
A small hospital that can afford only one MR machine should not consider purchasing a 3-tesla system because it cannot cover all clinical demands. That's the clear and unequivocal advice of two senior Dutch neuroradiologists who liken the performance of an MR unit with that of a sports car.
"In a traffic jam or with bad road infrastructure, the advantages of a sports car will disappear and the driver will have to deal with substantial challenges. In those circumstances, it might be better to drive an economical car or use public transportation," noted Dr. Mike Wattjes, senior staff radiologist at the VU University Medical Centre in Amsterdam.
 The 3-tesla sports car mutates into a 7-tesla Formula One racing car, which makes daily use even more challenging, according to Dr. Mike Wattjes.
The 3-tesla sports car mutates into a 7-tesla Formula One racing car, which makes daily use even more challenging, according to Dr. Mike Wattjes.
Such adverse conditions for a sports car correspond to certain 3-tesla applications, such as spinal cord imaging, he wrote in a joint commentary published online by European Radiology on 23 July.
"Higher magnetic field strengths do not necessarily lead to a better diagnostic accuracy. Disadvantages of high-field MR systems have to be considered in clinical practice," he wrote. "Disappointingly there are few direct comparisons of 1.5-tesla and 3-tesla MRI. Whether the next high-field MR generation (7-tesla) will improve diagnostic accuracy has to be investigated."
Higher field strengths are needed for functional imaging, spectroscopy, etc., and the installation and use of high-field MR systems for research and in clinical practice have dramatically increased, conceded Wattjes and his co-author Dr. Frederik Barkhof, from the same department and institution. Given the theoretical increase in signal-to-noise ratio (SNR) compared to systems of 1.5-tesla and below, the most relevant sales pitch by vendors is the achievement of better image quality and the ability to reduce MR data acquisition and overall examination times when using 3-tesla. Extensive research demonstrates the benefits, but also the challenges of 3-tesla MRI, they noted.
In neuroradiology, the benefits of 3-tesla are quite obvious, not only to obtain better quality routine structural imaging (e.g. of inflammatory lesions), but especially for applications with inherently low SNR, such as susceptibility weighted imaging (SWI), MR angiography (MRA), diffusion tensor imaging (DTI), functional MRI (fMRI), and MR spectroscopy. "However, still up for debate is the crucial question of the diagnostic relevance of 3-tesla MRI, or in other words, 'Does 3-tesla MRI lead to a more sensitive (earlier) and/or more specific diagnosis of certain diseases?' " the authors wrote.
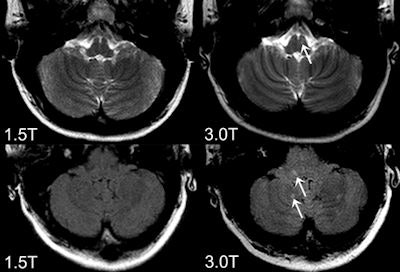 Axial FLAIR (bottom) and T2-weighted images (top) obtained at 3-tesla (right) and 1.5-tesla (left). The 3-tesla MRI shows more an inflammaory lesion in multiple sclerosis patients in the posterior fossa, which is clincially highly relevant because infratentoral lesions play an important role in the current diagnostic criteria and do have predictive value in terms of long term disability. All images courtesy of Dr. Mike Wattjes.
Axial FLAIR (bottom) and T2-weighted images (top) obtained at 3-tesla (right) and 1.5-tesla (left). The 3-tesla MRI shows more an inflammaory lesion in multiple sclerosis patients in the posterior fossa, which is clincially highly relevant because infratentoral lesions play an important role in the current diagnostic criteria and do have predictive value in terms of long term disability. All images courtesy of Dr. Mike Wattjes.The high standard of clinical trial methodology for drug testing is not transferable when comparing one diagnostic imaging method with another. Technological improvements occur continually, and it is impossible to systematically compare each new technique with an existing one, they explained. Only major steps require validation, and the discussion of the diagnostic benefit of higher magnetic field strength will shift gears when whole-body ultrahigh field MR systems operating at 7-tesla need to be compared with 3-tesla.
