
A total of 90 confirmed cases of Middle East respiratory syndrome (MERS) have now been reported worldwide, including 45 deaths. All patients have been linked to Saudi Arabia, Jordan, Qatar, and United Arab Emirates, but cases have emerged in France, Germany, Italy, and the U.K., researchers report in an article to be published online on 26 July by Lancet Infectious Diseases.
But experts insist the situation is firmly under control and is very unlikely to develop into an epidemic. They have appealed for calm, although they have urged radiologists and others to remain vigilant.
The new study -- the largest case series to date -- includes 47 cases (46 adults, 1 child) of confirmed MERS coronavirus (MERS-CoV) infections from Saudi Arabia between 1 September 2012, and 15 June 2013. By combining clinical records, lab results, and imaging findings with demographic data, the authors noted older patients, especially men, and patients with underlying medical conditions, tend to succumb to the disease.
','dvPres', 'clsTopBtn', 'true' );" >
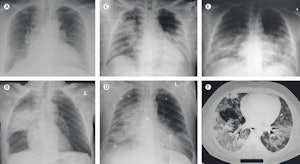
Click image to enlarge.
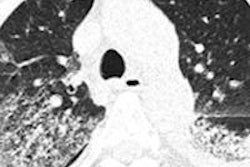
Imaging findings at presentation in Saudi patients with MERS. All images courtesy of Lancet Infectious Diseases.
As with severe acute respiratory syndrome (SARS), MERS infections presented with a diverse range of symptoms. Most patients admitted to hospital exhibited fever (98%), chills/rigors (87%), cough (83%), shortness of breath (72%), and muscle pain (32%). A quarter of patients also experienced gastrointestinal symptoms, including diarrhea and vomiting. But in contrast to SARS, most cases (96%) occurred in people with underlying chronic medical conditions including diabetes (68%), high blood pressure (34%), chronic heart disease (28%), and chronic renal disease (49%).
"Despite sharing some clinical similarities with SARS (e.g., fever, cough, incubation period), there are also some important differences such as the rapid progression to respiratory failure, up to five days earlier than SARS," explained Dr. Ziad Memish, deputy minister for public health from Saudi Arabia, who led the research along with Dr. Abdullah Assiri, from the Global Center for Mass Gatherings Medicine, Ministry of Health in Riyadh. "In contrast to SARS, which was much more infectious especially in healthcare settings and affected the healthier and the younger age group, MERS appears to be more deadly with 60% of patients with coexisting chronic illnesses dying, compared with the 1% to 2% toll of SARS."
The high mortality rate with MERS is probably spurious because doctors are only picking up severe cases and missing a significant number of milder or asymptomatic cases, but so far there is little to indicate that MERS will follow a similar path to SARS, he added.
The first two known patients with MERS-CoV infection (diagnosed retrospectively) died in April 2012 at a public hospital in Zarqa, Jordan. In Saudi Arabia, 70 cases have been reported to date. Some cases of MERS-CoV infection have occurred in travelers returning from the Middle East and in their close contacts, suggesting person-to-person transmission. This type of transmission was confirmed by genome sequencing of MERS-CoV isolates from the Al-Hasa healthcare-associated outbreak, the authors noted.
Radiological aspects
Because the x-ray and CT features of MERS-CoV are not different from any case of pneumonia, the best thing radiologists can do is to alert the physicians and have a high degree of awareness of the possibility of MERS-CoV infection in any case of pneumonia, according to co-author Ali Zumla, PhD, a professor of infectious diseases and international health at University College London. A detailed history of travel to the Arabian Peninsula may point toward the possibility of MERS-CoV infection, he added.
"Like any other chest infection, there is no imaging modality that can help make a specific diagnosis. Any changes in the imaging should be followed up by a request for a MERS-CoV-specific diagnostic test, including tests to rule out bacterial and other viral causes of pneumonia," he told AuntMinnieEurope.com.
