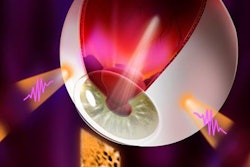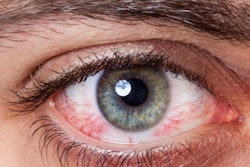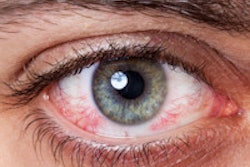
Full awareness of the CT features of orbital trauma, and the potential complications of damage to the eye, makes it possible to diagnose sight-threatening problems before permanent visual loss occurs, according to new research from a leading U.K. hospital group.
Orbital injury is common among polytrauma patients, and worldwide an estimated 1.6 million people have been blinded as a result of orbital trauma, noted radiology registrar Dr. Jane Topple and colleagues from Barts Health National Health Service (NHS) trust and the Royal London Hospitals.
"The diagnostic onus often lies with the radiologist to detect sight-threatening orbital problems in unconscious, intubated patients who cannot be assessed fully at the time of admission," they noted. "A detailed understanding of the anatomy of the orbit aids image interpretation when there are complex patterns of ocular injury."
Ocular injuries together with major trauma are important because they may be easily overlooked at a time when life-threatening injuries may take priority, and vision-threatening injuries may go undetected for hours or even days, they explained. Therefore, significant responsibility lies with the on-call reporting radiologist, who must know about the different types of potential orbital injury and recognize the associated radiological findings to expedite sight-saving and life-saving treatment.
Road traffic accidents and falls from a height are by far the most common causes of orbital trauma. Alcohol consumption is an important risk factor for orbital injury. Young to middle-aged men (ages 21-40) are by far the most likely to present with orbital trauma, Topple and colleagues wrote in an electronic poster that received a Cum Laude award at ECR 2013.
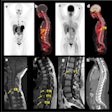
CT is the imaging modality of choice in orbital trauma, particularly in the emergency setting, they continued. Thin-section axial datasets are acquired from dedicated protocols, or retrospective reconstructions can be rendered from the volume CT head dataset. Thicknesses of 0.625 to 1.25 mm are optimal.
At Barts and the Royal London, the CT head study is performed as part of a standardized traumogram incorporating a noncontrast CT head volume-acquisition (from which facial and orbital images can be reconstructed) and cervical spine study followed by a postcontrast chest, abdomen, and pelvis. The hospitals' neuroradiologists strongly advocate the liberal use of multiplanar reformats, including oblique formats.
Ultrasound and MRI studies are useful in the diagnosis of orbital pathology, but they are not appropriate in the imaging of acutely injured unstable patients, according to Topple et al.
The CT imaging features of traumatic intraocular pathologies include hyphema, lens subluxation and dislocation, globe rupture, ocular detachment, and intraorbital hemorrhage.
Hyphema is defined as hemorrhage into the anterior chamber of the globe, and is caused by local disruption of blood vessels in the ciliary body and iris. CT findings include one or more of the following: an increase in the attenuation of the anterior chamber when compared with the uninjured side; widening of the anteroposterior (AP) distance between the lens and the anterior margin of the globe (this measurement depends on an intact cornea); and decreased volume of the anterior chamber with a reduction in the AP distance if there is associated corneal laceration or iris prolapsed.
"A decrease in the AP distance between the lens and the anterior globe margin is a subtle sign," the authors noted. "If a direct comparison is not made between the injured and uninjured side, this diagnosis can be missed. Subluxation of the lens anteriorly rather than corneal laceration or iris prolapse may also lead to a decrease in the AP distance."
Rapid equatorial expansion of the globe can lead to disruption of the zonular fibers that hold the lens in position. The lens will then sublux or completely dislocate out of its normal position. This injury is typically secondary to blunt force trauma and is often associated with orbital wall fractures. Subluxation is more common than dislocation. The iris tends to limit anterior dislocation, and dislocation of the lens in the posterior direction is more commonly identified, they added.
CT may demonstrate an abnormal position or angulation of a hyperdense lens. Alternatively, the lens may not be visualized at all, as in cases of lens rupture. Spontaneous lens dislocation associated with connective tissue disorders such as Ehlers-Danlos Syndrome should be suspected if bilateral dislocation is evident in the absence of a history of trauma, the group recommended.
Globe injury (open-globe injury) may occur if there is laceration or perforation of the globe with leakage of vitreous humor. This is a sight-threatening injury, the authors stated. In cases of blunt trauma, globe rupture is more likely to occur at the insertion points of the ocular muscles where the sclera is thinnest. It is often difficult to assess these patients clinically and they should be referred for CT scanning. Unfortunately, the sensitivity of CT for the diagnosis of open-globe injury is limited, and varies between 56% and 77%, they explained.
CT imaging may demonstrate asymmetrical alteration of globe contour, asymmetrical reduction of globe volume known as the flat-tire sign, stranding in the retrobulbar fat plane, scleral discontinuity, asymmetric alteration in anterior chamber depth, intraocular air, and an intraocular foreign body.
Etiologies of penetrating injury include occupational accidents (e.g., glass workers, carpenters, steel factory workers, and builders), criminal assault and self-inflicted trauma (e.g., stabbings and gunshot wounds), sports injury (e.g., racket sports, hockey, mountain-biking, and shooting), motor vehicle accidents (e.g., glass and metal fragments injuring drivers, passengers, and bystanders), and warfare and terrorist attack injuries (e.g., penetrating shrapnel related to blast injuries), they concluded.