Benign breast surgery decreases breast cancer screening sensitivity, probably due to postoperative mammographic changes, Dutch researchers have found.
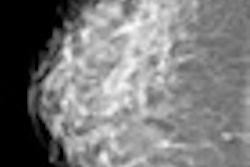
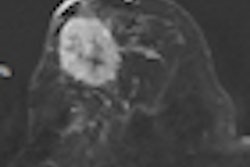
Mammographic interpretation after conservative breast surgery and radiotherapy is frequently hampered by the presence of scar formation, contour deformity of the breast, thickened Cooper's ligaments, skin thickening, and calcifications. While European countries and the U.S. have screening recommendations after breast-conserving surgery for malignant disease, not much exists for benign breast surgery. Benign breast surgery -- such as excisional biopsy and breast reduction surgery -- also leads to permanent postoperative mammographic changes in up to 50% of women, according to Dr. Vivian van Breest Smallenburg from the department of radiology at Catharina Hospital in Eindhoven, the Netherlands.
"A history of excisional biopsy for benign disease is associated with a higher recall rate, and we recently reported a lower sensitivity of screening mammography after previous benign breast surgery," she wrote in the September issue of the European Journal of Cancer. "However, it is not clear whether this impaired sensitivity is due to postsurgical mammographic alterations or due to specific breast tissue characteristics such as breast density or fibrocystic changes."
Van Breest Smallenburg and colleagues sought to determine exactly why breast cancer screening performance was lower after benign breast surgery. They included a consecutive series of 351,009 screening examinations in 85,274 Dutch women from January 1997 and January 2009. Two radiologists reviewed the exams of women with screen-detected cancers or interval cancers that were diagnosed after previous benign breast surgery. The radiologists also determined the presence and degree of changes after surgery, classified breast density, and determined whether mammographic interpretation was hampered by tissue characteristics. They also assessed whether the cancer had already been visible at a previous screen.
The researchers found screening sensitivity was lower in women with prior benign breast surgery than without (63.5% versus 73.5%). A total of 115 screen-detected cancers and 66 interval cancers were diagnosed in breasts after previous benign breast surgery. Also, postsurgical mammographic alterations in the part of the breast where cancer was diagnosed were more distinct in interval cancers than in screen-detected cancers.
There was an increased interval cancer risk in women with postsurgical mammographic changes at the location of the breast cancer, van Breest Smallenburg noted. Limited mammographic interpretation due to tissue characteristics was mentioned only in three screen-detected cancers and one interval cancer.
Breast density at the latest screening exam was similar for screen-detected cancers and interval cancers that had been detected in postoperative breasts and the reviewers rarely reported specific tissue characteristics such as fibrocystic disease or extensive calcifications hampered mammographic interpretation, the researchers wrote.
The proportions of screen-detected cancers and interval cancers already visible at a previous screen were comparable for women with and without prior surgery (47.5% versus 42.8% for screen-detected cancers and 50% versus 48.4% for interval cancers).
"The current study shows a lower sensitivity of screening mammography after previous benign breast surgery and we found that this lower sensitivity is most likely to be the result of postoperative mammographic changes rather than differences in breast density or the presence of specific tissue characteristics," the researchers wrote.
These findings may have implications for future screening guidelines, according to van Breest Smallenburg. "Although diagnostic surgical biopsy has largely been replaced by percutaneous biopsy techniques, 6.7% of women in our screening program currently mention a history of benign breast surgery, whereas 11.7% of women in the U.K. study of Banks et al reported previous breast surgery for conditions other than cancer."
One of the strengths of van Breest Smallenburg's study is it's the largest series of screened women who developed breast cancer after previous benign breast surgery. All screening examinations were read by two screening radiologists and from 2003 on by two mammography technicians in addition to the radiologists. There was also extensive follow-up to detect a maximum of interval cancers.
A limitation of the study includes its use of analogue screens only, whereas many screening units are now digital. The Netherlands screening program became fully digitized in 2010 and thus has resulted in higher referral rates and increased cancer detection rates, at the expense of a decreased positive predictive value of referral.
"The effect of the transition from screen film mammography to digital mammography on interval cancer rates and on cancer detection in postsurgical breasts is yet unknown," van Breest Smallenburg wrote. "Generalization of our study results may be limited by the presence of differences between our screening practice and those of other countries."
The Dutch screening program offers biennial screening, which is in contrast to the annual screening mammography recommendation in the U.S. and triennial screening in the U.K. In addition, the referral rate in the Netherlands is 1.3%, which may affect cancer detection in postsurgical breasts. Another limitation is the researchers were unable to calculate specificity as they were not informed about the total number of screened women with a history of benign breast surgery.
"At screening, utmost attention should be paid to mammographic breast segments showing postoperative changes in order to reduce the risk of interval cancer," she concluded. "In order to prevent an adverse effect on screening sensitivity, excision of breast lesions with conclusive, benign pathology at percutaneous biopsy should only be considered if a woman persists on removal of the lesion."