Failure to communicate to the clinician significant abnormal findings in diagnostic tests can result in potentially life-threatening consequences for the patient, particularly if those findings are unexpected. To address this problem, radiologists at Dublin's Mater Misericordiae University Hospital (MMUH) have implemented a system for making results' urgency uniformly understandable at first glance and the checking of reports automatically trackable.
Introduced six months ago, tailored computer software puts identifiers on lab results that show abnormal or significant findings through their number values. The results are then sent to a file and a "read receipt" type protocol is activated when the clinician has checked them. The scheme highlights that the remit of radiologists increasingly influences patient management. Radiologists can no longer simply interpret images and produce reports; they must ensure patient safety is supported through every stage of the process, including good reporting practice.
The risk of potential serious adverse events resulting from report communication failures can be identified, according to Dr. Leo Lawler, a consultant interventional radiologist at MMUH. In the literature, as many as 30% of all diagnostic tests ordered are not being checked by the ordering clinicians. This is due to several factors, including patient transfer between teams and lack of follow-up. In addition to this, nonuniform, blandly narrative reports were not specifically highlighting unexpected significant findings in a way that grabbed the attention of the clinician, he explained.
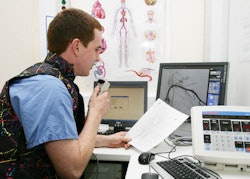 Dr. Paul Foran, a specialist radiology registrar, carries out his reporting duties at MMUH. Image courtesy of Dr. Leo Lawler.
Dr. Paul Foran, a specialist radiology registrar, carries out his reporting duties at MMUH. Image courtesy of Dr. Leo Lawler.
The customary lack of numerical values, and the unstructured prose-dependent style of radiology reports, made developing an automated system for radiological reporting slightly more problematic. To overcome this, a color word code is now included in the write-up of reports, Lawler noted. Automated triage and "read" verification of radiology reports should be live in the next couple of weeks.
In urgent cases, code "red" will tell the computer to flag highly significant findings requiring immediate attention such as cancer, aneurysm, pulmonary embolism, and abscess, which can cause harm if not acted upon. The program will recognize and tag code "blue" reports as findings needing attention sooner rather than later but that won't likely worsen during a short wait to follow-up. The default setting for normal findings without a code word will leave reports unmarked by the new program. This indicates that no further action is suggested.
"It doesn't matter how simple the system is, as long as one is in place. It could even be a paper system but with a uniform approach and an agreed [upon] universal vernacular to communicate to physicians a finding that needs attention," Lawler said, adding that the hospital has relatively simple IT infrastructure, with no PACS at present.
Patient safety is the linchpin behind the action, not standardized reporting for its own sake. Any system should not remove existing communication methods that serve as "safety net" solutions and that might include calling physicians, sending emails, and even telling the patients themselves.
"Radiologists need to define the limits of their duties and create a system to fulfill these duties in a demonstrable manner. Ten years ago we read the test and reported our findings. When radiologists started getting the blame for adverse events, our responsibilities grew. Now our remit is very different," Lawler said.
A clear "paper" or "electronic" trail proving that radiologists have communicated results in a correct and meaningful manner, and that the clinicians have received the information and acted on it (or not, as the case may be), will confer greater responsibility on those ordering tests and may change ordering practice. Such systems will consequently minimize the potential for court cases against radiologists.
Initial resistance to the system at the Dublin hospital stemmed from fear of such a paper trail being used against doctors. However, six months on, most staff members have now accepted its benefits: peace of mind, knowing that all lab reports have been communicated -- and checked -- appropriately, and perhaps more significantly, a more considered approach to test ordering.
By summer of this year, doctors at MMUH will know what difference the system is making to imaging, and it is hoped the new influx of doctors in July will consider it standard practice.
"This is less about IT and more about mind-set and behavior. Changing behavior requires more than changing a system," Lawler said. "Doctors need to see themselves as stakeholders in a problem and want to protect themselves and the patient."