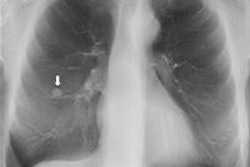
A new study by Swedish radiologists performed under real-world conditions indicates that digital chest tomosynthesis can replace CT for a number of lung exams, saving both money and radiation dose. The research confirms previous studies on the role tomo can play in carving out a middle ground between CT and conventional chest x-ray.
Researchers from Sahlgrenska University Hospital and the University of Gothenburg reviewed their department's experience with tomosynthesis after installing a system in December 2006. They examined the cases of 149 patients for whom digital chest tomosynthesis was used according to the clinical criteria of their hospital and calculated whether tomo was beneficial or detrimental.
The upshot? Digital chest tomosynthesis obviated the need for CT in 80% of cases in which CT would have been used, and it reduced the average radiation dose experienced by the entire patient population to just 25% of what it had been previously, according to lead author Dr. Ase Johnsson, PhD, and colleagues. The study was published online on 2 August in Academic Radiology.
An intermediary role
Much of the recent research on digital chest tomosynthesis has focused on the technology playing an intermediary role between chest radiography and CT. Conventional radiography has notoriously poor sensitivity for lung nodules, leaving many patients to be sent on to CT, where suspicious lesions are often found to be benign. Could tomo help resolve some of these cases?
Johnsson and colleagues decided to review their experiences with patients who received tomosynthesis studies since the 2006 installation of their system (VolumeRad, Definium 8000, GE Healthcare). Such a study could help fill a gap in the literature regarding the use of tomosynthesis on a routine clinical basis, they believed.
Mining the hospital's PACS database for tomosynthesis cases revealed 149 patients who had received tomosynthesis exams in March 2010 after suspicious nodules were detected on conventional chest x-rays. This particular time period was selected because by then clinical use of tomosynthesis at Sahlgrenska University Hospital had stabilized. It also enabled the acquisition of follow-up data in the three years between the study period and when the paper was written.
Data were collected on the type of referral for tomosynthesis (whether it came from a radiologist or a clinician), patient demographics, clinical indication, radiation dose, and any radiology follow-up exams that were required. Tomosynthesis exams were acquired at 120 kV using 60 low-dose projection radiographs with a 5-mm section thickness.
The value of digital chest tomosynthesis was evaluated based on two main criteria: whether it obviated the need for a CT scan, and to what extent it reduced the total radiation burden experienced by patients.
For the first part of the study, two experienced thoracic radiologists reviewed each tomosynthesis case, first deciding whether CT would have been performed if tomosynthesis had not been an option. Then they decided whether the tomo study was adequate, based on patient characteristics as well as clinical and radiological information available before the exam.
In 100 cases, CT would have been required for workup if tomosynthesis were not available, the researchers found; 80 of these could be followed up with tomosynthesis instead, meaning that tomo obviated the need for CT in 80% of the cases. For the remaining 49 exams, CT never would have been considered.
For the 100 cases in which CT would have been performed, tomosynthesis was judged to be beneficial in 85% of cases, neutral in 13%, and detrimental in 2%. In the latter two cases, tomosynthesis was found to have missed a tumor later detected on bronchoscopy, and a CT exam found a metastasis missed by tomo. In the 13 neutral cases, tomosynthesis was unable to answer the clinical question, and patients were sent on to CT.
Impact on radiation dose
In the second part of the study, the researchers analyzed the effect of tomosynthesis on radiation dose. They calculated dose for two scenarios: one represented the actual situation in their department, where tomosynthesis is available, while the other was a hypothetical situation in which tomo was not in use.
For the actual situation, Johnsson and colleagues recorded a mean effective dose of 0.14 mSv for tomo exams referred by radiologists and 0.18 mSv for studies referred by clinicians. In comparison, the mean effective dose for chest CT scans was 7.1 mSv (range, 3.2-14.2 mSv).
Under the hypothetical situation with no tomosynthesis, for the 76 cases referred by clinicians, radiation dose was almost 4 mSv higher per case because CT would have been used for 54 cases when tomosynthesis was not available, according to the authors. For the 73 radiologist-referred cases, 26 patients would have received a 4-mSv CT scan.
For the entire study population, the use of tomosynthesis decreased the average effective radiation dose from 2.7 mSv to 0.7 mSv.
Interestingly, the researchers found a major discrepancy in the utility of tomosynthesis based on whether the referring physician was a clinician or a radiologist. Some 91% of the clinical referrals never would have progressed to CT if tomosynthesis were not available, while 42% of the radiologist referrals still would have gone on to CT after the tomo exam was performed.
The researchers speculated that the threshold for ordering a tomosynthesis study was lower than for CT at their institution, perhaps due to awareness of tomo's lower radiation dose and the fact that tomo studies are performed immediately after the chest x-ray, Johnsson said in an email to AuntMinnieEurope.com. Even in this scenario, tomosynthesis seems to be used judiciously.
"In our clinical practice, the patient stays at the department until the [chest x-ray] has been reviewed so that supplemental projections or [tomosynthesis] can be performed directly," the authors wrote. "However, the use of [tomosynthesis] has not escalated and less than 10% of the [chest x-ray] examinations are supplemented by [tomosynthesis]."