The modeling and mimicking of surgical procedures that compare postoperative strain patterns on stents will be immensely valuable as the market grows for transcatheter cardiac valve device implantation, according to Dr. Andrew Taylor, a professor of cardiovascular imaging at London's Great Ormond Street Hospital (GOSH).
"The use of functional imaging systems which can demonstrate pre- and postoperative stent implantation -- coupled with the advent of the hybrid operating room that is large enough to accommodate multidisciplinary teams of imaging experts and surgeons, together with sophisticated imaging equipment -- is likely to be the way forward," he told delegates at the British Institute of Radiology (BIR) President's Conference in London.
About 20% of patients who have percutaneous pulmonary valve implants (PPVI) suffer from stent fractures, and it is important to understand why this happens. Lab tests can suggest that the valves would work well, but the reality is often different.
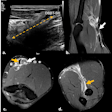
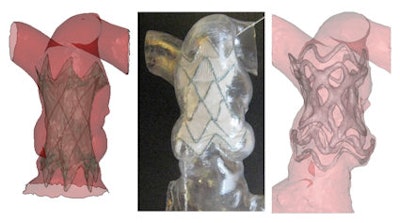 Implantation of a new percutaneous pulmonary valve device into a dilated pulmonary artery. Left: Virtual implantation on the computer. Middle: Implantation into a rapid prototyping model. Right: 3D CT image following actual device implantation. Note the excellent prediction of the device position following the trial implantation into the rapid prototyping model. Images courtesy of Dr. Andrew Taylor.
Implantation of a new percutaneous pulmonary valve device into a dilated pulmonary artery. Left: Virtual implantation on the computer. Middle: Implantation into a rapid prototyping model. Right: 3D CT image following actual device implantation. Note the excellent prediction of the device position following the trial implantation into the rapid prototyping model. Images courtesy of Dr. Andrew Taylor."A lot of testing that is currently done on cardiac devices is either tested on the bench, in the lab, or with animals, but the crucial piece of human information when the device is taken from these developmental stages is extremely important and this is where imaging comes into its own," he noted.
During the past seven years, Taylor has worked on the Melody transcatheter pulmonary valve (Medtronic, Minneapolis, MN), a cardiac device for percutaneous pulmonary valve implantation approved by the U.S. Food and Drug Administration on 25 January 2010. The device is made from bovine jugular vein valve, which is sewn into a small metal stent (scaffolding). The valve is indicated for use in patients with congenital heart defects involving malformation of the right ventricular outflow tract. More than 3,200 of these procedures have been performed at GOSH, and cardiovascular imaging has proved vital for confirming device efficacy and providing feedback to surgeons in order to reduce negative consequences.
Taylor became involved in this work partly because of his investigations into the causes of stent fractures in humans. He thought fractures may be partly due to the fact stents are being implanted into dynamic circulations, coupled with lots of motion where the valves were being inserted, and also because of irregularities in the shape of vessels due to a patient's anatomy. He highlighted this by showing images of 12 patients between the ages of 10 and 15 with Tetralogy of Fallot, who had all been operated on as neonates and whose anatomy was all completely different.
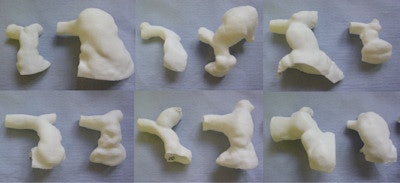 3D models of the pulmonary arteries built from MRI data from 12 adult patients with Tetralogy of Fallot, who all underwent repair during infancy. Note the huge range in anatomy that develops over time.
3D models of the pulmonary arteries built from MRI data from 12 adult patients with Tetralogy of Fallot, who all underwent repair during infancy. Note the huge range in anatomy that develops over time.Taylor described a virtual implantation of a stent, and showed how human data and modeling using techniques such as this can help to predict where stents may fracture. Demonstrating these virtual techniques in this way by using imaging provides physicians with greater knowledge about the predictability of stent fracture, he noted. Also, it is now feasible to create realistic models using rapid prototyping based on computational modeling and 3D datasets using MR and CT. The images can be run through a 3D printer that produces polymer images built up sequentially in layers, providing excellent 3D anatomically precise models. These new imaging methods have allowed Taylor and his team to identity patients who are suitable for this new PPVI technique.
"When looking at total numbers of patients presenting to a department who need valve replacements, only 15% of patients who have been selected through imaging can actually undergo this new percutaneous valve implantation treatment, and this means 85% of patients are still undergoing operations or have metal stenting alone," he said. "This new treatment avoids intensive care stays, costly recuperation, in-patient treatments, and operations."
In the future, Taylor hopes to see a situation where virtual surgery can be performed in the first instance. By using innovative 3D modeling techniques, it may be possible to predict which operations are best for the surgeons. Virtual surgery using 3D imaging provides several options, enabling surgeons to choose which would be most appropriate for their patients.