"Once again, certain advantages of 7 tesla are quite obvious and promising even in the clinical setting. However, the 3-tesla sports car mutates into a 7-tesla Formula One racing car, which makes daily use even more challenging," they wrote.
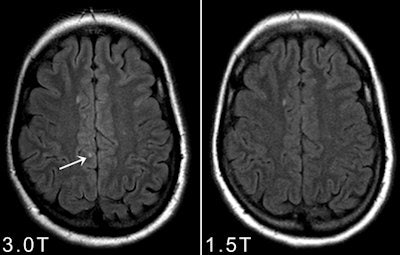 Axial 1.5-tesla and 3-tesla FLAIR obtained in a patients presenting with a clinically isolated syndrome suggestive of multiple sclerosis. Please note that at 3-tesla one juxtacortical lesion could be identified that was not prospectively scored on the 1.5-tesla images.
Axial 1.5-tesla and 3-tesla FLAIR obtained in a patients presenting with a clinically isolated syndrome suggestive of multiple sclerosis. Please note that at 3-tesla one juxtacortical lesion could be identified that was not prospectively scored on the 1.5-tesla images.Furthermore, a direct comparison of different magnetic field strengths in terms of diagnostic accuracy is almost impossible. The physical changes occurring when moving to higher magnetic field strength (e.g., tissue relaxation times, specific absorption rate) make it crucial to adjust the pulse sequences and MR protocol in terms of repetition and times, but also require a choice between spatial and temporal resolution to achieve comparable conditions, the authors elaborated. It is arguable whether these conditions are really comparable in terms of a side-by-side 1.5- versus 3-tesla comparison.
It is important to realize there are other factors that substantially contribute to image quality, such as coil technology, field homogeneity, and multitransmission technology. According to Wattjes and Barkhof, differences in image quality and MR performance can even be observed among MR systems of different vendors operating at the same field strength.
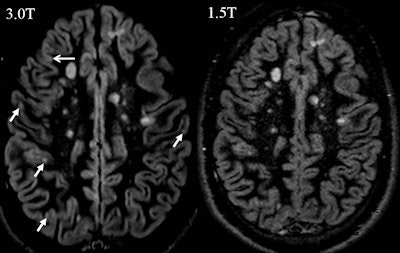 Axial double inverison recovery images at 1.5-tesla and 3-tesla in a patient with multiple sclerosis. Please note that at 3-tesla more cortcial gray matter lesion can be identified.
Axial double inverison recovery images at 1.5-tesla and 3-tesla in a patient with multiple sclerosis. Please note that at 3-tesla more cortcial gray matter lesion can be identified."We should ask ourselves whether it is necessary and useful to formally test all possible differences in terms of diagnostic accuracy between both field strengths. Advantages and disadvantages of higher magnetic field strengths are well known and incontestable. The higher SNR at 3 tesla allows imaging at a higher spatial resolution and the application of parallel imaging techniques as well as routine use of 3D sequences," they wrote.
"It has been conclusively shown that 3 tesla shows more (small) inflammatory white and gray matter lesions and offers a better visualization of smaller arterial branches on time-of-flight and contrast-enhanced MR angiography. Despite the fact that this might not lead to an earlier diagnosis of multiple sclerosis, or an earlier detection of aneurysm or vessel malformation with significant therapeutic consequence, (neuro)radiologists would opt for the better image quality if this came at the same cost and level of safety, because it makes the reading procedure easier and more reliable," the authors added.
This is true even for standard clinical examinations but becomes even more obvious for advanced and quantitative MR methods substantially benefiting from improved SNR, such as MR spectroscopy, perfusion MR, and fMRI, they pointed out. Studies dealing with these methods were almost exclusively performed in the research setting, and in particular, comparative studies in the clinical setting using these techniques are lacking.
"The major question is under what circumstances are the increased costs of 7 tesla and the inherent limitations in coverage and safety outweighed by diagnostic benefits?" concluded Wattjes and Barkhof.









![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)






