Multislice CT (MSCT) is a noninvasive and accurate way to detect postoperative complications in liver transplant recipients and the best option for confirming vascular complications, according to a new study by researchers from Egypt.
There is a heavy burden of chronic liver disease in Egypt due to the prevalence of hepatitis C virus infection, study author Dr. Omar Abdelaziz, from the department of diagnostic and interventional radiology at Cairo University, told AuntMinnie.com.
 Dr. Omar Abdelaziz from Cairo University.
Dr. Omar Abdelaziz from Cairo University.
The living donor liver transplantation (LDLT) program began in Egypt in 2001, and since its initiation more than 1,500 cases have been performed.
"As a part of the LDLT team in our institution, we decided to conduct this study to emphasize the role of MSCT for assessment of different postoperative vascular and nonvascular complications," Abdelaziz said.
Reducing complications
Postoperative complications significantly affect the morbidity and mortality of liver transplant recipients, the authors wrote. These complications are significant despite great technological and immunological advances in medicine (Egyptian Journal of Radiology and Nuclear Medicine, December 2013, Vol. 44:4, pp. 697-704).
The goal of imaging is to identify vascular and biliary complications, they noted, adding that long-term follow-up allows clinicians to identify recurrence of the primary disease and/or detect disease related to long-term immunosuppression.
While different imaging modalities are used during follow-up, multislice CT has recently been accepted as a practical, noninvasive diagnostic method. Doppler ultrasonography is portable, inexpensive, and noninvasive, but its accuracy depends on the technical experience of the operator and the condition of the patient. And while conventional angiography is the gold standard for diagnosis, it is not ideal for screening because of its high cost, invasive nature, and associated risks and potential complications.
"The excellent spatial and temporal resolution combined with postprocessing of the imaging data using a variety of 3D reformatting techniques allows MSCT to depict both hepatic anatomy and pathology efficiently and accurately," the authors wrote.
New advances in MSCT technology allow for good recipient and donor preoperative assessment with positive effects on surgical outcome and graft survival, according to Abdelaziz. After the operation, the use of MSCT improves the early detection of complications in the recipient, especially vascular complications.
In the current study, Abdelaziz and colleagues assessed 33 patients (28 men and five women) between the ages of 38 and 63 years who underwent living donor liver transplantation. All patients were referred to their radiology department between November 2009 and June 2012 for further evaluation of vascular, biliary, parenchymal, and abdominal complications.
The 33 patients underwent MSCT of the abdomen using a 64-detector-row scanner. All images were transferred to a workstation for postprocessing. Multiplanar reconstruction (MPR) and 3D maximum intensity projections (MIPs), volume rendering, and curved planer reformations were performed for all patients.
Sixteen out of the 33 cases were referred for assessment of vascular complications where Doppler ultrasonography was either inconclusive or required further definite diagnosis by MSCT angiography.
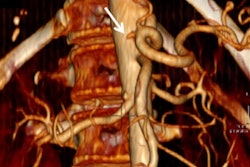
The researchers found vascular complications in all 16 patients, including eight cases of hepatic artery thrombosis, one case of hepatic artery stenosis, three cases of portal vein thrombosis, two cases of portal vein stenosis, and two cases of hepatic vein stenosis.
Abdelaziz said they were surprised by the high percentage of vascular complications encountered. However, this can be explained by the fact that their department is a referral center due to the availability of interventional radiological facilities and experienced personnel for managing emergency vascular complications.
It's important to note the high accuracy of MSCT angiography for assessing vascular complications, he added.
"It is the first imaging modality [to use] if vascular complication was suspected by color Doppler," he said. "Digital subtraction angiography is reserved if therapeutic intervention is contemplated."
In addition, MSCT can be used in the guidance of different percutaneous interventional procedures, Abdelaziz said.
The study authors noted that diagnosis of vascular complications is particularly important because early radiological or operative intervention may allow graft salvage.
When it came to biliary complications, Abdelaziz and colleagues found nine cases, including six of biloma and three of biliary stricture. The three cases of biliary stricture needed further evaluation by MR cholangiopancreatography (MRCP) to confirm diagnosis.
While the diagnostic accuracy, sensitivity, and specificity of MSCT angiography for the detection of various vascular complications was 100%, the study results show the inherent weakness of MSCT in identifying and characterizing biliary stricture, according to the authors.
This finding is in accordance with previous research that found MSCT to be less sensitive for assessing biliary complications and recommended MRCP instead.
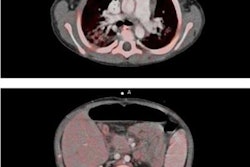
Parenchymal complications included two cases of hepatic abscesses and two cases of acute liver rejection, and recurrence of hepatocellular carcinoma was seen in three patients. As for abdominal complications, one patient developed non-Hodgkin's lymphoma one year after transplantation.
Radiologists must be aware of the initial Doppler ultrasonography findings and choose the next imaging modality based on those results, Abdelaziz noted. For example, if vascular complication is suspected, MSCT is mandatory, whereas if biliary complication is suspected, MRCP is the examination of choice.
MSCT provides synchronous evaluation of the hepatic vasculature, biliary tract, liver parenchyma, and the other abdominal organs in a single examination and is the best option for confirming suspicion of vascular complications, the authors concluded.