Machines and devices have always been important to radiology, with industry and healthcare professionals collaborating on technological advances. Now another exciting evolution is set to push forward endovascular medicine, virtual attendees heard in a special session at the ECR 2021 Summer Edition on 1 July.
Presenting the possibility of machines taking over some tasks in interventional radiology (IR), expert speakers noted that standardized robotic procedures would improve precision, physician dose, and patient outcomes.
Speaking from personal experience at the session -- entitled "The Rise of the Machine(s) in IR" -- Dr. Florian Wolf, vice director of the division of cardiovascular and interventional radiology at Vienna General Hospital, described his current view of the subspecialty and his vision of the future IR department.
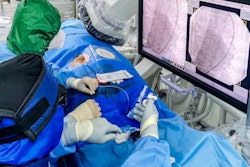
 Demonstrating his virtual reality (VR) helmet and controls, Dr. Florian Wolf believes VR will play a central role in future cardiac interventions. Image courtesy of Dr. Florian Wolf and ESR.
Demonstrating his virtual reality (VR) helmet and controls, Dr. Florian Wolf believes VR will play a central role in future cardiac interventions. Image courtesy of Dr. Florian Wolf and ESR."Every patient and intervention is different. Many things are standardized, but there is always the possibility that something goes wrong, or a new challenge arises during intervention, requiring creativity," he said. "Very often there is not a single right way to do something but different ways to reach your target."
The department deals with a wide range of interventions from brain thrombectomy to lower limb percutaneous transluminal angioplasty (PTA) procedures, as well as nonvascular interventions such as biopsy. The IR doctors work with advanced technology and devices such as angiography machines and 3D visualization. However, while an experienced interventional radiologist will be quicker than a machine in most cases, for a CT-guided liver biopsy or CT-guided microablation, requiring precise targeting of a lesion that can't be seen, the machine can do it better.
Wolf told listeners that he had never felt limited by his own hands, but after trying out Siemens Healthineers' Corindus robotic system, he admitted that he "really loved it."
"It works perfectly for putting in a wire and doing recognition," he said.
Possible fields of application are stroke thrombectomy because of its advantages of standardization, the heart, and PTA procedures in the lower legs, as well as postembolization work. He pointed to how new technological developments that come up in the next few years will open up possibilities for some procedures to be done by a machine instead of a human interventional radiologist, and this would be particularly useful when procedures needed more than two hands.
He also noted that robotic systems would allow for the radiologist to work near but not directly beside the patient when performing stroke thrombectomy, for example, meaning a vast reduction in dose for doctors and obviating the need to wear heavy lead aprons for hours during complex procedures. Such useful developments will come into play over the next five to 10 years, according to Wolf.
Virtual reality
"Today's robotic system is just the start," he noted. "Future developments will really be breathtaking, and one thing that is really fascinating for me is virtual reality."
Wolf has a virtual reality device at home and when he uses it, he can imagine the future of IR.
"3D visualization of the aorta before treatment using this virtual reality tool would be highly helpful. In the future it might be possible to do robotic treatment using a virtual reality system with VR helmet and controls, and do all the movements with my hands in a virtual world with a robotic system at the side of the patient. The potential of VR is very high," he said.
Hanno Herrmann, vice president of business development interventional radiology at Siemens Healthineers, provided insights on the vision behind the company's acquisition of Corindus.
"By building angiography systems, we have always been the eyes of the physician ... and now we want to become your hands," he noted.
The company aims to improve capacity for handling catheters and devices inside a human body or brain and believes Corindus offers the possibility of increasing precision during interventions, as well as shortening complex procedures by automation of movements.
"You can operate the robot from outside and this means you can take off lead aprons and don't have back strain," he said.
He envisages a time when many stroke patients are treated remotely via robotic technology. This will significantly reduce the time to treatment because patient and physician transfer can be eliminated.
Live discussion
Joining session chair Dr. Christian Loewe from the Medical University of Vienna for a live discussion, Dr. Maximilian de Bucourt, a radiologist at the Charité Medical University in Berlin, noted that decisions about the advantages from robotics and from artificial intelligence (AI) would need to be made pertaining to interventionalists' nearby presence outside of the suite, without the need for lead aprons, and remote proctoring from the other end of the world.
He asked Hermann about how the company attached to possible users and their reaction to the system. Herrmann noted that response had been extraordinary and always positive, pointing to a survey during a master class on robotics and robotic neurotreatment that the company had held in May.
The attendees, all neurointerventionalists, were asked whether they would consider remote robotic stroke treatment on themselves or a close relative. The initial response was 60% in favor. By the end of the class and even after the limitations of the system had been discussed, positive responses to the same question had risen to 75%. He revealed that in Canada the system had already undertaken 20 neurointerventions in clinical practice.
Summing up, Loewe said that robotics' biggest area for application would be more to make standardized interventions available in areas where they're not available currently due to a lack of training, with potentially specific targeting of patients in rural areas.
Herrmann noted that this was the case for stroke treatment. In other fields of IR such as chemoembolization, robotics could enable faster procedures with higher precision.
"It might mean that you mark a prostate or liver tumor and then have a robot automatically driving into the optimal embolization location for an ideal landing zone targeted during an embolization procedure," Hermann said. "The application is very broad, and you can also make procedures better, faster, and more precise, improving the quality of existing interventions."