
Momentum is building for ultrasound-guided venipuncture, not least because using a wireless probe can transform practice, according to researchers from Madrid who presented their results at this week's European Society of Cardiology (ESC 2014) annual meeting.
In a pilot study, the team from Ramón y Cajal University Hospital reported no impact on workflow versus the use of traditional wired probes, and no impact on image quality, but a far easier and more intuitive experience compared with a traditional wired ultrasound probe for venous access of the femoral vein.
 Dr. Daniel Rodriguez Muñoz.
Dr. Daniel Rodriguez Muñoz.Ultrasound guidance is recommended for venous access owing to several studies demonstrating that it's more accurate in targeting the vein than navigating by landmarks -- that is, by looking for visible veins without the aid of imaging. But in an interview with AuntMinnieEurope.com, lead author Dr. Daniel Rodriguez Muñoz said the traditional way of doing ultrasound-guided venous access is so cumbersome that practitioners would rather take their chances by just stabbing for their target unaided.
"Despite the recommendation that it's safer to perform vascular access guided by ultrasound, in most centers, including mine, it was not performed in a systematic way," he noted. "In most cases, that was just anatomical landmark locations and puncturing where you think the vein is going to be."
Muñoz, a fifth-year cardiology fellow, said it's obvious that using ultrasound for the procedures boosts accuracy, but with wires involved it's too complex and time-consuming to bother with.
"Right now if you want to use vascular ultrasound guidance for a procedure when the physician enters the room you have to take a sterile plastic bag and ask someone else to put the probe, which is not sterile, inside the bag along with the wire," he said, adding that touching it may compromise sterility. "That takes some time, and it has been suggested as a reason for low adoption and integration of ultrasound guidance."
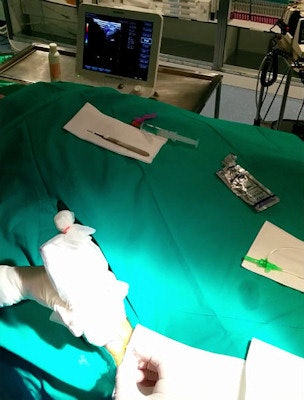 Wireless ultrasound probe used to visualize vein in the right femoral artery. All images courtesy of Dr. Daniel Rodriguez Muñoz.
Wireless ultrasound probe used to visualize vein in the right femoral artery. All images courtesy of Dr. Daniel Rodriguez Muñoz.But Muñoz, along with Prof. José Zamorano and colleagues, found that wireless guidance makes it easier, and the group's initial experience on several cases, now submitted for publication, shows virtually no differences compared with the wired ultrasound exam, except that it's simpler and probably faster. They used the Acuson Freestyle Ultrasound System (Siemens Healthcare) and its cable-free transducer on 18 cases performed by one attending physician, two fellows, three residents, and two vascular surgeons, who each tried ultrasound-guided access to the right femoral vein in three or four cases.
They interviewed the physicians about several aspects of the exam, regarding workflow, image quality, and whether it interfered with the procedure:
Overall procedure interference was rated at 0.75/5 with wireless ultrasound -- a score of 1 represents very low interference
Overall image quality was rated 3/5 (i.e. equivalent to wired ultrasound)
Overall perception of delay in transmission versus wired ultrasound was rated at 0.5/5 -- meaning no perceptible delay using wireless by any practitioner
There was one adverse event when a patient suffered an inadvertent arterial puncture that went unnoticed during the procedure, Muñoz said. The patient was admitted and a blood panel showed a drop in hemoglobin as a result of the error.
Overall, however, the probe made the difference between ultrasound guidance being not worth it and being a real help in the ward, he explained.
 Siemens Healthcare's Acuson Freestyle ultrasound system, untethered to the central unit.
Siemens Healthcare's Acuson Freestyle ultrasound system, untethered to the central unit."When the physician enters the room, the probe is already inside the sterile pack, and the sterile gel is already on top of the sterile field, and all you have to do is take the probe and put it on top of the leg of the patient, see what you have, and puncture, which is more or less the same amount of time you would use for just the landmark anatomical locations," he said.
Also, the practitioner can adjust all of the image settings because the probe has controls, he said, meaning there's no need to have an extra person on hand to help adjust the gain, color, or depth of the image on the central unit.
Put it all together and the system has been a hit, which bodes well for participation in ongoing studies, Muñoz said.
"Six months after we started using it, everyone in our electrophysiology lab was actually using it, and when we didn't have it available, people asked for it," he said. "That didn't happen when we tried to start using the conventional wired probe with the ultrasound, because it was annoying, and took a significant amount of time."



















