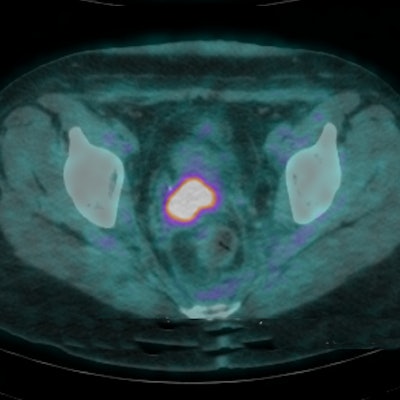
With the help of an established five-point scoring system to assess metabolic response to chemoradiotherapy on FDG-PET/CT scans, U.K. researchers can more appropriately treat and better predict outcomes for patients with locally advanced cervical carcinoma, according to a study published in the April issue of the European Journal of Nuclear Medicine and Molecular Imaging.
Given that the scoring system, coupled with FDG-PET/CT, is helpful in determining survival, its best attribute may be in dealing with patients who are naturally quite concerned about their condition and future.
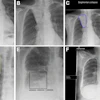
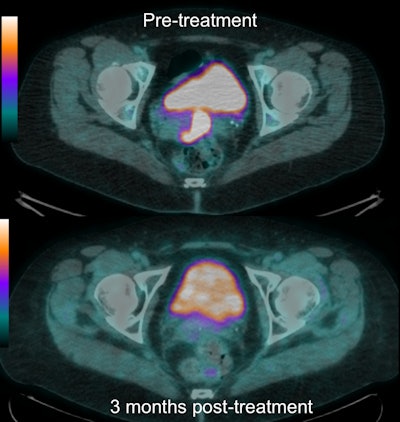 FDG-PET/CT images show shows baseline (top) and follow-up (bottom) results in a patient who had a complete metabolic response (grade 1) in the primary tumor. All images courtesy of Dr. Andrew Scarsbrook.
FDG-PET/CT images show shows baseline (top) and follow-up (bottom) results in a patient who had a complete metabolic response (grade 1) in the primary tumor. All images courtesy of Dr. Andrew Scarsbrook."The PET scoring system is most useful when the clinicians are able to provide reassurance to patients that they have had a very good response to treatment and only have a low chance of relapse," noted lead author Dr. Andrew Scarsbrook, consultant radiologist and nuclear medicine physician at Leeds Teaching Hospitals National Health Service (NHS) Trust. "It is also of value in a small proportion of patients who have unsuspected distant disease detected on the follow-up PET/CT and allows targeted palliative treatment."
Previous experience
Scarsbrook has co-authored several studies on the use of FDG-PET/CT to assess treatment response following chemoradiotherapy. A 2012 study on head and neck cancer patients touted the hybrid modality's high negative predictive value of a complete metabolic response was sufficient to guide treatment management decisions (Clinical Radiology, October 2012, Vol. 67:10, pp. 966-975).
The researchers then investigated the clinical impact of FDG-PET/CT on the management of patients with locally advanced cervical cancer. The group found that when used for staging, the modality had a "major impact on the initial management of approximately one-third of patients" and altered treatment intent and/or radiotherapy planning (Clinical Radiology, December 2015, Vol. 69:12, pp. 1235-1243).
"This work naturally led to an interest in evaluating the utility of FDG-PET/CT for assessing response to chemoradiotherapy in patients with locally advanced cervical cancer," Scarsbrook wrote in an email to AuntMinnieEurope.com.
This retrospective study enrolled 96 consecutive female patients with a mean age of 47 (range of 24 to 75 years) and histologically confirmed locally advanced cervical cancer. The subjects were treated with chemoradiotherapy between February 2011 and April 2014 in Leeds (EJNMMI, April 2017, Vol. 44:4, pp. 581-588).
All the patients received baseline FDG-PET-CT scans (Gemini TF 64, Philips Healthcare) before treatment and a follow-up scan approximately three months after the completion of chemoradiotherapy. The mean time between the end of treatment and the follow-up FDG-PET/CT scan was 98.3 days (range of 60 to 232 days). Of the 96 patients, 79 women (82%) had the scan within three months.
In addition, clinical follow-up consisted of a physical examination six weeks after chemoradiotherapy completion and every three months until two years after therapy. MRI scans also were performed at three and 12 months. If the three-month MRI scan was inconclusive, it was repeated at the six-month mark.
All patients were followed until death or the end of December 2015. The minimum follow-up period for surviving patients was 18 months (range 18 to 54 months) from time of response assessment with FDG-PET/CT.
Disease evaluation
The five-point scoring system to assess response to chemoradiotherapy is in widespread clinical use for patients with high-grade lymphoma. It is referred to as Deauville criteria, because it was first described at an international meeting in Deauville, France, Scarsbrook explained.
