
Honesty generates trust in patient-doctor relations, but when mistakes are made, radiologists must distinguish between the legal requirement for duty of candour and the preference for openness, according to U.K. Royal College of Radiologists (RCR) President Dr. Nicola Strickland.
During a session on 13 September at the RCR's annual meeting in Liverpool, she highlighted circumstances in which radiologists were obliged by law to disclose mistakes in a formal duty of candour process (a healthcare professional's obligation to notify patients of adverse events), when informal openness must be encouraged, and, conversely, when discretion was the best course of action for the sake of the patient. She also highlighted how truthfulness from the start can help avert being sued.
 RCR President Dr. Nicola Strickland.
RCR President Dr. Nicola Strickland."Many clinicians feel compelled blindly to apply the letter of the law, regardless of the futile stress it will cause patients," Strickland told AuntMinnieEurope.com after the congress. "Openness can avoid court cases, but we should only inform patients compassionately when it will foster trust, not officiously or systematically across the board, out of fear."
Between 1996 and 2006, there were 440 claims against radiologists in the U.K., including 199 for missed or delayed cancer diagnoses, she noted. The National Health Service (NHS) paid 8.5 million pounds (9.6 million euros) in damages and 5 million pounds (5.6 million euros) in legal fees for these claims -- money that perhaps could have been spent helping patients in other ways, such as funding radiology trainees or new equipment.
Following the investigation in 2010 into poor care and high patient mortality at Stafford Hospital run by the Mid Staffordshire NHS Foundation Trust, the authorities updated the Health and Social Care Act 2008 with new regulations stipulating that a health service body must act in an open and transparent way with relevant persons in relation to the care and treatment provided to service users. Duty of candour legislation was implemented in 2014.
Duty of candour must be applied when there has been an incident that has resulted in death, serious or moderate harm, or prolonged psychological harm, Strickland noted. Patients, or relevant persons, must be officially informed in person by the clinician, a written apology made, and an investigation into the incident undertaken. However, when a mistake has resulted in no harm, informing the patient is a judgment call.
90 errors per week
From the literature, Strickland extrapolated that around 90 radiological errors, many trivial, are made each week in an average-sized U.K. radiology department.
"It would be ludicrous to undertake 90 openness discussions or duty of candour every week. We must use our clinical judgment to put the welfare of the patient to the fore and choose which misses are notifiable," she said, clarifying that it was the clinician in charge of the case, not the radiologist, who should hold the discussion with the patient.
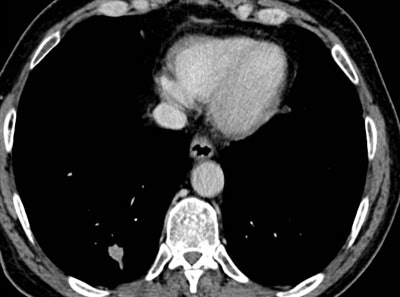
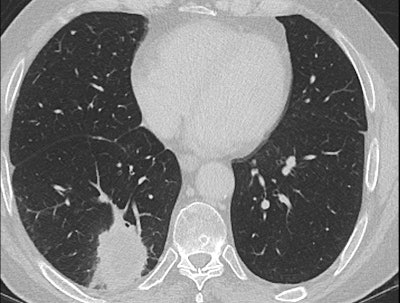
In her Liverpool talk, Strickland showed examples of missed lung cancers. In one case, leading to a duty of candour procedure, the lung bases, visible on a CT scan of the abdomen performed for suspected pancreatic pathology, had not been looked at on lung contrast windows, causing a small right basal lung cancer to be missed (see images above). On a subsequent chest CT scan several months later, the lesion was much bigger, and a second cancer was present in the left upper lobe. A duty of candour was issued because the lung cancer was at a higher stage when it was finally detected, likely leading to a worse outcome for the patient.
Even in cases in which no harm comes to the patient as a result of a delay in diagnosis, openness is the best policy, she noted.
"If the patient were to ask, 'Was the cancer visible on my previous chest x-ray?' and the individual hadn't already been told that it was, this will look as though the doctor was trying to hide this information, which will foster mistrust and damage the relationship," Strickland said.
Inevitability of mistakes
In a work context where acute staff shortages lead to heavy workloads, fatigue, and constant interruptions from clinicians and other staff, perceptual and interpretative mistakes are inevitable, and these are likely to increase as imaging demand growth combined with the rapid advance of technology makes workloads ever more heavier and complex, Strickland continued.
The duty of candour letter
Dear Mr. X,
As we discussed in consultation this morning, I am very sorry that your CT scan undertaken to investigate pain in your abdomen and pancreas on Xth April 2014 did, in fact, show a small nodule in the bottom of the right lung. It is likely this was the early stage of the squamous cell cancer that we have now found in the right lung and are planning to treat.
A full and thorough investigation will be carried out by XXX Hospital as to why this small nodule was overlooked on the CT scan and why the scan was not flagged to the lung cancer team.
Again, I do apologize that this was missed, and I am very confident that we have a good plan for your treatment moving forward.
Kind regards,
XXX
A key part of the solution is to bolster the U.K.'s radiological workforce. Without more radiologists, the entire healthcare system will collapse since radiology is essential for almost all medical diagnoses, she said, noting that 500 U.K. radiology staff posts remain vacant.
Double reporting every imaging study would lower the number of reporting errors, but since a vast number of x-rays and scans in the U.K. are not even single reported in a timely fashion, this is not a practical solution, she said.
Mistakes in radiology are often multifactorial and may include omissions or actions earlier up the chain, such as the requester failing to provide an adequate patient history, particularly when there is a known previous history of cancer. The absence or inaccessibility of the patient's previous imaging also can lead to diagnostic errors.
However, unlike most other specialists, radiologists will always be legally vulnerable; they make actionable diagnoses that may affect patient management, leaving a trail of evidence which can be judged for accuracy at a later date. There may be no documented evidence proving a clinician missed a clinical sign such as a breast lump in an earlier checkup, but the same patient's routine mammogram showing malignant microcalcifications will be scrutinized in cases of alleged radiological error.
Educating patients
Strickland thinks that the public needs to be educated about the whole nature of radiological diagnosis, which is not a binary result like a blood test. Many diagnoses can only be confirmed as more clinical evidence accrues, and the disease process reveals itself.
She also described how outcome and hindsight biases affect judges, juries, and expert witnesses in medicolegal cases. A poor patient outcome will understandably sway the court to be on the patient's "side" out of sympathy, according to Strickland, while hindsight bias is the 20/20 vision everyone has in retrospect for spotting tiny lung cancers on early scans, once the subsequently detected lung cancer is pointed out on later imaging.
Radiologists' defense lies in educating the public and also in publishing figures of error, keeping their education up-to-date, continuous self-testing, and peer review, Strickland said.
"If you make a one-off mistake, it doesn't make you a bad doctor. We must try to foster the same 'no blame' culture as seen in the aircraft industry," she concluded.



















