Healthcare IT is undergoing a painful evolution. Spurred by spiraling healthcare costs, healthcare providers are waking up to the reality that their sector is lagging behind. Radiology to date has tended to be ahead of the curve in adoption of healthcare IT, evident in the widespread implementation of PACS. But heavy reliance on PACS and stubborn resistance to broader cooperation with other hospital stakeholders is slowing healthcare IT development. Below, we take a quick look at the dynamic changes taking place in this rapidly evolving industry.
PACS
PACS offered radiology a glimpse into the future. The ability to archive, query, annotate, and share images across departments and clinics was the first building block of the "digital hospital." Keen to be at the forefront of cutting-edge technology, radiologists embraced PACS. Jargon-heavy upgrades, touting "game-changing" solutions and "transformational" image sharing capabilities continued to drive momentum for larger and more complex PACS. Yet, PACS was originally a single-department concept -- it was never intended to provide interoperability at the multidepartment or multisite level. Therefore, as demand for IT systems outside of the radiology department has grown, new solutions for the broader need have emerged.
Vendor-neutral archiving (VNA)
The need for digitalization across the hospital conceived VNA storage. While VNA is often bound to many solutions, a true VNA offers widespread use for all file formats, allowing storage of DICOM and non-DICOM fi les. Each hospital department has its own specific need and requirements for IT system and storage. The majority opt for specialist vendor solutions, regardless of whether this connects well with other departmental systems or storage. This produces a complex hospital IT ecosystem with few common vendors or system types. While there is a trend toward centralized hospital contracting for IT in a bid to reduce cost, many users are unwilling to change to a less specialist vendor. Therefore VNA is the only sensible IT storage solution that allows each department still to maintain a semidiscrete status. It's also one of the few current solutions that fit the future long-term development of healthcare IT.
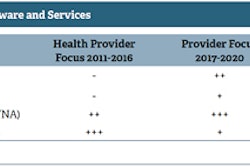
![Revenues [$ millions] - includes new systems and maintenance. Source: IHS.](https://img.auntminnieeurope.com/files/base/smg/all/image/2014/03/ame.2014_03_21_11_01_21_519_2014_03_24_PACS_VNA.png?auto=format%2Ccompress&fit=max&q=70&w=400) Revenues [$ millions] - includes new systems and maintenance. Source: IHS.
Revenues [$ millions] - includes new systems and maintenance. Source: IHS.Big data and health information exchange
The biggest challenge for healthcare IT improvement is bringing together various healthcare IT systems to a point where interoperability of data is commonplace. Yet, combining each discrete data element into a centralized "big data" silo could have revolutionary consequences for the provision of healthcare.
Large-scale health data interoperability, often referred to as health information exchange (HIE), is touted as offering game-changing benefits for patients and providers alike. The ability to pull patient records and history between hospital, regions, or country improves administration, billing, and clinical treatment. Patients with pre-existing conditions could even carry their records and history with them on smartphone devices. Furthermore, pooling of healthcare data also offers real clinical benefits. Tracking of disease prevalence and epidemiology on a large scale could bring about new care protocols, decision support for diagnosing physicians, and new globalized standards in treatment. Healthcare spending could also be managed more efficiently; resources, supplies and expertise could be more accurately monitored, analyzed, and actioned based on large-scale data evidence.
The challenge ahead
Admittedly, seamlessly integrated HIE still has a long way to go, with only a few subregional or multihospital systems in place currently. Rollout of such systems has huge barriers to face including patient confidentiality, public and private integration, governmental, state and hospital level regulation, not to mention the sheer cost of upgrading existing IT and connectivity infrastructure to manage such a complex system.
Yet, scaling such challenges must begin with overcoming smaller barriers toward a common goal -- HIE rollout. Overreliance and use of PACS as a storage solution is one such barrier that is simpler to correct.
Stephen Holloway is the associate director of medical devices and healthcare IT research at IHS. He can be reached at [email protected].
The comments and observations expressed herein do not necessarily reflect the opinions of AuntMinnie.com, nor should they be construed as an endorsement or admonishment of any particular vendor, analyst, industry consultant, or consulting group.
Originally published in ECR Today on 9 March 2014.
Copyright © 2014 European Society of Radiology