VIENNA - Justification is radiology's trump card in the increasingly tough battle to win back public confidence and reassure patients over the benefits of CT. That was certainly the strong impression given by two opinion leaders at Friday's special focus session at ECR 2013.
Make sure you minimize radiation exposure without compromising image quality or diagnostic performance, recommended Willi Kalender, PhD, from the Institute of Medical Physics at the University of Erlangen in Germany, who barely concealed his frustration and anger over how CT is being portrayed in some areas of the media. He referred to "the crazy debate" linking the use of CT directly to cancer deaths, which is "absolute nonsense," and commented that "some things are really out of control."
 Willi Kalender, PhD, from Erlangen, Germany. Image courtesy of the European Society of Radiology.
Willi Kalender, PhD, from Erlangen, Germany. Image courtesy of the European Society of Radiology.Don't forget to estimate organ and effective dose and include them in your reports, and though it's vital to keep the ALARA (as low as reasonably achievable) principle in mind, keep stressing the benefits of radiology, Kalender noted.
"The benefit-to-risk ratio has to be as high as reasonably achievable," he said. "AHARA is the goal!"
Specific dose estimates for a patient, scanner, and protocol can now be provided with high accuracy, even in pediatric exams, but manufacturer cooperation is often required to obtain data on filtration and other relevant information. This is of great interest for research projects, but is not indicated for routine use, explained Kalender, who disclosed that he is a consultant to Siemens Healthcare and founder, shareholder, and CEO of CT Imaging.
Focusing on clinical practice, Dr. Catherine Owens, a cardiothoracic radiologist and reader in radiology at London's Great Ormond Street Hospital (GOSH) said the key points are to set protocols according to individual needs, make sure images are fit-for-purpose, and strike a balance between optimal image quality and radiation dose.
In cases of fluoroscopic intervention, it's important to bear in mind that the radiologist achieving the lowest patient dose will receive the lowest professional dose. Aim for a short fluoroscopy time, use pulsed fluoroscopy, take a low number of high-quality exposures, ensure optimal parameter selection, and build up your knowledge of specific equipment, she advised.
Other factors to consider are the best position for workers inside the room, modifying the technical parameters and effects on exposure, and use of protective devices to minimize dose to critical organs.
 Dr. Catherine Owens from London. Image courtesy of the European Society of Radiology.
Dr. Catherine Owens from London. Image courtesy of the European Society of Radiology.To be justifiable, the benefit of an exam must always outweigh the risk, according to Owens. The decision about whether to proceed should be a strictly clinical one taken by a multidisciplinary team. Strict referral criteria must be followed, and in pediatric radiology, ultrasound is the first line of investigation and abdominal requests should be referred to MRI.
"Check the date of the patient's last CT exam," Owens noted. "It's always very disappointing to see the level of repeat scans in some institutions."
It is widely accepted that the risks from ionizing radiation are greater in children than in adults because their tissues are more radiosensitive, and the prospect of a longer life means they're more likely to develop associated problems. Worryingly often, however, adult scanning parameters are used in pediatric imaging and, unlike plain films, CT images never look overexposed.
Additionally, children receive a higher effective dose due to the distribution of absorbed energy over smaller area and organs. Furthermore, there is a lack of adequate guidelines and protocols from manufacturers, and patients with a wide age and weight range are being dealt with, she said.
At GOSH, CT optimization is achieved by following the ALARA principle, establishing specific pediatric weight- or diameter-based scanning protocols, limiting coverage to the area under investigation only, reducing kVp (e.g., 80-100), applying dose modulation, and ensuring the patient is in the isocenter, where dose and image quality are optimal.
Remember that prospective ECG-gated cardiac imaging provides similar radiation burden as nongated studies but with improved image sharpness, she added. The advent of second-generation dual-source CT and 320-detector-row CT has reduced the need for ECG triggering.
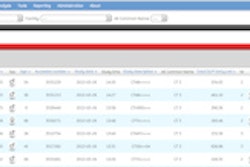
Kalender elaborated on the common approaches to assessing patient dose in clinical CT today: CT dose index volume(CTDI) and dose-length product (DLP) values, which are essential to set dose reference levels and of interest for comparison purposes, but they do not represent patient dose; DLP to effective dose (DLP-to-E) conversion, which is neither patient- nor scanner-specific and does not provide organ dose values; and programs based on pretabulated data, e.g., ImpactDose, ImPACT CT patient dose calculator in the U.K., and CT-Expo in Germany.
In patient-specific dose estimates based on the CT image data instead of solely phantoms, total scatter has to be accounted for (complete body representation is necessary), dose to organs has to be assessed (organs have to be identified and segmented), organ and effective dose values should be estimated for the patient, scanner and scan protocol should be listed, and results should be available without long waiting times and in a comprehensible format, he concluded.
Originally published in ECR Today on 9 March 2013.
Copyright © 2013 European Society of Radiology