In this study, the scoring system was used to rate locally advanced cervical carcinoma based on the following:
- Grade 1 -- No residual FDG uptake within primary tumor and nodes and complete metabolic response to treatment
- Grade 2 -- Focal uptake less than mediastinal blood pool (MBP) activity and likely complete metabolic response
- Grade 3 -- Focal uptake greater than MBP, but less than liver activity, with indeterminate residual uptake
- Grade 4 -- Focal uptake greater than liver activity and consistent with partial metabolic response
- Grade 5 -- Intense focal uptake greater than twice background hepatic activity, with disease progression
"These criteria have subsequently been proven as reliable and robust for use in response assessment," Scarsbrook said. "Our group decided to test the applicability of this scoring method for assessing treatment response in locally advanced cervical cancer, which had not been previously studied to the best of our knowledge."
Based on the scoring scale criteria, 40 (42%) of the 96 subjects exhibited a complete metabolic response from chemoradiotherapy (grade 1 or 2) on post-treatment FDG-PET/CT scans. Of those patients, 38 women (95%) remained disease-free after a minimum follow-up time of 18 months.
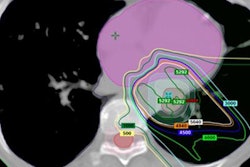
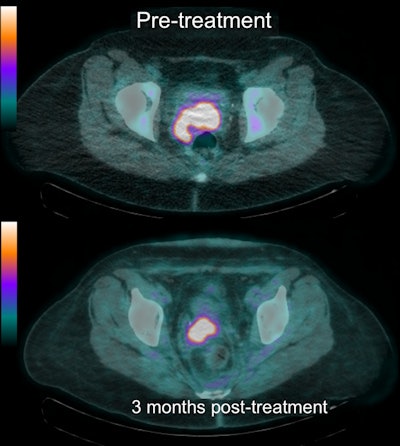 These FDG-PET/CT images show baseline (top) and follow-up (bottom) results in a patient with significant residual (grade 5) uptake in the primary tumor after treatment. The finding was confirmed to represent residual tumor histologically and the patient underwent successful salvage surgery.
These FDG-PET/CT images show baseline (top) and follow-up (bottom) results in a patient with significant residual (grade 5) uptake in the primary tumor after treatment. The finding was confirmed to represent residual tumor histologically and the patient underwent successful salvage surgery.There were 24 patients (25%) who had an indeterminate residual primary or nodal uptake (score 3) after treatment, of whom eight patients (33%) relapsed during follow-up. In addition, 17 women (178 %) had significant residual uptake (score 4), with 11 cases (65%) of cervical cancer relapse. Sadly, 15 patients (16%) demonstrated progressive disease (score 5) following treatment; one patient (7%), however, had a false positive result.
Based on the results, FDG-PET/CT achieved overall sensitivity of 94% in predicting residual or recurrent disease. Specificity was 62%, compared with positive predictive value of 59%. Negative predictive value reached 95% and overall diagnostic accuracy was 74%.
Survival rates
Relative to survival outcomes, 35 patients (36%) had their cancer progress during the follow-up period. The mean time to cancer recurrence was 7.3 months (range 2.6 to 38 months). In all, 27 patients died during the follow-up period. The average time to death was 16.9 months, with a range of 7.8 to 33.1 months.
In adapting the results to the clinical setting at Leeds, Scarsbrook said the five-point scoring system is most useful in the setting of complete metabolic response (grade 1 and 2), and clinicians can reassure patients they have had a very good response to treatment and have a low chance of relapse.
 Dr. Andrew Scarsbrook of Leeds Teaching Hospitals NHS Trust.
Dr. Andrew Scarsbrook of Leeds Teaching Hospitals NHS Trust."In the other groups with residual uptake, the combination of MRI and PET can be useful for guiding optimal management, but often it is difficult to distinguish between slow to resolve post treatment changes and residual disease, and repeat imaging after an interval may be required," Scarsbrook said.
The researchers cited several limitations of the study, including the fact the retrospective research was conducted at one institution with a relatively small sample of patients. In addition, not all patients received the same treatment and some patients were not suitable for high-dose brachytherapy.
There is more research on this area from the Leeds group. They also have studied the comparative effectiveness of qualitative response assessment interpretation criteria for MRI and FDG-PET/CT in this clinical scenario. Their results show that dynamic contrast-enhanced MRI parameters may help evaluate early changes in cervical squamous cancer from concurrent chemoradiotherapy.
"A manuscript based on this work is undergoing peer review and will hopefully be published as an original article later this year," Scarsbrook said. "We are also considering future prospective work exploring the safety and efficacy of FDG-PET/CT response driven follow-up after chemoradiotherapy in locally advanced cervical cancer with patients at low-risk of recurrence being offered less intensive follow-up incorporating patient reported outcome measures."