MERS-CoV is unlikely to spread as rapidly as SARS did, he added. MERS-CoV was first identified 15 months ago, and there have been only 90 cases reported so far. SARS spread rapidly, and within the epidemic, there were 8,000 cases and approximately 800 deaths. Also, a French scientist who specializes in modeling epidemics has concluded that at the rate at which new cases are being detected, there is only a remote possibility of it becoming an epidemic.
"It is very unlikely any epidemic will ensue. The public needs to be reassured," Zumla explained. "Standard infection-control precautions for travelers should be followed, as stated by the Saudi Arabian government guidelines."
The Saudi government has screened more than 3,000 contacts (family members, workmates, hospital staff) of patients with MERS-CoV infections. Of these, they detected seven people who had mild flu-like symptoms and recovered fully in a few days. This suggests doctors have only noticed the more serious cases who are admitted to hospital, and it seems that, in most cases, MERS-CoV may be a mild illness, he said.
Saudi Arabia has had 5 million pilgrims come to Makkah and Madinah over the past 15 months, yet there have been only 70 cases of MERA-CoV so far, Zumla stressed. Currently, there are 2 million pilgrims who have come from more than 180 countries for the month of Ramadan, and there have been no cases of MERS-CoV. This reassures everybody that MERS-CoV does not constitute a public health emergency and the public must be reassured, he noted.
Transmission in Europe
To date, there have been three cases in the U.K. (all of whom died), three cases in Italy, two cases in France (one of whom died), and two cases in Germany, according to Zumla. These occurred in returning travelers from the Middle East or in patients who were contacts of patients with MERS-CoV in European hospitals.
In the U.K., MERS-CoV was transmitted to a family member who visited a patient with confirmed infection. A recent report from France also described patient-to-patient nosocomial transmission of MERS-CoV. A 64-year-old French man with a renal transplant fell ill with diarrhea and fever a week after returning from Dubai. Pneumonia was an incidental finding on chest radiography, and he subsequently developed severe respiratory disease, from which he died. A second case of MERS-CoV infection was diagnosed at the same hospital in a patient on long-term steroid treatment. The respiratory presentation of the case suggests transmission in the hospital room shared by both patients.
"The main findings of our study are that most patients present with serious respiratory disease, need to be admitted to hospital, and 60% of them die," the authors stated in Lancet. "Adults of both sexes are affected, at a mean age of 56 years (range 14-94)."
Further case-control studies are needed to define the effect of comorbidities on susceptibility to and associated mortality from MERS-CoV infection, they continued. In addition, long-term sequelae of patients who recover from acute MERS are not yet known and must be defined. Apart from enhanced and active surveillance for cases, rapid, accurate, serological diagnostic tests should be developed, and important questions about transmission, risk factors, clinical course, and natural history of MERS-CoV infection need to be addressed.
"The recent identification of milder or asymptomatic cases of MERS in healthcare workers, children, and family members of contacts of MERS cases indicates that we are only reporting the tip of the iceberg of severe cases and there is a spectrum of milder clinical disease, which requires urgent definition. Ultimately, the key will be to identify the source of MERS infection, predisposing factors for susceptibility to infection, and the predictive factors for poor outcome. Meanwhile, infection-control measures within hospitals seem to work."
Writing in a linked editorial, Dr. Christian Drosten, head of the Institute of Virology at University of Bonn Medical Center in Germany, emphasizes the urgent need for accurate diagnostic tests to help focus control efforts and minimize the risk of spread. "To ascertain relevant data for MERS epidemiology, we need to develop serological assays using samples from well-defined groups of patients. Population-based antibody testing could establish the extent of MERS-CoV infection, instead of only seeing the tip of the iceberg."
It is important to bear in mind that clinical follow-up of patients who recovered from SARS shows radiological, functional, and psychological abnormalities of varying degrees, Assiri, Memish, and colleagues noted. In the early rehabilitation phase, many patients complained of limitations in physical function from general weakness or shortness of breath. Lung function testing six to eight weeks after hospital discharge showed a mild or moderate restrictive pattern consistent with muscle weakness in 6% to 20% of individuals. Psychobehavioral problems such as anxiety and depression were not uncommon in the early recovery phase and improved over time for most patients, they wrote.










![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)




