provide better visualization of low-grade inflammation in joints and tendons than power Doppler ultrasound, yielding clinical information that often influences patient management, a team of U.K. researchers recently found.
The technique, called Superb Micro-Vascular Imaging (SMI, Toshiba Medical Systems), offered better visualization of microvasculature, enabling the detection of low-grade inflammation not previously identified with power Doppler, concluded Dr. Adrian Lim, from Imperial College Healthcare National Health Service (NHS) Trust, and colleagues.
"This has significant clinical impact, leading to a change in management in 25% of our patients in this study population," said Lim, who presented the research at the RSNA 2014 meeting in Chicago.
Power Doppler ultrasound is currently the modality of choice for assessing joint and tendon inflammation, offering an easier, more accessible, and much cheaper method than contrast-enhanced MRI, he said. Doppler ultrasound technology continues to improve, however, and SMI is designed to visualize the microvasculature without the need for ultrasound contrast.
Conventional ultrasound filters remove clutter in the image, but in the process they also remove slow-moving vessels, as they can't discriminate between similar features of clutter and clinical data. In contrast, the SMI algorithm analyzes unique and distinct features of clutter in images, isolating and then removing clutter without compromising valuable clinical information, according to Lim.
The researchers set out to assess the efficacy of SMI in detecting low-grade inflammation in the joints and tendons, comparing its performance with conventional power Doppler ultrasound. The study population consisted of 77 patients who presented for musculoskeletal ultrasound at Charing Cross Hospital between July 2013 and June 2014. Patients were included in the study if they demonstrated changes on B-mode ultrasound, signal on power Doppler, or signal on SMI.
The subjects had a mean age of 44 years (range, 29-81 years), and there were 20 men and 57 women. In all, 98 joints and 18 tendons were imaged.
An Aplio 500 ultrasound scanner (Toshiba) with an 18-MHz probe was used to obtain ultrasound video clips and images. One of three radiologists with more than 10 years of musculoskeletal ultrasound experience independently read the studies and determined if vascularity was seen in the joints or tendons with power Doppler, SMI, or both methods.
If signal was detected with both power Doppler and SMI, the readers were asked to provide a score for whether SMI was no better, mildly better, moderately better, or markedly better than power Doppler based on the sensitivity and spatial resolution of the images. They also documented whether a change in patient management occurred based on the SMI results.
While flow was demonstrated on both power Doppler and SMI in 58 cases, SMI alone showed vascularity in 40 cases. No cases of vascularity were shown on power Doppler but not on SMI. In 18 cases, no flow was detected by either technique. This difference in performance between power Doppler and SMI was statistically significant (Fisher's exact test: p < 0.001).
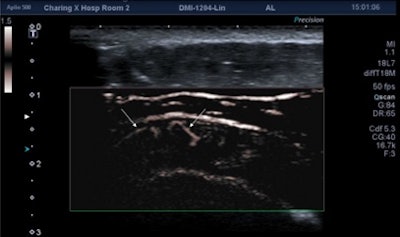 Acute case of supraspinatus tendinitis. SMI shows abnormal microvasculature (arrows) within the inflamed tendon. Image courtesy of Dr. Adrian Lim.
Acute case of supraspinatus tendinitis. SMI shows abnormal microvasculature (arrows) within the inflamed tendon. Image courtesy of Dr. Adrian Lim.In more than half the cases where flow was identified using both techniques, SMI was judged to be either moderately or markedly better than power Doppler. This difference was also statistically significant (p = 0.02).
Of the 40 cases where vascularity was observed only with SMI, management was changed for 19 patients (24.7% of overall patients), who then received ultrasound-guided steroid injection, oral analgesia, and/or disease-modifying treatment, according to the group. The researchers also noted excellent interobserver agreement with SMI (kappa = 0.85-0.92 for all three readers).
"[SMI] allows detection of low-grade inflammation of joints and tendons not previously possible with power Doppler and without the need for ultrasound contrast," Lim said. "This leads to earlier detection and treatment with steroids or [disease-modifying antirheumatic drugs] and may help with prognosis and prediction of relapse in patients with arthritis."











![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)




